For many women in their late 40s and early 50s, the experience of "brain fog"—that persistent, hazy inability to retrieve a simple proper noun or focus on a standard task—is often dismissed as a byproduct of a busy life. However, for an increasing number of women, this cognitive decline is not a symptom of general burnout, but a profound physiological transition: menopause.
Reviewed by experts Brian St. Pierre, MS, RD, and Helen Kollias, PhD, the emerging consensus among medical professionals suggests that we have long misunderstood the systemic impacts of the menopausal transition, often misdiagnosing it as clinical depression or chronic fatigue.
The Invisible Struggle: A Personal Chronology
The narrative of the menopausal transition often begins with subtle, maddening lapses. One woman describes it as having her thoughts buried under "a pile of garbage."
"I’d sit in front of my computer screen, stare at a document, and will myself to do something constructive," she recalls. "Everything seemed hazy, like those first few moments in the morning when you’re awake enough to turn off the alarm but too sleepy to do basic math."
For two years, this individual navigated a revolving door of medical professionals. She was prescribed a succession of antidepressants and sleeping pills, all of which exacerbated her sense of being a "zombie." It was only during a routine gynecological exam, when she happened to mention vaginal dryness, that a physician connected her cognitive decline, mood swings, and insomnia to the hormonal shifts of menopause. Within days of beginning prescribed estradiol and progesterone, her mental clarity returned. The "sludge" had lifted.
Anatomy of the Menopausal Transition
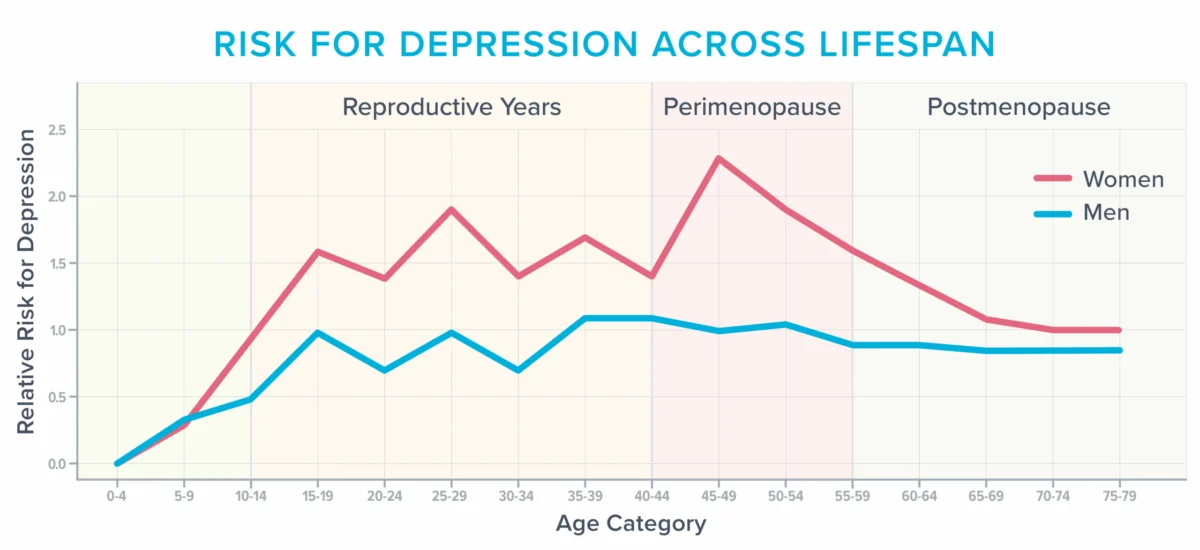
It is critical to clarify that menopause is not a disease; it is a life stage. Defined as occurring 12 consecutive months after a woman’s final period, it marks the transition to a postmenopausal state. During the years leading up to this, hormone levels—specifically estrogen—fluctuate and decline.
While weight gain and reduced libido are the most publicized symptoms, the American College of Obstetricians and Gynecologists (ACOG) notes that roughly 40 percent of women report increased irritability, anxiety, and profound fatigue. Crucially, this period represents a window of heightened vulnerability for the onset of clinical depression, particularly in those with a prior history.
The Role of Vasomotor Symptoms
While life stress, aging, and career pressures certainly contribute to cognitive strain, a significant and often overlooked trigger is the "hot flash." Known clinically as vasomotor symptoms, these events involve the constriction or dilation of blood vessels, triggered by a "wonky" hypothalamus that incorrectly regulates body temperature.
When a hot flash occurs, the body releases norepinephrine and cortisol. This hormonal spike increases heart rate and blood pressure, often leaving the woman feeling faint, anxious, or exhausted.
Scientific Evidence: Beyond the "Inconvenience"
For decades, medicine treated vasomotor symptoms as mere social inconveniences. Current research is forcing a paradigm shift. Recent studies utilizing MRI technology have identified a correlation between frequent hot flashes and the presence of "whole-brain white matter intensities"—patchy areas in the brain that serve as markers for potential future cognitive decline.

Research involving 226 women found that those experiencing the most frequent hot flashes exhibited a higher abundance of these brain lesions. Furthermore, a three-year study of 492 women determined that frequent hot flashes correlate with unhealthy vascular changes, specifically an impaired ability of blood vessels to dilate and support brain oxygenation.
The Sleep-Brain Connection
The cycle of nocturnal vasomotor symptoms—night sweats—creates a secondary, catastrophic impact on the brain. Many women do not realize their sleep is being disrupted by hot flashes; they simply wake up. These repeated, unrecognized micro-awakenings prevent the brain from consolidating memories, metabolizing metabolic toxins, and maintaining the connectivity of the hippocampus.
The Diagnostic Dilemma
The medical community currently faces a crisis of diagnosis. Standard tools, such as the PHQ-9 depression scale, often capture symptoms that overlap perfectly with menopausal sleep deprivation: fatigue, difficulty concentrating, and loss of interest in activities.
"80 percent of medical residents admit they feel ‘barely comfortable’ talking about menopause," notes Dr. Jerrold H. Weinberg, a Michigan-based specialist. This lack of specialized training leads to "defensive medicine," where doctors avoid prescribing Hormone Therapy (HT) due to outdated fears regarding safety.
Re-evaluating Hormone Therapy
The modern medical perspective on hormone therapy has evolved. Research indicates that for women under 60—or those within 10 years of their final period—the benefits of hormone therapy often outweigh the risks. Beyond alleviating cognitive fog and insomnia, HT can offer protective benefits against osteoporosis and Alzheimer’s disease.
Advocating for Your Health
Navigating the healthcare system requires proactive engagement. Experts recommend the following steps:
- Seek Specialists: Look for practitioners certified by the Menopause Society.
- Document Data: Use apps or journals to track sleep, mood, and hot flash frequency. Data prevents the "hazy" recollection that often occurs during a doctor’s appointment.
- Shared Decision-Making: Ask your doctor directly: "What are the risks versus benefits for me, specifically, regarding hormone therapy?"
Holistic Strategies for Brain Health
While medical intervention is often necessary, lifestyle strategies provide a vital secondary layer of defense.
- Creatine Supplementation: Research suggests that 5 to 7 grams of creatine monohydrate daily can assist in countering mental fatigue and supporting cognitive function during periods of sleep deprivation.
- Circadian Alignment: Prioritize morning sunlight exposure to regulate the internal clock, which improves both sleep quality and daytime alertness.
- Adjusting Exercise Intensity: Middle age is not the time to push through chronic exhaustion. Swap high-intensity interval training (HIIT) for zone 2 cardio or restorative yoga on days when sleep has been compromised.
- Cognitive Behavior Therapy for Insomnia (CBT-I): This is the gold-standard psychological intervention for sleep, focusing on behavioral restructuring rather than medication.
- Nutritional Support: Adopting a Mediterranean or MIND diet provides the circulatory support necessary to protect brain blood vessels. Nitrate-rich foods like beets and dark leafy greens can assist in temporary blood vessel dilation.
Implications: A New Perspective on Aging
The experience of menopause, while undeniably difficult, serves as an unintended "existential audit." When the biological capacity to "do it all" shifts, women are forced to evaluate their priorities.
"Before going on hormones," one woman notes, "I was forced to ask: Do I really need to be doing this?"
By shedding unnecessary responsibilities, setting firmer boundaries, and utilizing modern medical support, the menopausal transition can be reclaimed. It is not merely a period of loss, but a period of profound re-calibration. As the medical community catches up to the reality of the female experience, women are increasingly finding that the "fog" is not an inevitable decline, but a temporary state that can be managed, understood, and ultimately overcome.