Breast cancer remains the most formidable health challenge facing women globally. According to the latest data from the World Health Organization (WHO), the year 2022 saw approximately 2.3 million new diagnoses and 670,000 lives lost to the disease. Despite significant advancements in oncological science—ranging from targeted therapies to improved surgical techniques—a critical, persistent obstacle remains: the management of aggressive, fast-growing subtypes that resist standard treatment protocols. Clinicians are frequently hindered by a lack of predictive diagnostics, leaving a void where precision medicine is needed most.
A transformative new research initiative, the Biomarker Research Integrating Data of Glyco-Immune Signatures and Clinical Evidence in Breast Cancer (BRIDGE), has launched to address this diagnostic and therapeutic gap. By decoding the complex biological "language" between tumors and the immune system, the BRIDGE project aims to pioneer a new generation of biomarkers capable of transforming how we monitor and treat high-risk breast cancer.
The Landscape of the Challenge: Why Aggressive Tumors Persist
The complexity of breast cancer lies in its heterogeneity. No two tumors are identical, and even within a single patient, cancer cells can evolve, mutating to evade both the body’s natural immune defenses and pharmacological interventions.
The Diagnostic Gap
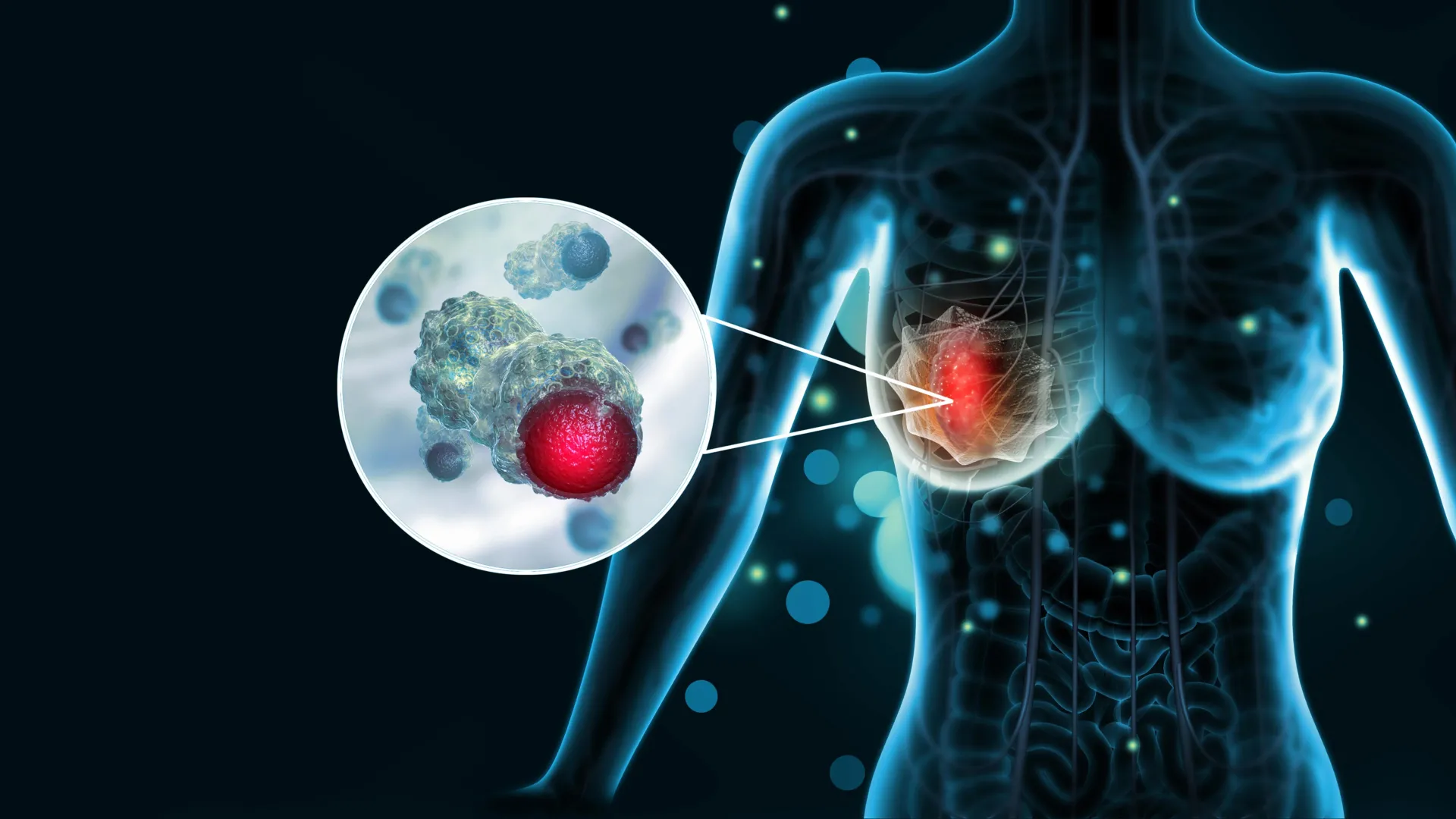
Currently, doctors rely on established clinical markers—such as estrogen receptor (ER), progesterone receptor (PR), and HER2 status—to categorize breast cancers. While these markers are life-saving, they do not tell the full story. For patients with aggressive phenotypes, these standard diagnostics often fail to predict how a tumor will behave over the coming months or how it will respond to emerging immunotherapies. The BRIDGE project posits that the answer lies not just in the cancer cells themselves, but in the "glyco-immune" landscape—the complex sugar-coated molecular signals that dictate how a tumor interacts with its environment.
Chronology of the Initiative: From Laboratory Concept to Clinical Validation
The inception of the BRIDGE project follows years of foundational research at the Instituto de Tecnologia Química e Biológica António Xavier (ITQB NOVA) of the NOVA University of Lisbon.
- Phase I: Discovery (2020–2023): Researchers at the Advanced Cell Models laboratory, led by Catarina Brito, identified specific molecular communication pathways between tumor cells and the immune system. They observed that tumors often "mask" themselves using specific surface molecules to avoid destruction by immune cells.
- Phase II: Strategic Partnership (2024): Recognizing the need to translate these findings into clinical utility, ITQB NOVA formalized a partnership with the Portuguese Institute of Oncology (IPOFG—Instituto Português de Oncologia de Lisboa Francisco Gentil). This alliance bridges the gap between fundamental laboratory science and bedside application.
- Phase III: Funding and Launch (2025): The initiative was selected as part of the iNOVA4Health Lighthouse Projects (LHP) 2025 program. With a two-year funding window and a €75,000 grant, the project has officially entered its validation phase, where laboratory theories will be tested against real-world patient samples.
Decoding the Tumor Microenvironment
To understand the ambition of the BRIDGE project, one must understand the "tumor microenvironment." A tumor is not a solitary entity; it is a complex ecosystem composed of cancer cells, blood vessels, immune cells, and extracellular matrix structures.
The Role of Glycans
The project focuses specifically on glycans—complex sugar structures that coat the surface of every cell. In the context of cancer, these glycans act as a "camouflage," effectively signaling to the immune system that the tumor is a normal part of the body, or worse, sending "don’t attack" signals to immune cells that would otherwise eliminate the threat.
By mapping these glyco-signatures, the researchers hope to identify specific biomarkers that can be measured in blood or tissue samples. These biomarkers would serve as a "real-time dashboard" for clinicians, providing a snapshot of the tumor’s current state and predicting its future trajectory.
Official Perspectives: Translating Science into Solutions
The strength of the BRIDGE project lies in its collaborative ethos. By marrying the technical expertise of the ITQB NOVA with the clinical infrastructure of the IPOFG, the project ensures that the science remains grounded in patient needs.
Catarina Brito, leader of the Advanced Cell Models laboratory, emphasizes the shift toward clinical relevance. "We have previously identified how tumors communicate with certain cells of the immune system to protect themselves," she explains. "With BRIDGE, we aim to validate these findings using real patient samples and translate this knowledge into clinical applications. Our focus is to find new biomarkers that can contribute to more precise, individualized therapies."
The Role of the IPOFG
The Portuguese Institute of Oncology acts as the project’s clinical backbone. By providing access to anonymized patient samples and clinical history, IPOFG allows the researchers to verify if the "glyco-signatures" observed in the lab are consistent with the actual clinical outcomes of patients. This iterative process—moving from patient sample to lab bench and back to the clinic—is the gold standard for translational medicine.
Supporting Data: Why Biomarkers Matter
Biomarkers are the cornerstone of modern precision oncology. They allow for a transition away from the "one-size-fits-all" model of chemotherapy, which often carries significant toxic side effects.
- Early Detection of Resistance: If a biomarker can predict resistance to a specific therapy, clinicians can switch to a more effective, alternative treatment before the cancer spreads.
- Monitoring Progression: Regular testing of biomarkers can provide a non-invasive way to monitor for recurrence, potentially replacing or supplementing more invasive biopsies.
- Immune System Priming: If researchers can identify the molecules tumors use to hide, they can develop targeted therapies that "unmask" the tumor, allowing the patient’s own immune system to finish the job.
With global cancer costs rising, the cost-benefit analysis of such diagnostic tools is significant. Identifying a patient’s specific biomarker profile early could save healthcare systems millions in unnecessary treatments that were destined to fail, while significantly improving the quality of life for the patient.
Implications: The Future of Personalized Care
The implications of the BRIDGE initiative extend far beyond the laboratory. If successful, the project will lay the groundwork for a new diagnostic category in breast cancer care.
Moving Toward Tailored Medicine
The ultimate goal of the BRIDGE project is the development of a "Personalized Care Roadmap." Imagine a scenario where a patient diagnosed with an aggressive form of breast cancer undergoes a glyco-immune profile test. The results return a specific signature, allowing the oncologist to select a treatment that is known to bypass that specific tumor’s defensive mechanisms. This would represent a fundamental paradigm shift from treating "breast cancer" as a broad diagnosis to treating the "unique molecular identity" of the patient’s disease.
Long-term Impact
While the initial project timeline is set for two years, the researchers anticipate that the findings will create a ripple effect. The methodology used to map these signatures could theoretically be adapted for other aggressive cancers, including pancreatic and lung cancers, which share similar immune-evasion tactics.
Conclusion: A Collaborative Path Forward
The BRIDGE project, supported by the iNOVA4Health Lighthouse Projects (LHP) 2025 program, represents a strategic investment in the future of oncology. With €75,000 in funding and a robust team of scientists and clinicians, the project is well-positioned to tackle the most stubborn aspects of breast cancer biology.
As the team begins the task of validating their glyco-immune signatures, the medical community will be watching closely. In an era where cancer care is becoming increasingly specialized, initiatives that focus on the underlying biological dialogue between tumor and host offer the most promising path forward. By deciphering how tumors communicate and survive, the BRIDGE project is not merely studying cancer—it is learning how to dismantle its defenses, one signal at a time. Through this rigorous, interdisciplinary approach, the researchers hope to turn the tide against aggressive breast cancer, moving the global medical community closer to a future where every patient receives the care they truly need.