By Emily Olsen | May 6, 2026
The American workplace is currently the stage for a high-stakes financial and medical tug-of-war. As the popularity of GLP-1 receptor agonists—drugs originally designed to treat Type 2 diabetes—surges, employers across the United States are grappling with the unprecedented budgetary impact of these high-cost therapies. A new survey from the Business Group on Health reveals that nearly 8 in 10 employers identify these medications as a primary driver of rising healthcare costs, forcing corporate leaders to reconsider how they structure benefits for the coming fiscal year.
The Main Facts: A Financial Paradigm Shift
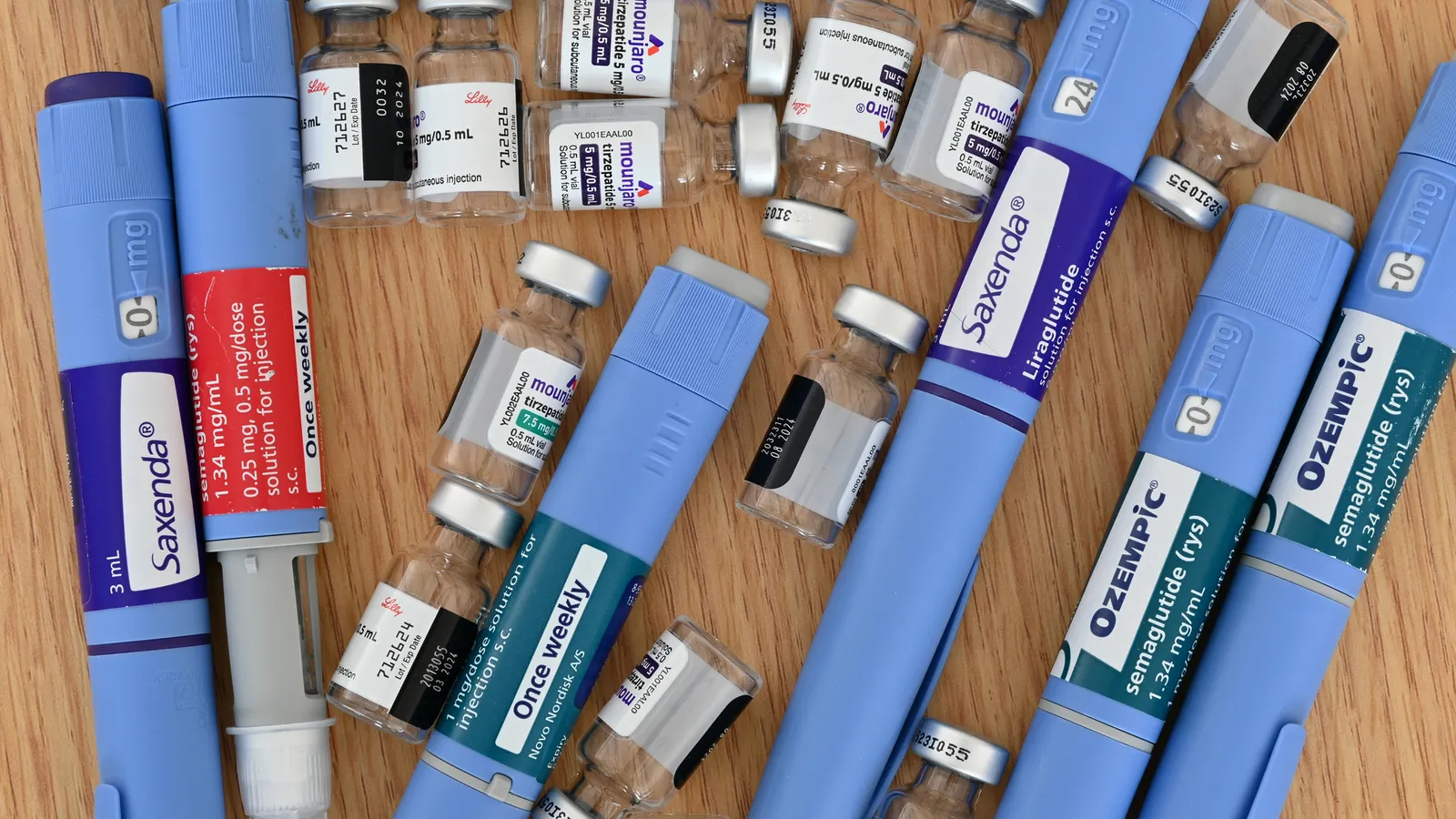
For years, employers have managed healthcare costs through incremental adjustments to deductibles and premiums. However, the introduction of potent weight-loss medications like Wegovy and Zepbound has introduced a level of volatility previously unseen in corporate benefit planning. With list prices hovering around $1,000 per month, the financial burden is no longer a peripheral concern; it has moved into the boardroom.
According to the latest data from the Business Group on Health, which surveyed over 100 of its member organizations earlier this year, the pressure is mounting. The findings are stark: while corporations remain committed to employee wellness, the sheer volume of claims for weight-loss drugs is threatening the long-term financial viability of traditional employer-sponsored health plans. As companies face anticipated double-digit healthcare cost increases, the focus has shifted from "how to offer these drugs" to "how to sustain the budget while offering them."
A Chronology of the GLP-1 Explosion
To understand the current crisis, one must look at the rapid evolution of GLP-1s in the American healthcare market:
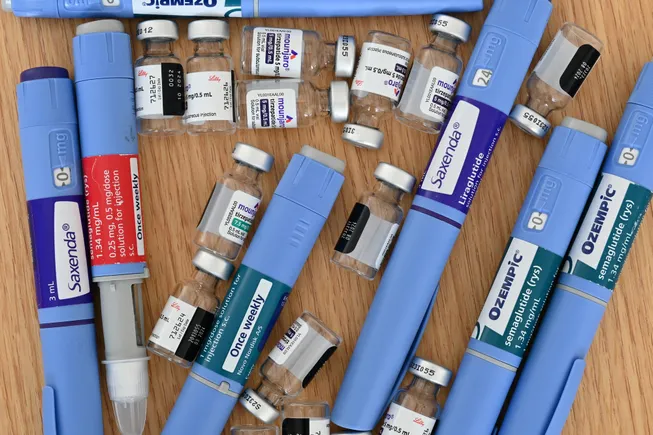
- Pre-2021: GLP-1 agonists, such as Ozempic and Trulicity, were primarily recognized and utilized by patients managing Type 2 diabetes. While expensive, the patient population was relatively contained, and the impact on employer budgets was predictable.
- 2021–2023: Clinical trials and subsequent FDA approvals for higher-dose versions of these drugs specifically for weight management triggered a cultural phenomenon. Social media influence, combined with clinical evidence of significant weight loss, led to a massive surge in demand.
- 2024: The "GLP-1 gold rush" hit the commercial insurance market. Employers reported a significant spike in pharmacy benefit spending, as employees sought coverage for drugs previously considered "lifestyle" medications.
- 2025: Employers began experimenting with utilization management strategies, including prior authorization requirements and the exclusion of certain medications from formularies to mitigate costs.
- 2026: The current landscape is one of skepticism. Despite promises that these drugs would improve overall health and lower long-term costs, employers report a disconnect between the high cost of the drugs and the measurable clinical outcomes in their workforce populations.
Supporting Data: The Scope of the Challenge
The data provided by the Business Group on Health, supplemented by broader research from the Kaiser Family Foundation (KFF), highlights the scale of the challenge. Approximately 1 in 8 American adults currently report taking a GLP-1 medication. This is no longer a niche treatment; it is a mainstream medical intervention.
However, the survey highlights a significant gap in expectations versus reality:
- Coverage Rates: Currently, 67% of surveyed employers provide coverage for GLP-1s specifically for weight management.
- Management Strategies: To curb costs, employers are implementing rigorous controls. A majority now rely on standard cost-sharing arrangements, while many have instituted requirements such as mandatory participation in holistic weight management programs and limiting prescriptions to specific providers.
- Executive Oversight: The financial weight of these decisions is so great that 8 in 10 employers report that executive management teams are now directly involved in the approval and policy decisions surrounding GLP-1 coverage—a level of oversight rarely seen for other pharmaceutical categories.
Official Responses: The Employer Perspective
The sentiment among corporate leadership is one of cautious, and increasingly defensive, concern. Ellen Kelsay, president and CEO of the Business Group on Health, articulated the gravity of the situation in a recent statement.
"Our findings show the tremendous concern employers have regarding these medications from a cost and financial viability perspective," Kelsay stated. "Against the backdrop of anticipated double-digit healthcare cost increases, fueled to a large degree by GLP-1s and overall prescription drug costs, companies cannot ignore the reality that these medications have significant implications for health care budgets—and overall employer affordability."
The consensus among the leadership surveyed is that the "wait and see" approach is failing. Employers are no longer willing to bank on the promise of future cost savings—such as reduced rates of obesity-related comorbidities like heart disease or joint replacements—when the current pharmacy spend is eroding their balance sheets in the present.

Implications for the Future of Benefits
The implications of this trend extend far beyond the pharmacy counter. As employers reach a breaking point, several potential shifts in the benefits landscape are emerging:
1. The End of Universal Coverage
We are likely to see a bifurcation in the workforce. Large, cash-rich corporations may continue to offer GLP-1 coverage as a competitive recruiting tool. Conversely, mid-sized and smaller firms may move to drop weight-loss coverage entirely, citing the necessity of keeping basic health insurance affordable for all staff.
2. The Rise of "Value-Based" Pharmacy Benefits
Employers are demanding more accountability from pharmaceutical manufacturers. If these drugs are to be covered, companies are increasingly looking for outcomes-based contracts where the manufacturer provides rebates or price adjustments if the drug does not lead to measurable clinical improvements or a reduction in secondary medical claims for the patient.
3. A Focus on Holistic Health
The data suggests that simply providing the drug is not enough. Employers are shifting their focus toward "weight management programs" that combine medication with nutrition coaching, physical therapy, and mental health support. The goal is to ensure that if the company is paying for a $1,000-a-month drug, it is being used as a catalyst for a sustainable lifestyle change rather than as a standalone solution.
4. The Data Gap
Perhaps the most concerning finding for the long term is that, despite the massive expenditure, employers have yet to see a "return on investment." Most companies reported that they have seen little to no evidence of lower obesity rates or fewer bariatric surgeries among their covered population. While clinical experts argue that these benefits take years to manifest, employers—who operate on annual budget cycles—are finding it difficult to justify the expense based on long-term, theoretical savings.

Conclusion: A Sustainability Crisis
The story of the GLP-1 in the American workplace is emblematic of a broader issue in the U.S. healthcare system: the clash between medical innovation and economic capacity. While these drugs represent a monumental leap forward in the treatment of obesity—a condition affecting a significant swath of the American public—the current pricing models are proving unsustainable for the employer-sponsored system.
As we move through 2026, the question is no longer whether these drugs are effective, but whether the current model of employer-sponsored health insurance can afford to support them. For millions of employees, the next open enrollment period may bring significant changes to their benefits, as companies move from a period of wide access to one of strict, cost-driven regulation. The path forward will require a complex negotiation between pharmaceutical pricing, clinical outcome transparency, and the financial reality of the modern American corporation.