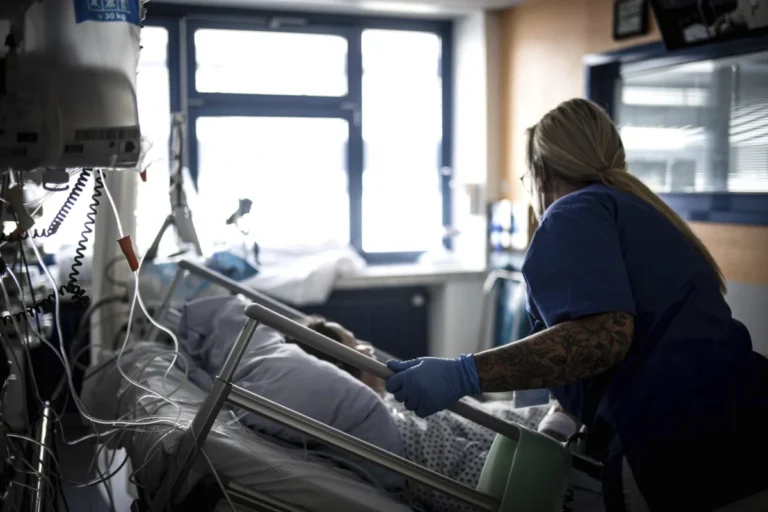
Critical care transport (CCT) represents the absolute pinnacle of Emergency Medical Services (EMS). It is a high-stakes, high-intensity environment where the margin for error is razor-thin. When dealing with the most fragile patients—premature neonates, multi-system trauma victims, or patients fully dependent on complex life-support systems—the transport environment itself becomes a mobile intensive care unit.
However, beneath the veneer of high-acuity medicine lies a persistent, often overlooked crisis: the administrative burden of clinical documentation. For the professionals who navigate these life-or-death scenarios, the paperwork required to validate their care has become a secondary, exhausting marathon. As the industry evolves, the need for intelligent, streamlined, and automated documentation has transitioned from a convenience to a clinical and financial imperative.
Main Facts: The Anatomy of Critical Care Documentation
Critical care transport is inherently different from standard 911 emergency responses. While typical EMS calls focus on stabilization and rapid transit, CCT involves maintaining intensive care standards over long distances, often through the air or across state lines.
The primary challenge in CCT documentation is the sheer density of data. A standard EMS run sheet might track a few sets of vital signs and a narrative of the intervention. A CCT chart, by contrast, must account for:
- Minute-by-minute ventilator settings: Including pressure support, oxygen concentration, and tidal volumes.
- Multi-infusion therapy: Tracking precise dosage rates for vasopressors, sedatives, and paralytics.
- Advanced device management: Monitoring invasive lines, chest tubes, and balloon pumps.
- Lab result integration: Documenting blood gas analyses and biochemical shifts during transport.
Because these cases are often "stacked"—meaning teams move from one high-acuity transport to the next with minimal turnaround—the cognitive load of remembering every detail hours later is immense. This documentation is not merely bureaucratic; it is the legal and medical record of a patient’s survival journey.
Chronology: The Evolution of the "Paper Trail"
The history of CCT documentation reflects the broader digital transformation of healthcare, albeit at a slower pace due to the unique constraints of the field.
- The Era of Paper (Pre-2000s): Documentation was almost exclusively handwritten on carbon-copy forms. In the back of a moving ambulance or a vibrating helicopter, accuracy was often sacrificed to speed and readability.
- The Early Digital Transition (2000–2010): Agencies moved to electronic patient care reporting (ePCR) systems. However, these were often desktop-based, requiring crews to return to the station and spend hours transcribing handwritten notes into a computer.
- The Mobile Integration Era (2010–2020): Ruggedized tablets and laptops allowed for "point-of-care" documentation. Yet, these systems remained largely manual, requiring providers to type data while simultaneously managing patient care.
- The Current Frontier (2020–Present): The focus has shifted toward interoperability and automation. Modern systems are now designed to "talk" to medical devices, pulling data directly into the patient chart, effectively removing the human error associated with manual entry.
Supporting Data: The Cost of Inefficiency
The implications of poor or inefficient documentation extend far beyond the provider’s fatigue. They reach into the financial stability of agencies and the continuity of patient safety.
The Financial Toll
EMS agencies operate on thin margins. A significant portion of revenue is tied to the ability to provide "medical necessity" documentation. If a report is incomplete, messy, or fails to capture the complexity of the intervention, insurance providers—including Medicare and private payers—frequently deny claims. Industry estimates suggest that agencies lose millions annually in recoverable costs due to "documentation leakage," where the intensity of the care provided is not accurately reflected in the final billing code.
The Patient Safety Risk
Discontinuity of care is a known clinical hazard. When a transport team arrives at a receiving hospital, their documentation acts as the "handoff" bridge. If vital details—such as a last-minute adjustment to a ventilator or an undocumented medication bolus—are missing, the receiving ICU team is forced to play catch-up. This "information gap" can lead to medication errors, delays in treatment, and compromised patient outcomes.

Official Perspectives: The Push for Innovation
Industry leaders, such as Joe Graw, Chief Growth Officer at ImageTrend, emphasize that the goal is to shift the focus from data entry to data utilization.
"Critical care work is hard enough without clunky systems making documentation more complicated than it needs to be," Graw notes. The industry consensus is moving toward three core pillars of improvement:
- Device Integration: Using Bluetooth or hardwired connections to stream data from ventilators and cardiac monitors directly into the ePCR. This eliminates the "double-entry" problem.
- Clinical Decision Support: Incorporating "hard stops" and real-time alerts. For example, if a provider attempts to enter a dose of a high-risk medication that falls outside of established protocols, the software alerts them before the record is finalized.
- Structured Data Fields: Replacing free-text boxes with structured, standardized fields. This not only speeds up the charting process but also creates a "clean" dataset that agencies can use to track trends, identify training gaps, and prove clinical efficacy to hospital partners.
Implications for the Future of EMS
The future of critical care documentation is clearly moving toward "invisible" charting. As artificial intelligence and machine learning become more prevalent, the expectation is that the software will eventually be able to "listen" to the environment or synthesize data inputs to create a draft report that the provider simply reviews and validates.
Operational Resilience
For agencies, the implementation of smarter documentation tools is a retention strategy. In an industry facing staffing shortages, reducing the administrative burden on clinicians is a direct way to prevent burnout. When a flight nurse or paramedic can finish their shift without spending an extra hour on redundant paperwork, they are more likely to stay in the field.
Regulatory and Legal Protection
As the landscape of healthcare litigation evolves, the standard of proof for "what happened in the back of the truck" becomes more rigorous. Digital, timestamped, and device-synced logs provide an ironclad audit trail that protects both the agency and the individual provider. It is the best defense against liability and the clearest evidence of professional accountability.
Conclusion: Supporting Those Who Serve
Critical care teams are asked to perform the most demanding tasks in healthcare under the most challenging conditions. They are the frontline of survival, often operating in the dark, in the air, or on the side of a highway. To ask them to also be expert data-entry clerks is to ignore the physical and mental realities of their profession.
By investing in intuitive, device-integrated, and automated documentation systems, agencies do more than just improve their bottom line. They honor the complexity of the work being performed. They ensure that when the transport is over, the provider can focus on their own recovery rather than a mountain of paperwork. As the EMS industry continues to innovate, the most successful agencies will be those that realize that the best way to care for patients is to, first, take better care of the people who transport them.
This article is part of the MedCity Influencers program. Insights provided by Joe Graw, Chief Growth Officer at ImageTrend.