BARCELONA, Spain — For decades, the cornerstone of managing acute decompensated heart failure (HF) has been the administration of loop diuretics to achieve decongestion. Yet, for a significant subset of patients, the standard pharmaceutical approach often falls short. New data presented at the European Society of Cardiology’s Heart Failure 2026 congress suggest that clinicians may be missing a vital diagnostic window: the early identification of "diuretic resistance."
A post-hoc analysis of the landmark TRANSFORM-HF trial reveals that patients identified as high-risk for diuretic resistance face substantially worse clinical outcomes, regardless of whether they are prescribed furosemide or torsemide. The findings underscore a shift in clinical philosophy: when loop diuretics fail, simply swapping one for another is insufficient. Instead, physicians must pivot toward aggressive, alternative decongestion strategies.
The Clinical Challenge: Defining Diuretic Resistance
Diuretic resistance is characterized by the body’s inability to achieve adequate natriuresis—the excretion of sodium via urine—despite the administration of appropriate or escalated doses of loop diuretics. While the phenomenon is well-recognized in academic circles, it remains notoriously difficult to quantify in the "heat of battle" within a busy emergency department or inpatient cardiac ward.
"In clinical practice, there is heterogeneity in response to loop diuretics," explained Ambarish Pandey, MD, of the University of Texas Southwestern Medical Center. "Diuretic resistance affects a substantial subset of patients and is associated with worse decongestion and, ultimately, worse outcomes for the patient."
For years, the medical community lacked a standardized, accessible tool to predict which patients would fall into this refractory category. This led to a "trial and error" approach, where clinicians would wait to see if a patient responded to initial treatment before deciding to escalate or modify therapy. This delay often results in prolonged hospital stays, persistent symptoms, and higher mortality rates.
Chronology of Evidence: From TRANSFORM-HF to BAN-ADHF
The foundation for this analysis lies in the TRANSFORM-HF trial, a massive, pragmatic study originally designed to determine if torsemide offered a clinical advantage over the more commonly used furosemide in hospitalized heart failure patients. When the primary results were unveiled at the 2022 American Heart Association scientific sessions, they sent a ripple through the cardiology community: there was no meaningful difference in all-cause mortality or readmission rates between the two drugs.
However, the trial left a lingering question: Did the "average treatment effect" mask a specific sub-population that was fundamentally resistant to both drugs?
To investigate this, Dr. Pandey and his colleagues applied the BAN-ADHF (Bumetanide-Associated Natriuresis in Acute Decompensated Heart Failure) risk score—a tool they first validated in a 2023 study—to the TRANSFORM-HF patient cohort.
The BAN-ADHF score was developed to provide a "point-of-care" risk assessment. By aggregating eight variables—including renal function, natriuretic peptide levels, serum bicarbonate, prior exposure to diuretics, and comorbidities such as atrial fibrillation and hypertension—the score generates a value. A score greater than 12 identifies patients at high risk for diuretic resistance.
By applying this score to 2,421 participants from the TRANSFORM-HF trial, researchers were finally able to look "under the hood" of the data, categorizing patients by their inherent risk profiles rather than just their assigned medication.
Supporting Data: The High-Risk Phenotype
The analysis of the 2,421 participants provided a sobering picture of the high-risk patient. Approximately 21% of the cohort met the threshold for high diuretic resistance risk. These patients were, on average, older, possessed higher levels of NT-proBNP, and suffered from significantly impaired renal function.
The data revealed a stark divergence in prognosis:
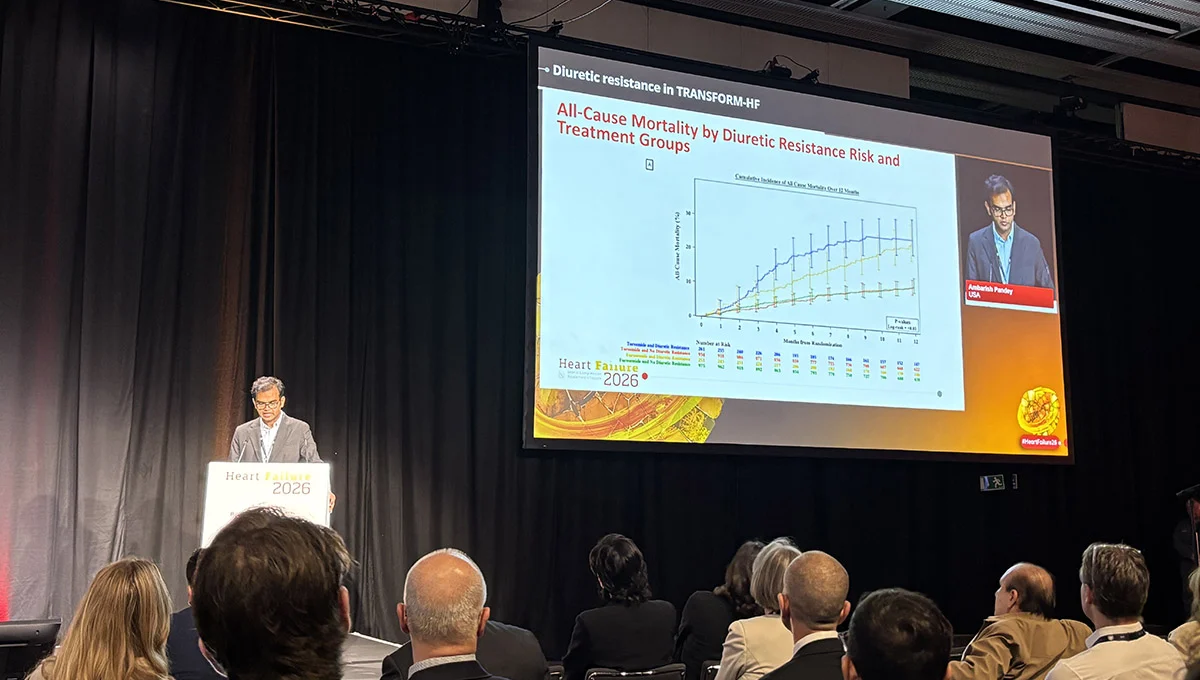
- Mortality: Patients with a high BAN-ADHF score faced a hazard ratio (HR) of 1.79 (95% CI 1.45-2.21) for all-cause mortality.
- Hospitalization: The risk for all-cause hospitalization was significantly higher (HR 1.34; 95% CI 1.15-1.55), with high-risk patients experiencing a greater cumulative burden of recurrent admissions.
- Quality of Life: Using the Kansas City Cardiomyopathy Questionnaire (KCCQ) Clinical Summary Score, researchers found that high-risk patients experienced significantly less improvement in their quality of life compared to low-risk peers.
Crucially, when the researchers stratified these patients by their assigned medication (furosemide vs. torsemide), the "high-risk" curves for mortality and hospitalization remained uniformly poor, regardless of the drug administered. The treatment arms showed no meaningful separation, confirming that for these patients, the choice between the two common loop diuretics was effectively moot.
Official Responses and Clinical Perspectives
The presentation of these findings at the ESC Heart Failure 2026 congress sparked an intense dialogue among leading cardiovascular experts. Piotr Ponikowski, MD, of Wroclaw Medical University, praised the BAN-ADHF score as a "great prognosticator" but raised the critical clinical question: If we can identify these patients, how do we change their trajectory?
Dr. Pandey’s response highlighted a critical distinction between prognostic scoring and therapeutic intervention. "The lack of interaction in this study is less of a reflection on the score and more of a reflection on the treatment in TRANSFORM-HF," Pandey noted.
He emphasized that while swapping furosemide for torsemide failed to yield results, other trials—such as ADVOR (using acetazolamide), CLOROTIC, and PUSH-AHF—have suggested that "intensification" or "diversification" is the key. In essence, if the primary pathway (loop diuretics) is blocked, adding a secondary, different mechanism of action—such as distal tubule diuretics—is far more effective than merely increasing the dose of the failing medication.
Implications for Modern Cardiology
The shift in paradigm suggested by these findings is three-fold:
1. Routine Risk Stratification
The BAN-ADHF score is now available for real-world clinical use. The implication is that every patient admitted with acute heart failure should be assessed for diuretic resistance within the first 24 hours. By identifying the 20-25% of patients at high risk, clinicians can move from a "wait and see" strategy to a proactive management plan.
2. Moving Beyond "Loop" Reliance
The data confirms that the loop diuretic-centric approach has reached its ceiling for a large segment of the population. When the BAN-ADHF score flags a patient as high-risk, the clinical team should be prepared to introduce combination diuretic therapy early. This might include acetazolamide or thiazide-like diuretics to target different segments of the nephron, ensuring effective fluid removal.
3. Precision Medicine in HF
This study serves as a masterclass in how post-hoc analysis of large-scale trials can extract precision medicine insights. While the original TRANSFORM-HF trial was viewed by some as a "negative" trial because it found no difference between two common drugs, the secondary analysis proves the data was a goldmine for understanding patient phenotypes. It underscores the necessity of moving away from "one-size-fits-all" treatment protocols in heart failure.
Conclusion
The findings presented in Barcelona mark a transition toward a more nuanced era of heart failure management. By acknowledging that diuretic resistance is a distinct, measurable phenotype, clinicians can finally break the cycle of ineffective therapy.
As Dr. Pandey concluded, "There is value in leveraging a clinical score to identify diuretic resistance early. But rather than swapping one loop diuretic for another, it makes more sense to switch to an entirely different type of diuretic." The path forward for the field is clear: identify the resistant patient early, and hit the target with multi-modal therapy before the patient’s condition—and quality of life—deteriorate beyond the reach of simple loop-diuretic intervention.