For many older adults, the transition from evening to morning is not a period of restorative calm, but rather an increasingly difficult emotional hurdle. As the global population ages, clinical focus has often centered on the prevention of cognitive decline, dementia, and physical frailty. However, a silent, pervasive challenge frequently goes undertreated: late-life anxiety.
A groundbreaking study conducted by researchers at the Center for BrainHealth at The University of Texas at Dallas has now illuminated a crucial biological mechanism behind this emotional burden. Published in Nature Communications Psychology, the research reveals that the decline of "slow-wave sleep"—the deep, restorative phase of non-REM sleep—is a primary driver of overnight emotional dysregulation in older adults. More importantly, the study suggests that because sleep is a modifiable behavior, it may offer a promising, actionable target for clinical intervention that structural brain changes do not.
The Science of Slow-Wave Activity
Slow-wave sleep, characterized by large, rhythmic, rolling brain oscillations, is often described as the "deepest" form of sleep. It is during this stage that the brain engages in intensive maintenance, clearing out metabolic waste and consolidating memories.
The UT Dallas team, led by Dr. Eti Ben Simon and senior author Dr. Matthew Walker, sought to understand how the deterioration of this specific sleep architecture impacts emotional health. By analyzing 61 cognitively healthy older adults with a mean age of 74.6, the researchers discovered that the ability to generate these "slow waves" is a critical barometer for how an individual feels the following morning.
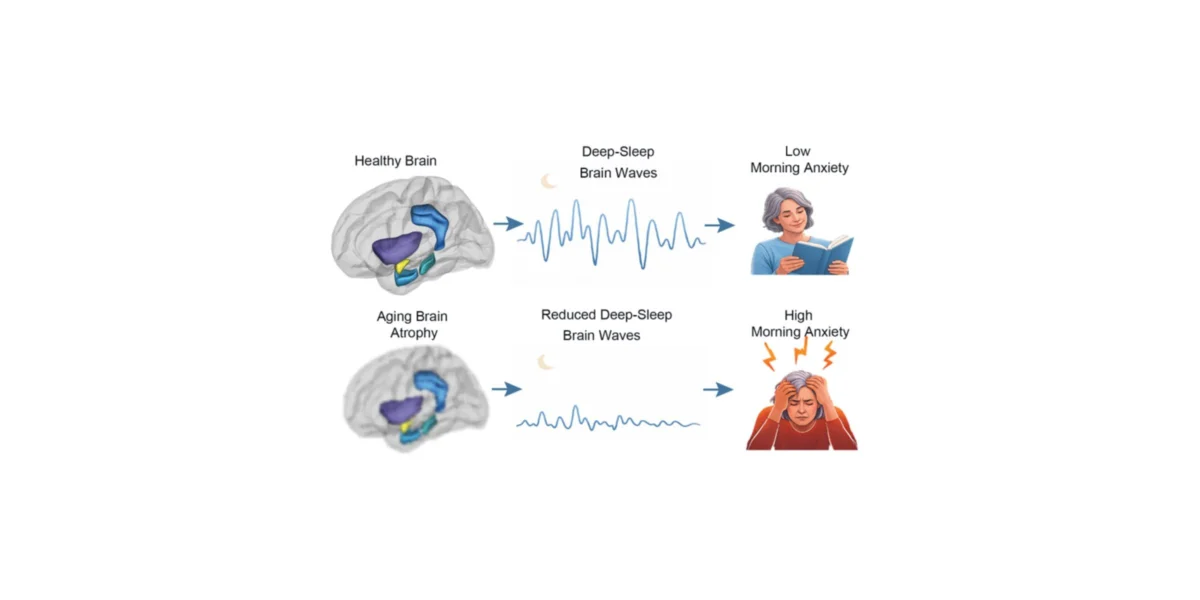
Those participants who maintained robust slow-wave activity during the night woke up with significantly lower anxiety levels. Conversely, those who produced fewer slow waves exhibited a measurable spike in morning anxiety. Crucially, this relationship remained consistent regardless of the participant’s chronological age, suggesting that the quality of sleep, rather than the number of years lived, is the primary mediator of emotional well-being.
Chronology: A Four-Year Longitudinal Perspective
To understand whether this relationship was a snapshot in time or a progressive decline, the researchers conducted a longitudinal follow-up. A subset of 24 participants returned to the laboratory four years after their initial assessment to repeat the comprehensive battery of tests.
The findings were stark. Over the four-year span, the group experienced an average 20% decline in slow-wave activity. This reduction in deep sleep was accompanied by a corresponding increase in self-reported anxiety levels. This longitudinal data provided the "smoking gun" for the researchers: as the brain’s capacity to generate deep sleep erodes, the individual’s psychological resilience against anxiety diminishes in tandem.
While the study confirmed that structural brain atrophy—specifically in the amygdala, insula, and cingulate cortex—correlates with fewer slow waves, the researchers were careful to note that the atrophy itself is not the immediate cause of the anxiety. Instead, the structural decay acts as a bottleneck, impairing the brain’s ability to generate the deep sleep necessary for emotional recalibration.
Supporting Data and Physiological Mechanisms
The study utilized high-resolution MRI scans and polysomnography to create a multidimensional view of the aging brain. The data suggests two primary pathways through which slow-wave sleep serves as an emotional buffer:
- Autonomic Nervous System Regulation: Deep sleep acts as a bridge between the sympathetic nervous system (the "fight or flight" response) and the parasympathetic system (the "rest and digest" response). By facilitating a shift toward parasympathetic recovery, deep sleep reduces the brain’s reactivity to stressors the following day.
- The Locus Coeruleus Connection: The researchers hypothesize that the decline in slow-wave sleep is tied to the degradation of the locus coeruleus, a brainstem structure responsible for producing noradrenaline. As this region begins to degenerate, the biological machinery required to trigger deep sleep begins to fail, leaving the brain in a heightened state of alertness.
Interestingly, the study found that REM sleep did not share this predictive relationship with next-day anxiety, narrowing the focus of potential therapeutic interventions to the slow-wave phase specifically.
Official Responses: Shifting the Paradigm
The implications of these findings are significant for geriatric medicine, where anxiety is often dismissed as an inevitable side effect of aging or overshadowed by concerns over neurodegeneration.
"Deep sleep acts as a kind of nightly recalibration for the anxious brain," says Dr. Eti Ben Simon, associate director of the Sleep Innovation Laboratories at the Center for BrainHealth. "When that recalibration is impaired, anxiety doesn’t fully resolve overnight. The encouraging part is that sleep is modifiable in ways that brain structure is not, offering a powerful lever to help the aging brain continue to adapt and thrive."
Dr. Matthew Walker, director of the sleep innovation laboratories and a leading voice in neuroscience, emphasizes the urgency of this discovery. "The stakes here are real," Dr. Walker stated. "As a society, our brainspans are not keeping up with our extended lifespans, but research continues to reveal new avenues that we can influence to proactively improve and optimize our brain health—including sleep."
Dr. Walker further clarified the distinction between structural loss and functional impairment: "The atrophy is upstream—it’s the power cut, not the darkness itself." This analogy underscores the optimism of the study; while we may not yet have the technology to fully reverse structural atrophy in the brain, we have a growing array of tools to influence the quality of sleep, potentially "turning the lights back on" for emotional health.
Implications for Future Intervention
The most transformative aspect of this research is the transition from observation to intervention. Because the study identifies slow-wave sleep as a "modifiable target," the team at the Center for BrainHealth is already designing future clinical trials.
Potential Therapeutic Avenues:
- Acoustic Stimulation: The researchers are investigating the use of precisely timed audio cues delivered during the non-REM sleep cycle. These "pink noise" or rhythmic sound patterns are designed to synchronize with existing brain oscillations, effectively boosting the amplitude and frequency of slow waves.
- Preventative Neurology: The team is currently examining whether the preservation of slow-wave activity can act as a protective barrier, slowing the progression from healthy aging to mild cognitive impairment (MCI).
- Clinical Screening: Currently, anxiety in older adults is under-diagnosed. This research supports the integration of sleep quality assessments into routine geriatric physicals, allowing clinicians to identify "at-risk" patients before anxiety levels reach a clinical threshold.
Conclusion: A New Frontier in Brain Health
The findings from the UT Dallas team provide a compelling narrative for the future of aging. By framing sleep not merely as a passive necessity but as an active, therapeutic mechanism for emotional regulation, the study challenges the medical community to look beyond the surface of cognitive decline.
If deep sleep can indeed be rehabilitated through acoustic stimulation or other non-invasive techniques, the implications for late-life anxiety are profound. It suggests a future where mental health in our later years is not a matter of inevitable decline, but one of maintenance and optimization. As the research moves into the next phase of clinical trials, it offers a beacon of hope: even as our brains change with age, the "nightly recalibration" that keeps us grounded remains a lever within our reach.