For the first time since 2018, the American College of Cardiology (ACC) and the American Heart Association (AHA) have issued a sweeping update to clinical guidance on the screening and management of blood cholesterol. Unveiled on March 28 at the ACC’s 75th Annual Scientific Session in New Orleans, these recommendations—published simultaneously in the Journal of the American College of Cardiology and Circulation—mark a fundamental shift in how the medical community approaches cardiovascular disease (CVD) prevention.
The guidelines arrive at a critical juncture in public health. As modern medicine continues to grapple with the long-term impacts of metabolic health, the new framework shifts the focus from reactive treatment to proactive, personalized, and lifelong risk management.
The Core Mandate: Lowering LDL and Prioritizing Prevention
At the heart of the 2026 guidance is an intensified commitment to lowering low-density lipoprotein (LDL) cholesterol—the "bad" cholesterol that serves as the primary engine for atherosclerosis. The guidelines also place a new emphasis on other lipid markers, such as lipoprotein(a) [Lp(a)], and underscore the necessity of early intervention.
"We know that lower LDL cholesterol levels are better when it comes to reducing the risk of heart attacks, strokes, and congestive heart failure," explains Roger S. Blumenthal, M.D., chair of the guideline writing committee and director of the Johns Hopkins Ciccarone Center for the Prevention of Cardiovascular Disease. "We also know that bringing elevated lipids and blood pressure down in young adults supports optimal heart and vascular health throughout a person’s life."
The message is clear: cardiovascular health is not a destination reached in middle age, but a cumulative process that begins in early adulthood. By addressing lipid dysregulation in the young, clinicians can prevent the "silent" buildup of plaque that leads to catastrophic events later in life.
Chronology of Change: From 2018 to 2026
To understand the magnitude of these updates, one must look at the evolution of cardiac care over the last decade.
- 2018 Guidance: The previous cholesterol guidelines focused heavily on the use of statins and established 10-year risk assessment models for adults aged 40 and older. While revolutionary at the time, these guidelines primarily targeted established risk factors like age, basic cholesterol panels, and blood pressure.
- The Interim Years (2019–2025): Advancements in genetic testing, imaging technology (such as coronary artery calcium scoring), and the development of non-statin therapies like PCSK9 inhibitors necessitated a review of existing protocols. Furthermore, a growing body of evidence linked pregnancy complications and autoimmune conditions to long-term heart risk.
- 2026 Update: The current guidance integrates these advancements. It expands the scope of the risk assessment tool, incorporates a broader range of patient history, and introduces aggressive lipid-lowering targets for diverse populations.
Supporting Data: Why Earlier Screening is Non-Negotiable
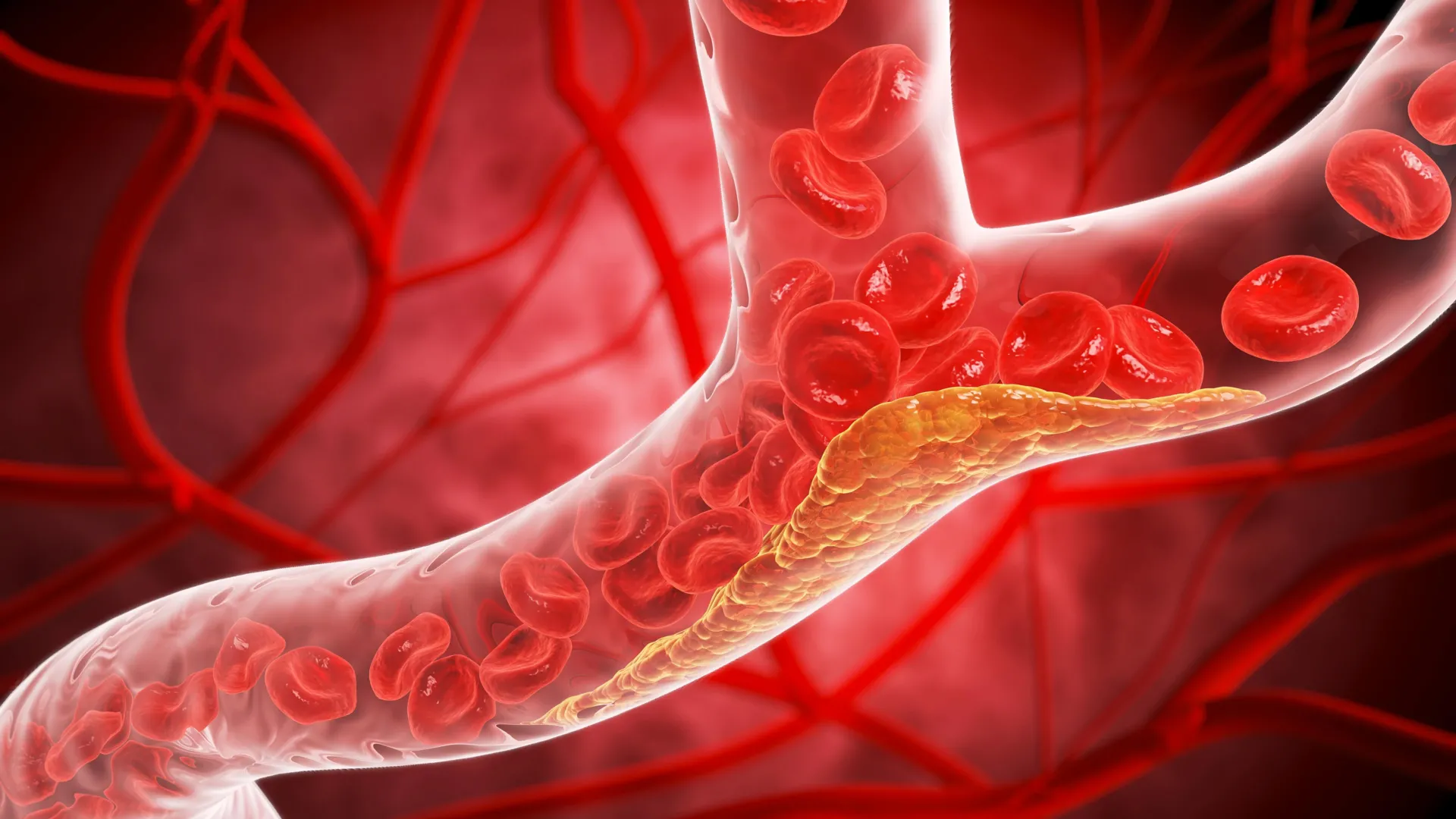
The urgency of this update is backed by sobering statistics: roughly 1 in 4 American adults currently lives with elevated LDL cholesterol. This condition is the primary driver of atherosclerosis, where lipids build up along the inner walls of the arteries. Over time, this plaque restricts blood flow, and if a rupture occurs, it can trigger a heart attack or stroke.
The Role of Genetics and "Risk Enhancers"
The new guidelines advocate for a more nuanced view of the patient. This includes looking beyond traditional markers to identify "risk enhancers."
- Genetic Screening: For individuals with familial hypercholesterolemia—a genetic condition characterized by high LDL levels—screening should now begin as early as age 9.
- Lp(a) Testing: The guidelines recommend a one-time test for Lp(a). This marker, which is largely inherited, can increase heart disease risk by 40% at levels of 125 nmol/L and can double that risk at 250 nmol/L.
- Hidden Risk Factors: The guidelines explicitly advise doctors to consider history beyond the standard "Big Five" (smoking, blood pressure, cholesterol, diabetes, and age). Clinicians are now urged to inquire about early menopause, preeclampsia, gestational diabetes, and chronic inflammatory conditions like rheumatoid arthritis or HIV.
The PREVENT Calculator: A Technological Leap
Perhaps the most significant technical advancement in the 2026 guideline is the introduction of the Predicting Risk of Cardiovascular Disease EVENTs (PREVENT) calculator.
The previous risk model was limited to a 10-year outlook for individuals 40 and older. The PREVENT tool, however, is a massive upgrade. Based on data from 6.6 million individuals—a dramatic leap from the 26,000 used in the previous model—the tool provides both 10-year and 30-year risk projections. It allows clinicians to start assessments at age 30 and incorporates vital indicators such as kidney function and blood sugar levels.
"Shifting the paradigm toward proactive prevention strategies earlier in life can meaningfully change the trajectory of cardiovascular disease and lead to better health outcomes for people decades later," notes Seth Martin, M.D., M.H.S., a member of the guideline writing committee.
Official Responses and Clinical Implications
The cardiovascular community has responded with cautious optimism, noting that while the guidelines are ambitious, they provide the necessary roadmap to curb the rising rates of heart disease.
Aggressive Targets and Diverse Therapies
The guidelines are not one-size-fits-all. Treatment targets are now tiered based on risk profiles:
- Low-to-Moderate Risk: LDL-C should be maintained below 100 mg/dL.
- Intermediate Risk: Targets are lowered to below 70 mg/dL.
- High-Risk Individuals: A target of less than 55 mg/dL is recommended.
To achieve these goals, the medical community is moving beyond a "statins-only" approach. The 2026 guidance explicitly validates the use of ezetimibe, bempedoic acid, and PCSK9 monoclonal antibodies. These therapies are crucial for patients who either cannot tolerate statins or whose LDL levels remain stubbornly high despite standard treatment.
Lifestyle as the Foundation
Despite the emphasis on high-tech diagnostic tools and pharmaceutical innovation, the committee remains firm on the basics. Experts stress that lifestyle modifications remain the first line of defense. A balanced, heart-healthy diet, consistent physical activity, tobacco cessation, adequate sleep, and weight management remain the cornerstones of prevention. According to Dr. Blumenthal, approximately 80% to 90% of cardiovascular disease can be linked to these modifiable lifestyle factors.
Future Directions: Beyond 2026
The release of these guidelines is not the end of the conversation. An accompanying editorial in the American Journal of Preventive Cardiology highlights the potential for even more aggressive targets in the future. Drawing on data from the VESALIUS-CV clinical trial, which demonstrated the benefits of combining multiple therapies to reach very low cholesterol levels, some experts are already suggesting that the threshold for moderate atherosclerosis patients should be pushed even lower than 55 mg/dL.
The collaboration between the ACC, the AHA, and various other sub-specialty organizations signifies a unified front. By integrating cutting-edge data science with a more inclusive understanding of human biology—from pregnancy history to genetic markers—the 2026 guidelines represent a significant milestone in preventive medicine.
For the clinician, the mandate is clear: start earlier, look deeper, and utilize the full spectrum of tools—from lifestyle counseling to advanced lipid-lowering therapies—to safeguard the long-term health of the population. For the patient, the takeaway is equally clear: heart health is a lifelong pursuit, and the window for effective intervention is wider, and more important, than ever before.