By Sree Roy
For years, the sleep medicine community has been locked in a high-stakes dialogue regarding the maintenance of Continuous Positive Airway Pressure (CPAP) equipment. The message from the US Food and Drug Administration (FDA) and major manufacturers has been consistent and clear: the rise of third-party, automated "plug-and-play" cleaning devices—often utilizing ozone or ultraviolet (UV) light—poses unnecessary risks to patient health and equipment integrity.
New survey data from Sleep Review suggests that this public health campaign has been a resounding success. Patients are, by and large, heeding the warnings. However, a troubling secondary trend has emerged: as users move away from these automated gadgets, they are falling short in the manual cleaning processes that are essential for long-term health and device performance.

The Shift Away from Automated Cleaning Devices
The FDA’s stance on automated cleaning devices has been unequivocal. In official guidance, the agency has stated, “These machines are not necessary to clean your CPAP. Most CPAP accessories like masks, hoses, and CPAP machine humidifier tanks can be cleaned with mild soap and water as described in the owner’s manual.” The FDA further clarified that these add-on devices do not, and cannot, replace the rigorous cleaning protocols established by the original manufacturers.
The market response to these warnings has been stark. According to the recent Sleep Review survey, a staggering 86% of respondents reported that they have “never” used an automated CPAP cleaning device. Of the remaining 14%, all confirmed they are former users, with zero respondents indicating that they currently rely on these automated systems for their daily hygiene routines.
This shift is largely driven by a growing awareness of the potential financial and mechanical consequences. With many CPAP manufacturers now explicitly updating their warranty language to exclude damage caused by ozone or UV exposure, the financial risk has become a primary motivator for patients. The survey found that 57% of users are “very concerned” that using such devices would void their equipment warranties. The remaining 43% acknowledged that while they were not aware of the specific warranty implications, the shift away from these devices remains a priority due to the guidance of their healthcare providers.

The Role of Clinical Guidance
The success of this transition is largely attributable to the proactive role of durable medical equipment (DME) providers. The survey highlights a "boots-on-the-ground" approach to education, where staff members at supply companies are actively discouraging the use of automated cleaning systems during the setup and follow-up processes.
One respondent captured the sentiment of many, noting, “I was told by an employee from a CPAP supply company to not use any of the CPAP cleaning machines… that they weren’t good for the machine.” This direct line of communication between clinicians and patients appears to be the most effective mechanism for dispelling the convenience-driven allure of automated cleaners.
The Manual Cleaning Deficit: A Concerning Trend
While the abandonment of ozone and UV cleaners is a positive development for patient safety, it has exposed a significant weakness in home-care compliance. The transition back to traditional soap-and-water methods has not been uniform across the entire CPAP system.

Data reveals that patients are prioritizing the “high-touch” components—specifically the mask—while neglecting the deeper, more complex parts of the system. Over half (57%) of respondents reported washing their CPAP mask within the past 24 hours, adhering to standard industry recommendations. Another 29% report washing it within the past week. However, the numbers drop precipitously when looking at other vital components.
The maintenance of tubing, humidifiers, and internal filters is often inconsistent. Many patients express a lack of clarity regarding how often these parts require a deep clean, leading to a "set it and forget it" mentality that can result in the accumulation of mineral deposits, bacteria, and moisture—the perfect breeding ground for respiratory irritants.
The Complexity of Disassembly
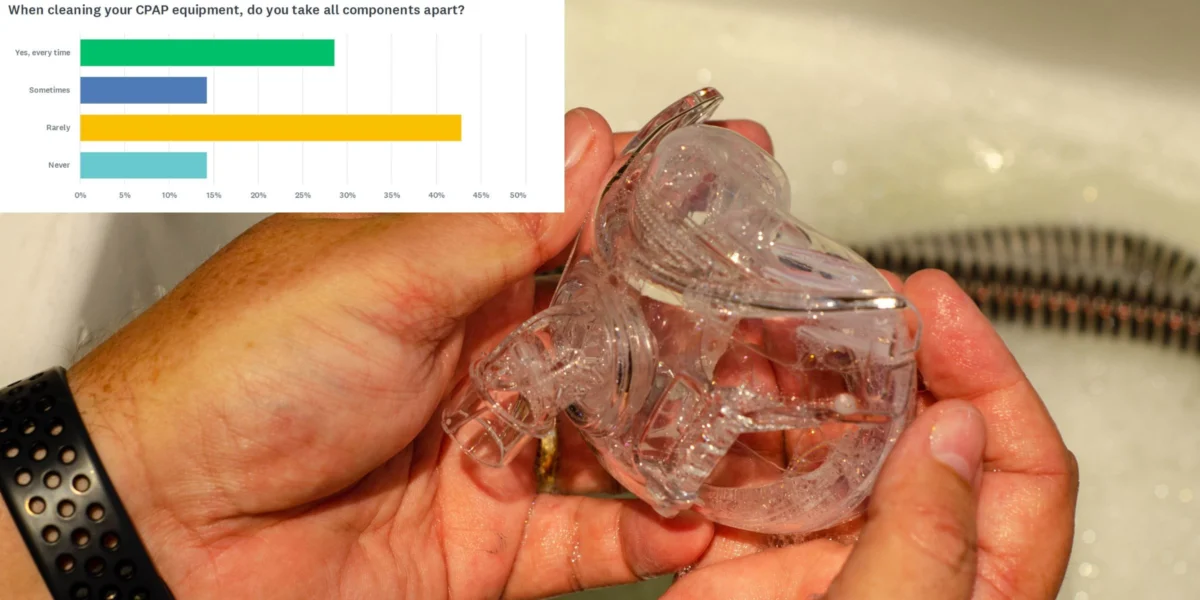
Perhaps the most alarming finding in the survey is the reluctance of patients to fully dismantle their CPAP systems for cleaning. Effective maintenance requires a complete teardown of the equipment, yet only 29% of respondents report taking all components apart “every time” they clean their equipment.

The frequency of full disassembly is strikingly low:
- Always: 29%
- Sometimes: 14%
- Rarely: 43%
- Never: 14%
This failure to disassemble the equipment prevents a truly thorough cleaning. When components like the humidifier water chamber, the internal seals of the mask, and the connection points between the tubing and the unit remain attached, residual moisture and biofilm can persist. This not only degrades the plastic and silicone materials over time but can also lead to the delivery of contaminated air, potentially exacerbating the very respiratory conditions the CPAP is intended to treat.
Cleaning Methods and Drying Protocols
When patients do engage in cleaning, the methodologies are diverse, if not always ideal. Roughly 29% of respondents utilize specialized CPAP wipes, while another 29% use CPAP-specific soaps. Others rely on household staples such as white vinegar and distilled water.

Drying protocols also present a potential point of failure. While 83% of users correctly utilize air drying on a towel or rack—with most reporting a drying time of under two hours—there is a cohort that remains uncertain about the risks of improper drying. Moisture trapped in hoses or filters is a significant concern for sleep specialists, as it can encourage mold growth. The emergence of automated CPAP dryers—distinct from the controversial cleaning devices—has captured about 17% of the user base, representing a middle ground for patients seeking both convenience and safety.
Official Responses and Regulatory Perspective
The FDA’s position serves as the bedrock for the current industry standard. By emphasizing that "add-on" devices are not a substitute for manual hygiene, the FDA has forced a re-evaluation of how companies market their products. The agency’s Consumer Update regarding CPAP cleaning devices continues to be the definitive resource for providers and patients alike.
Manufacturers have followed suit by standardizing their user manuals to include explicit warnings. These documents now detail specific, non-toxic cleaning agents that are safe for the materials used in modern CPAP components. The industry-wide pushback against automated cleaners is, therefore, not merely a protective measure for warranties, but a fundamental stance on medical device safety.

Implications for Sleep Medicine
The implications of these findings are profound for sleep medicine professionals. The data suggests that while the "war" against automated cleaning devices has been won, the "battle" for daily, proper maintenance is ongoing.
For DME providers and sleep physicians, the challenge is no longer just about discouraging harmful practices; it is about providing comprehensive, actionable education on the "how-to" of manual cleaning. Many patients report feeling overwhelmed by the complexity of disassembling their devices, often opting to clean only the mask because it is the most visible and accessible part of the system.
Future patient education programs must pivot toward:

- Visual Training: Providing step-by-step video tutorials or physical demonstrations of how to safely disassemble a CPAP unit.
- Scheduling Support: Helping patients integrate cleaning into their daily routines, similar to how they integrate the use of the CPAP itself.
- Material Awareness: Educating patients on why specific soaps (like those without harsh chemicals or fragrances) are essential to prevent the degradation of sensitive silicone seals.
- The "Hidden" Components: Placing a greater emphasis on the cleaning of water chambers and filters, which are often the most neglected parts of the device.
Conclusion: A Renewed Commitment to Hygiene
The transition away from automated cleaning devices marks a significant turning point in CPAP compliance. It demonstrates that patients are responsive to scientific guidance and are increasingly protective of their equipment. However, the survey data serves as a clear warning: convenience cannot come at the expense of hygiene.
As we move forward, the focus must remain on the diligence of the user. A clean CPAP machine is not just a requirement for a valid warranty; it is a critical component of effective sleep apnea therapy. By closing the gap between the knowledge of why to clean and the skill of how to clean properly, the medical community can ensure that patients are getting the full, life-saving benefits of their CPAP therapy without the risks associated with inadequate maintenance.
The data is clear—patients are listening. Now, the industry must ensure they have the tools and the confidence to keep their equipment as clean as their health demands.