For individuals living with Ehlers-Danlos Syndrome (EDS), the body’s internal architecture is often a source of persistent challenge. EDS, a group of genetic connective tissue disorders, is characterized by joint hypermobility, skin hyperextensibility, and tissue fragility. Because collagen—the body’s "glue"—is defective, the skeletal system often struggles to maintain structural integrity. One of the most significant manifestations of this instability is scoliosis, an atypical, progressive curvature of the spine.
While scoliosis is often viewed through the lens of adolescent development, for the EDS community, it represents a lifelong management concern. To shed light on this complex interplay, we examine the nuances of spinal health in hypermobile populations and spotlight the Schroth Method, a specialized, evidence-based approach to physical therapy that is transforming outcomes for patients.
The Essentials: Understanding Scoliosis
Scoliosis is defined as an atypical lateral curvature of the spine. While commonly diagnosed during the rapid growth spurts of adolescence, it is not merely a pediatric condition. It is a progressive disorder, meaning the "Cobb angle"—the standard clinical measurement used to assess the severity of the spinal curvature—can increase over a patient’s lifetime.
For the general population, scoliosis is a common orthopaedic finding. However, when paired with the connective tissue laxity inherent in EDS, the spine’s ability to resist gravity and maintain neutral alignment is significantly compromised.
The EDS-Scoliosis Connection: A Clinical Overview
The relationship between EDS and spinal deformity is statistically significant. Research indicates that approximately 29% of individuals with EDS present with some degree of scoliosis.
Data Breakdown:
- Mild Scoliosis (10–24° Cobb angle): Affects 87.5% of the EDS-scoliosis population.
- Moderate Scoliosis (25–40° Cobb angle): Affects 12.5% of the population.
- Severe Cases: While rarer in the general EDS population, the kyphoscoliotic subtype of EDS (kEDS) is specifically linked to more profound spinal deformities.
In hypermobile bodies, the ligaments and tendons that typically "lock" joints into place are unable to provide the necessary tension to stabilize the vertebrae. This leads to a vicious cycle: as the spine shifts, the muscles must work harder to compensate, often leading to chronic pain, spasms, and localized fatigue.
The Schroth Method: A Specialized Intervention
For many years, the standard of care for mild-to-moderate scoliosis was "wait and see," often followed by generic physical therapy or bracing. However, for those with EDS, generic strengthening exercises—like standard planks or dead bugs—may fail to address the three-dimensional nature of a scoliotic curve.
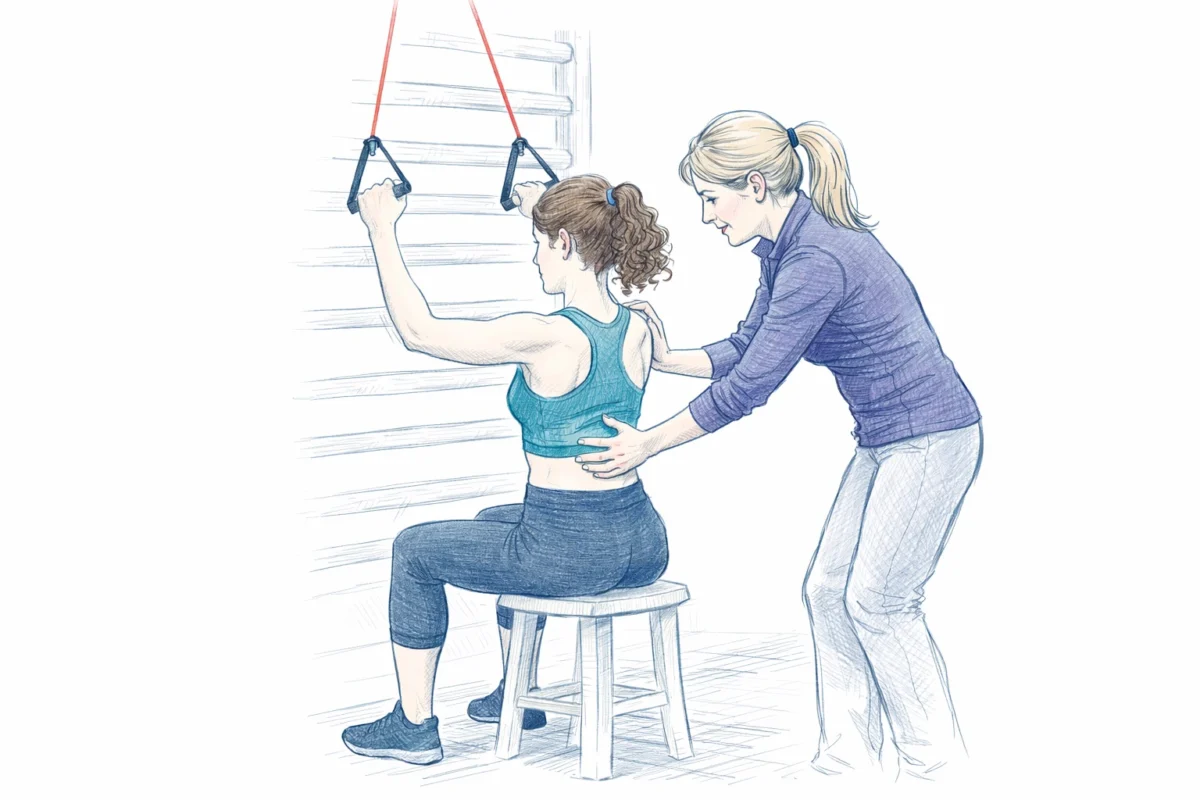
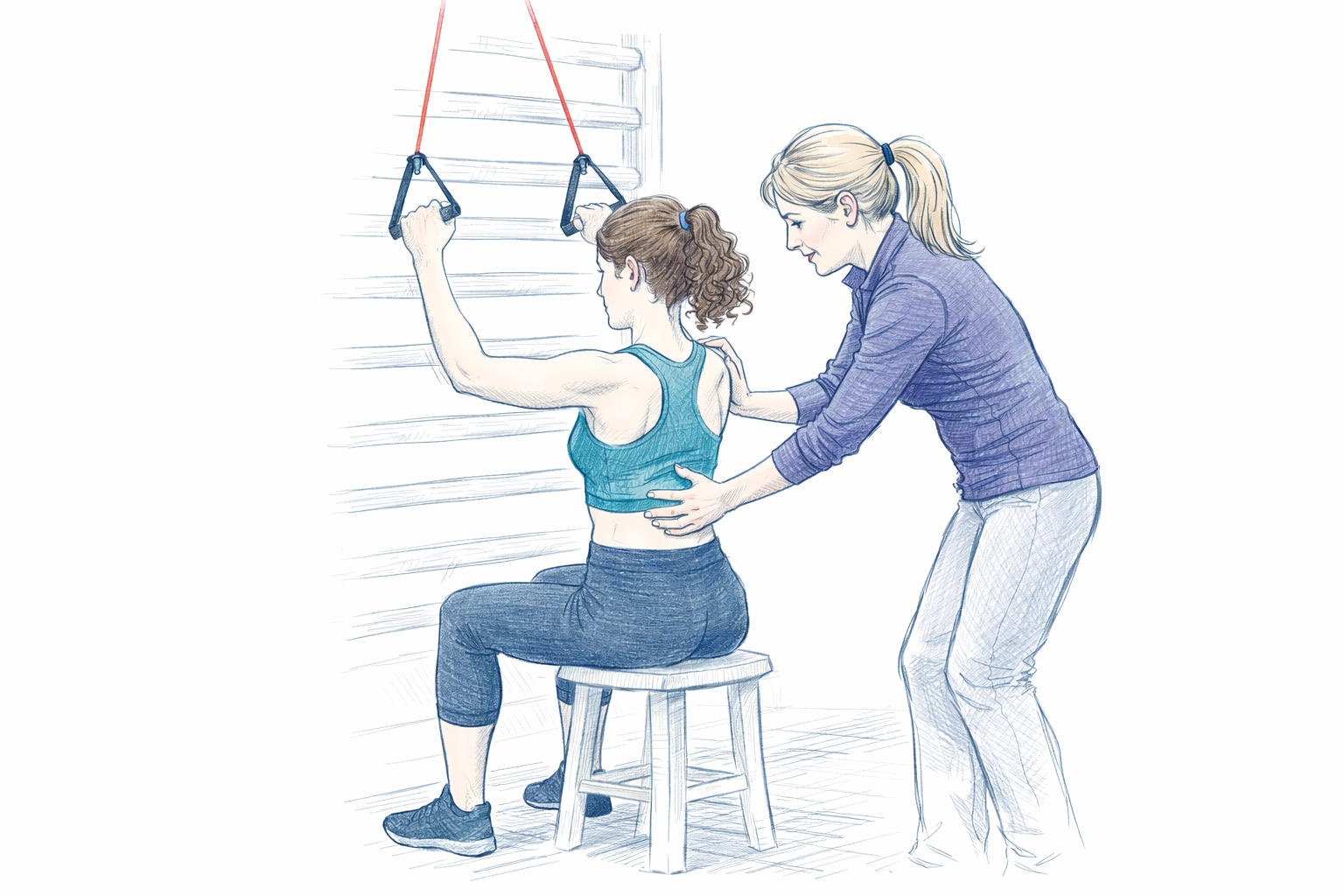
Enter the Schroth Method. Unlike traditional physical therapy, which often focuses on general core strength, the Schroth Method is a highly calibrated, evidence-based approach designed to de-rotate and elongate the spine. It focuses on:
- Correcting Muscle Asymmetry: Identifying which muscles are overactive and which are under-active due to the spinal tilt.
- Postural Awareness: Training the patient to breathe into the "collapsed" areas of the ribcage to expand the torso.
- Active Engagement: Utilizing active muscle engagement rather than passive stretching, which is critical for the safety of hypermobile patients.
Expert Q&A: Perspectives from the Clinic
To better understand how this method translates to real-world outcomes for EDS patients, we sat down with Caroline Campesi, DPT, a leading Schroth-certified physical therapist.
Q: What drew you to specialize in scoliosis, specifically regarding hypermobility?
Campesi: "I started my career in general orthopedics, but I kept seeing patients with persistent neck and back pain whose torsos just looked ‘off.’ In PT school, we spent less than an hour on scoliosis. I realized I lacked the diagnostic tools to assess spinal asymmetry. Once I started my first Schroth training in 2019, I was hooked. The level of detail in the assessment is unparalleled, and we see clinical gains in patients within just a few visits."
Q: How common is hypermobility in your scoliosis caseload?
Campesi: "It is incredibly high. I’m often surprised when a new patient doesn’t have hypermobility. Last week, I treated 22 patients; 13 scored higher than 5/9 on the Beighton scale (a standard assessment for hypermobility). I estimate that roughly 75% of my total caseload presents with some form of connective tissue disorder."
Q: Is scoliosis in EDS patients purely a structural issue?
Campesi: "Absolutely not. EDS is systemic. Patients often come to me thinking their pain is solely from their spine, but we have to look at the ‘whole-body’ picture. Because connective tissue is in our arteries and intestines, these patients often deal with GI issues, cardiovascular symptoms, or dysautonomia like POTS (Postural Orthostatic Tachycardia Syndrome). I prioritize ‘first things first.’ If someone has poorly managed POTS, they cannot effectively perform physical therapy. We must stabilize the cardiovascular symptoms before we can focus on the spine."
Q: Does the Schroth Method require modification for the hypermobile body?
Campesi: "Yes, and it must. Individuals with EDS should avoid ‘end-of-range’ stretching. While some Schroth exercises involve elongation, we emphasize active muscle engagement—using your deep stabilizers—rather than passive hanging. I believe in making the exercise fit the person, not the other way around. If a patient is prone to subluxations or has ‘noisy’ joints, we adapt the position immediately."
Q: What is the primary goal for an adult with EDS and scoliosis?
Campesi: "For many, the goal is arresting progression and improving daily functionality. We provide a ‘toolkit’—strategies for using a lumbar roll, techniques for myofascial release, and, most importantly, the confidence to exercise. A person with EDS can exercise; it just may look different than the routine of a stiffer-bodied person at the gym."
Implications for the Patient Journey
The findings from experts like Campesi highlight a paradigm shift in how we manage spinal health. For the EDS patient, the path forward is not found in rigid, one-size-fits-all protocols, but in specialized, personalized, and adaptive care.
Key Takeaways for Patients:
- Advocate for Specialized Care: If you are seeking PT for scoliosis, ask specifically about the therapist’s experience with hypermobility. A great question to ask is: "What percentage of your patients have both scoliosis and EDS/HSD?"
- Prioritize Stability: Focus on exercises that build deep-layer muscle engagement rather than those that push joints to their end-range.
- Manage the Systemic Picture: If you suffer from dysautonomia or chronic fatigue, ensure these are being managed alongside your musculoskeletal issues. Your nervous system must be stable to support the muscular work required for spinal correction.
- Movement is Medicine: Research now suggests that active movement is a powerful tool against progression. Sedentary lifestyles can worsen the symptoms of both scoliosis and EDS.
Conclusion
Living with Ehlers-Danlos Syndrome requires a vigilant approach to health, and scoliosis is a primary component of that journey. While the diagnosis may feel daunting, the combination of advanced therapeutic systems like the Schroth Method and a deeper understanding of connective tissue disorders offers a hopeful roadmap. By prioritizing active stabilization, expert-guided movement, and systemic health management, individuals with EDS can successfully navigate the complexities of spinal health and maintain a higher quality of life.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional regarding your specific medical conditions and treatment plans.