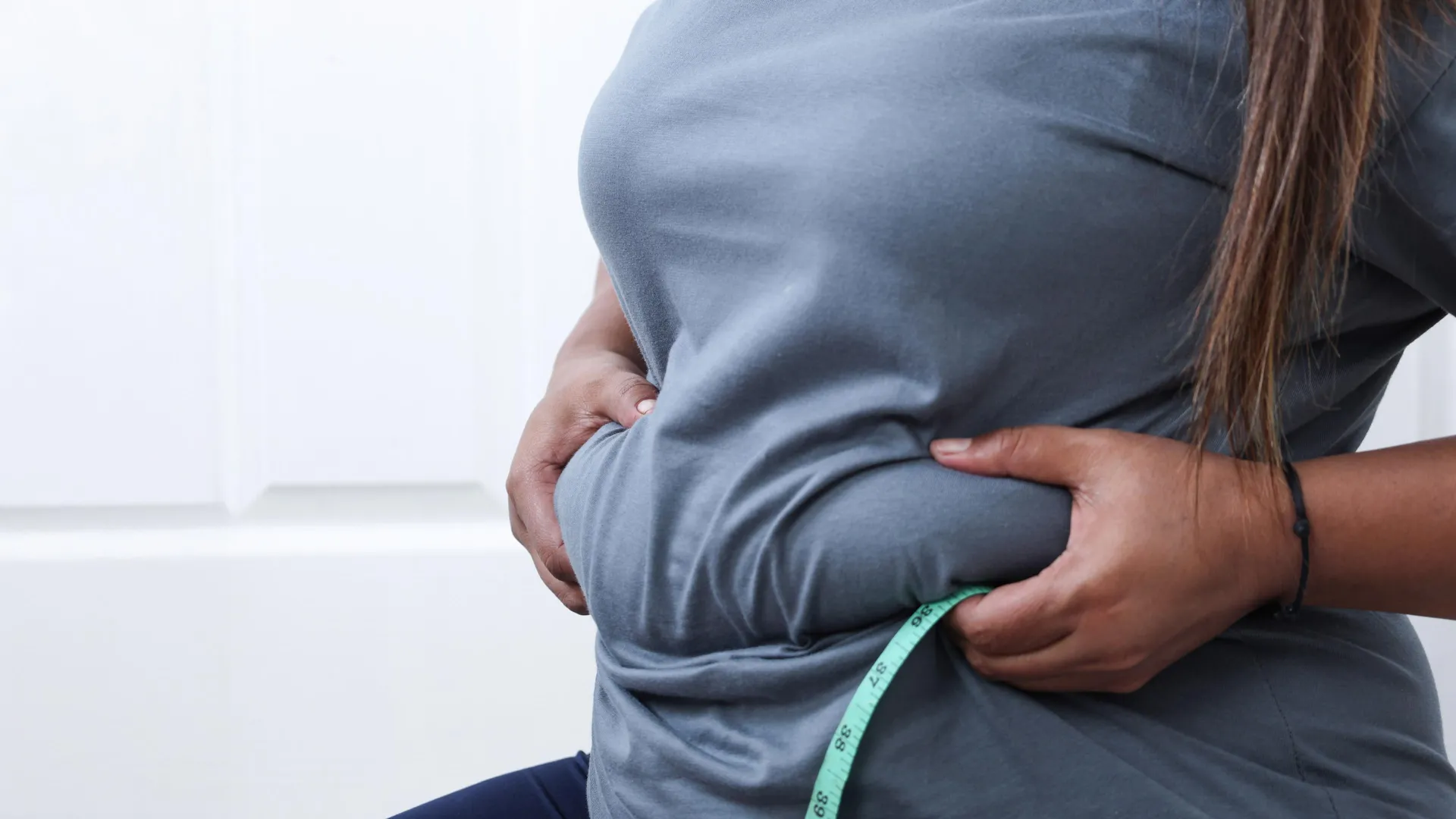
As the human body traverses the decades, it undergoes a silent, physiological metamorphosis. While the external changes—graying hair or thinning skin—are often the focus of societal vanity, a far more significant transformation occurs internally. As we age, the total volume of body fat increases, but more critically, its anatomical "real estate" shifts. This redistribution, often moving from peripheral, subcutaneous areas to the deep, visceral cavities, represents a major, under-discussed health challenge.
A groundbreaking study recently published in the journal Obesity Pillars suggests that we may finally be unlocking the mechanisms behind this shift. By exploring the nexus between testosterone and fat distribution, researchers are moving away from the "weight loss at all costs" mentality, instead advocating for a more nuanced, hormonally informed approach to aging and injury recovery.
The Anatomy of Aging: Subcutaneous vs. Visceral Fat
To understand the stakes, one must first distinguish between the two primary types of body fat. Most of the fat we can pinch—the subcutaneous layer—sits just beneath the skin. While often viewed as a cosmetic concern, subcutaneous fat serves vital biological functions, acting as an energy reservoir and a thermal insulator. It is generally considered benign, even necessary, for hormonal balance and overall vitality.
In contrast, visceral fat is the "silent killer" of the metabolic world. It builds up deep within the abdominal cavity, wrapping itself around vital organs like the liver, pancreas, and intestines. Unlike subcutaneous fat, visceral fat is metabolically active; it secretes inflammatory markers and hormones that disrupt the body’s normal functions. It is the primary culprit behind the increased risk of type 2 diabetes, cardiovascular disease, and chronic inflammation as we age.
As Jacob Earp, an assistant professor of kinesiology in the College of Agriculture, Health and Natural Resources (CAHNR) at the University of Connecticut, notes, this redistribution is a hallmark of the aging process. "As men and women age, there’s an unhealthy redistribution of fat from the more innocuous regions into the visceral compartment," Earp explains. "There is a direct link between sex hormones and fat distribution throughout the body."
The Flaw in Conventional Weight Loss
For decades, the standard medical advice for those carrying excess weight has been straightforward: consume fewer calories and move more. While effective for reducing the number on the scale, these "blanket" weight loss strategies often ignore the specific needs of the aging population.
When an older adult undergoes a calorie-restricted diet, the body does not simply melt away visceral fat. It often burns through precious muscle mass—a condition known as sarcopenia. In the elderly, muscle mass is the primary insurance policy against frailty, falls, and metabolic decline.
"Doing these blanket weight loss strategies is not always the healthiest approach," Earp warns, "especially because muscle weight will be lost along with fat, and maintaining muscle is extremely important as we age." Consequently, traditional dieting can sometimes leave an older person lighter, but metabolically more vulnerable and physically weaker.
Chronology of a Clinical Breakthrough
The quest for a more targeted intervention led Earp and his team to investigate whether hormonal therapy, specifically topical testosterone, could manipulate where the body stores fat. The target demographic for this study was women over the age of 65 who were in the critical recovery phase following a hip fracture.
The Catalyst: The Crisis of Hip Fractures
Hip fractures represent a watershed moment in the health of older women. They occur nearly three times more often in women than in men and are statistically linked to a rapid decline in independence. The subsequent period of immobilization is particularly dangerous; it triggers a cascade of muscle atrophy and metabolic stagnation. During this recovery period, the body naturally tends to pack on visceral fat, creating a "perfect storm" for long-term health complications.
The Methodology
The clinical trial followed 66 women, all over the age of 65, who had recently suffered a hip fracture. The study design was rigorous:
- Baseline Assessment: All participants underwent a DXA (Dual-energy X-ray Absorptiometry) scan to establish a baseline of their body composition, specifically measuring the ratio of visceral to subcutaneous fat.
- Standardized Rehabilitation: Every participant was enrolled in a structured, consistent exercise program tailored to their recovery stage.
- The Intervention: The cohort was divided into two groups. One group received a topical testosterone gel, while the other served as a control, receiving no hormonal intervention.
- The Six-Month Follow-up: After half a year of combined therapy and exercise, the participants were scanned again to observe changes in fat storage and body composition.
Supporting Data: When Hormones Change the Narrative
The results, as reported in Obesity Pillars, were striking for what they did—and did not—show. If one were to look only at the total weight of the participants, the study would appear unremarkable. Both groups showed similar levels of overall body weight change.
However, when the researchers peered beneath the surface, a clear divergence emerged. The group that did not receive the testosterone gel followed the expected, grim trajectory: their visceral fat levels increased, a common physiological response to the inactivity and stress of recovering from a major injury.
The testosterone group, however, bucked this trend entirely. Despite having similar overall body weights to the control group, they exhibited significantly lower levels of visceral fat. The hormone appeared to act as a metabolic compass, "telling" the body to avoid storing energy in the abdominal cavity and instead maintain a healthier, more distributed profile.
Official Perspectives and Expert Interpretation
The findings represent a paradigm shift in how clinicians view the role of testosterone in women’s health. Historically, testosterone has been categorized exclusively as a "male" hormone, leading to a significant delay in researching its therapeutic potential for women.
"If you have an injury and, just generally as we age, we expect an increase in visceral fat," Earp explains. "This [study] really bucked that trend and caused selective reduction of fat in that visceral compartment."
By decoupling weight loss from muscle loss, the study offers a blueprint for "healthy aging." The goal is no longer to be thin, but to be metabolically resilient. If clinicians can use targeted hormonal therapy to prevent the accumulation of deep-seated visceral fat during periods of recovery, they may be able to prevent the onset of secondary diseases like diabetes, which often plague seniors following an injury.
Implications for Future Medicine
The implications of this research extend far beyond the recovery room of a hip fracture ward. If confirmed by larger, long-term studies, this approach could change the standard of care for millions of aging individuals.
1. Reconceptualizing Recovery
Current rehabilitation protocols focus almost entirely on bone density and muscle strength. Incorporating metabolic management via hormonal therapy could ensure that patients don’t just "survive" the healing period but emerge with a metabolic profile that supports long-term health.
2. The Future of Hormone Replacement Therapy (HRT)
This study adds to the growing body of evidence suggesting that HRT, when administered with clinical precision and oversight, is a vital tool for age-related health management. It moves the conversation away from the controversial history of HRT and toward a modern, precision-medicine approach.
3. Improving Quality of Life
"These are devastating injuries that most women don’t ever recover from," says Earp. For the elderly, the difference between a successful recovery and a decline in health is often measured in the ability to walk to the grocery store or live independently. Any intervention that reduces the metabolic burden of visceral fat can contribute to higher energy levels, better mobility, and, ultimately, a significantly higher quality of life.
Conclusion: A New Horizon in Geriatric Care
The research led by Jacob Earp and his team serves as a poignant reminder that biology is not destiny. While the aging process dictates that our bodies will change, we are moving toward a time when we can actively influence the nature of that change.
By moving beyond the simplistic obsession with the scale and focusing on the complex, hormonal dance of body composition, we are beginning to see a future where aging does not automatically imply decline. As science continues to untangle the roles of hormones like testosterone, we may soon find that the most effective way to help our aging population is not just to help them move, but to help their bodies distribute energy in a way that fuels health, rather than undermining it.
The path forward will require further investigation into the long-term safety and efficacy of these treatments, but the initial findings are undeniably promising. For those recovering from injury, and for the millions of aging adults seeking to maintain their vitality, the message is clear: the secret to healthy aging may not be found in fewer calories, but in the intelligent, scientific management of our internal chemistry.