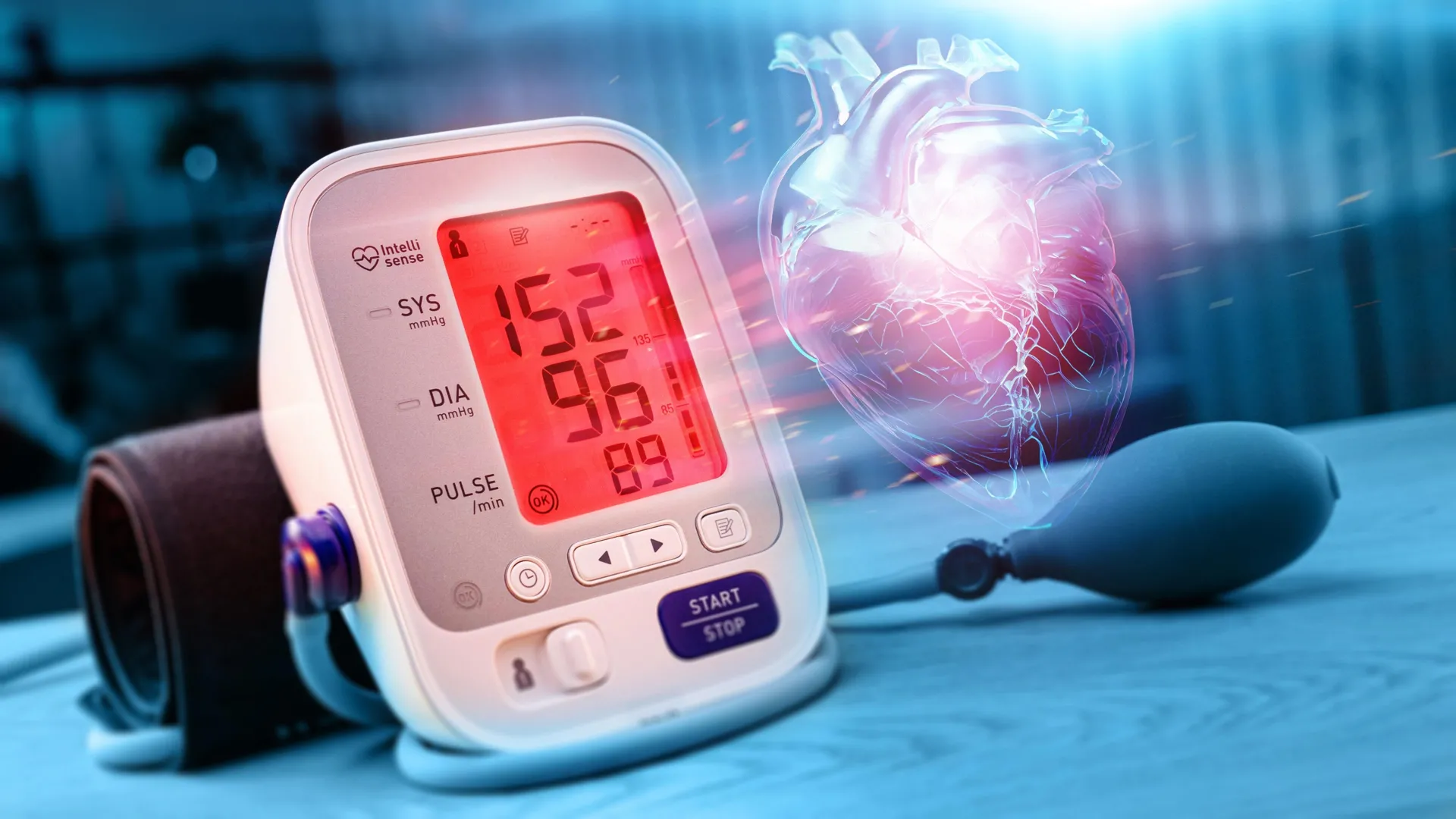
In a significant advancement for cardiovascular health research, a new study published today (November 17) in Hypertension, an American Heart Association journal, has unveiled a critical link between chronic pain and the development of high blood pressure. The findings suggest that the physical toll of persistent pain is not merely a localized issue but a systemic health concern that can significantly elevate the risk of life-threatening cardiovascular events.
For decades, clinicians have treated pain and hypertension as distinct medical challenges. However, this study, which analyzed health data from over 200,000 adults in the United States, reveals that the presence, location, and distribution of chronic pain are potent predictors of future hypertension. The study underscores a complex interplay between chronic physical discomfort, psychological well-being, and cardiovascular stability.
Understanding the Scope of the Cardiovascular Crisis
High blood pressure, or hypertension, remains the leading cause of death both nationally and globally. According to the 2025 joint guidelines from the American Heart Association (AHA) and the American College of Cardiology (ACC), hypertension is defined as blood pressure readings of 130/80 mm Hg or higher. It is a condition characterized by blood pressing too forcefully against vessel walls, which, if left unmanaged, drastically increases the likelihood of heart attack, stroke, and kidney failure.
Despite the widespread awareness of risk factors such as diet, physical inactivity, and genetics, the role of chronic pain has often been sidelined. With nearly half of all U.S. adults living with some form of hypertension, identifying novel risk factors—such as persistent musculoskeletal pain—is essential for public health interventions.
Chronology and Methodology: Tracking the Impact of Pain
The study, led by Dr. Jill Pell, the Henry Mechan Professor of Public Health at the University of Glasgow, was designed to investigate whether the duration and geography of pain correlate with the onset of hypertension over a long-term period.
Data Collection and Baseline Assessment
To ensure a robust analysis, researchers utilized a massive cohort of over 200,000 participants. At the baseline, each participant completed comprehensive questionnaires designed to measure their physical and mental health.
- Pain Mapping: Participants reported whether they had experienced pain in the previous month that interfered with their daily activities. Crucially, they identified the specific site of the pain, including the head, face, neck/shoulder, back, stomach/abdomen, hip, knee, or "widespread" pain (across the entire body).
- Duration: Participants were asked if these symptoms had persisted for more than three months, establishing the clinical definition of "chronic pain."
- Psychological and Inflammatory Markers: Depression was assessed using standardized tools measuring mood, disinterest, and lethargy. Meanwhile, inflammation was measured objectively through blood tests tracking C-reactive protein (CRP), a protein produced by the liver that spikes in response to inflammation.
The Long-Term Follow-Up
Following the initial assessment, the researchers tracked the cohort for an average of 13.5 years. This longitudinal approach allowed the team to observe the progression of health outcomes rather than relying on a snapshot, providing a clearer causal narrative between the onset of chronic pain and the subsequent diagnosis of high blood pressure.
Key Findings: The "Widespread" Risk Factor
The results of the 13.5-year follow-up were stark. The study found that individuals experiencing widespread chronic pain were significantly more likely to develop high blood pressure compared to those who reported no pain, transient discomfort, or pain localized to only one region.
Dr. Pell notes that the correlation is dose-dependent: "The more widespread their pain, the higher their risk of developing high blood pressure."
Perhaps most importantly, the researchers identified a mediating factor that bridges the gap between physical agony and vascular disease: depression. The data suggests that chronic pain often triggers or exacerbates depression, and it is this subsequent state of psychological distress that creates a biological environment conducive to hypertension. This "dual-pathway" suggests that for many, the road to hypertension is paved first by the stress of living with pain and the resulting impact on mental health.
Expert Perspective: Integrating Pain Management and Cardiology
Dr. Daniel W. Jones, M.D., FAHA, a prominent voice in the medical community and chair of the 2025 AHA/ACC High Blood Pressure Guideline, emphasized that while the short-term spike in blood pressure during acute pain is well-documented, the long-term, systemic effect of chronic pain has been vastly under-researched.
"This study adds to our understanding, finding a correlation between the number of chronic pain sites and that the association may be mediated by inflammation and depression," Dr. Jones stated. He points to the necessity of a paradigm shift in how we manage patients with chronic pain.
The Medication Paradox
One of the most pressing concerns highlighted by Dr. Jones is the role of medication. Millions of Americans rely on Nonsteroidal Anti-Inflammatory Drugs (NSAIDs) like ibuprofen to manage their daily pain. However, these medications are known to raise blood pressure.
"Chronic pain needs to be managed within the context of the patient’s blood pressure," Dr. Jones explained. "We have to be exceptionally careful that the treatment for pain does not inadvertently contribute to the development of hypertension."
Implications for Future Clinical Practice
The findings have profound implications for primary care providers. As Dr. Pell suggests, when a patient presents with chronic pain, the clinical focus should expand beyond musculoskeletal treatment to include cardiovascular screening.
1. Early Detection of Mental Health Needs
Because depression acts as a "bridge" between pain and hypertension, screening for mental health should become a routine component of pain management. By treating depression early in patients suffering from chronic pain, clinicians may potentially break the chain of events that leads to elevated blood pressure.
2. Holistic Patient Care
The study advocates for a multidisciplinary approach. Pain management specialists, cardiologists, and mental health professionals must communicate more effectively to treat the patient as a whole. This includes monitoring blood pressure regularly for any patient diagnosed with long-term musculoskeletal conditions like back, neck, or joint pain.
3. Future Research Directions
Dr. Jones recommends that the next phase of this research should involve randomized controlled trials. These trials would help determine whether specific pain management strategies—such as physical therapy, cognitive behavioral therapy, or non-NSAID medications—can actually reduce the risk of hypertension in chronic pain patients.
Study Limitations and Considerations
While the findings are groundbreaking, the authors were careful to note the limitations of the current study. The cohort consisted primarily of middle-aged and older white adults of British origin. Consequently, the researchers caution that these results may not be generalizable to younger populations or to individuals of different racial and ethnic backgrounds, who may experience chronic pain and cardiovascular disease through different social and biological lenses.
Furthermore, the study relied on self-reported pain levels and clinical diagnostic coding. Future research would benefit from more frequent blood pressure monitoring and a broader demographic reach to confirm that these findings hold true across diverse global populations.
Conclusion: A Call for Integrated Medicine
The research published today serves as a vital reminder that the human body functions as an integrated system rather than a collection of separate parts. Chronic pain is not merely a sensation to be masked by medication; it is a systemic signal that can have profound, long-term consequences for the heart.
By acknowledging the link between pain, depression, and blood pressure, the medical community can move toward a more proactive model of care. For the millions of people suffering from persistent discomfort, this research offers a pathway to better long-term health outcomes—one that prioritizes not just the relief of pain, but the protection of the cardiovascular system as a whole. As we continue to refine our understanding of these complex relationships, the integration of mental health support, cautious medication management, and proactive cardiovascular monitoring will be the cornerstones of effective, patient-centered care.