For millions living with Chronic Fatigue Syndrome (CFS)—also clinically recognized as Myalgic Encephalomyelitis (ME/CFS)—the struggle for vitality is a daily, often invisible battle. Characterized by profound, unrefreshing exhaustion and a debilitating cognitive "fog," the condition is perhaps best defined by its most cruel hallmark: post-exertional malaise (PEM), a severe worsening of symptoms following even minor physical or mental activity.
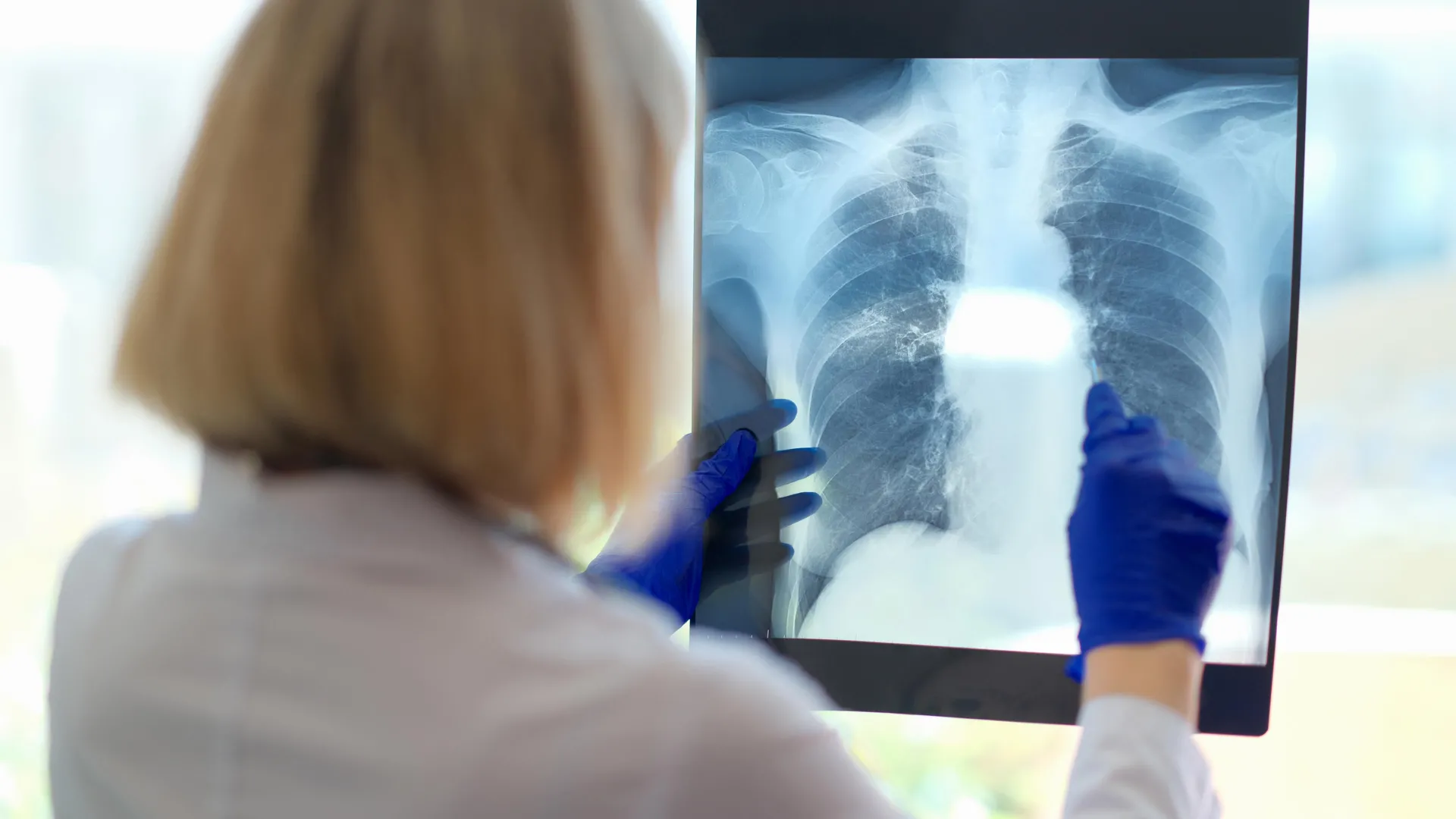
While the scientific community has long searched for the biological roots of this elusive condition, a groundbreaking study from the Icahn School of Medicine at Mount Sinai has shed light on a previously overlooked physiological mechanism: dysfunctional breathing. Researchers have discovered that a vast majority of patients with chronic fatigue suffer from irregular breathing patterns, suggesting that the very way these patients breathe may be compounding their exhaustion and fueling their malaise.
The Hidden Physiology: Defining the Link
The recent study, published in the journal Frontiers in Medicine, shifts the diagnostic lens toward the respiratory system. Researchers found that patients with CFS are significantly more prone to dysfunctional breathing and hyperventilation than the general population. This discovery is particularly vital because these breathing irregularities are not merely symptoms of the disease; they may be active contributors to the cycle of fatigue that defines the patient experience.
Dysfunctional breathing—a phenomenon often seen in asthma or anxiety-related conditions—manifests in several ways. It includes frequent, unnecessary deep sighing, rapid breathing cycles, forceful abdominal exhalations, or "chest breathing," which fails to engage the diaphragm. When the diaphragm is underutilized, the lungs cannot fully expand, and the muscles responsible for respiration fall out of sync.
The research team, led by senior author Dr. Benjamin Natelson and first author Dr. Donna Mancini, posits that these abnormalities are likely linked to dysautonomia. This is a disorder of the autonomic nervous system—the "autopilot" of the body—which governs unconscious processes like heart rate, blood pressure, and the regulation of blood vessels. When the autonomic nervous system is impaired, the body’s internal signals become garbled, potentially triggering the rapid, shallow, or irregular breathing patterns observed in the study.
A Chronology of Investigation: The Testing Protocol
To understand the relationship between CFS and respiratory health, the researchers conducted a rigorous two-day cardiopulmonary exercise testing (CPET) protocol. The study involved 57 participants diagnosed with chronic fatigue syndrome and a control group of 25 healthy individuals matched for age and activity levels.
Day One: Baseline and Capacity Assessment
The initial phase of the study focused on establishing a physiological baseline. Researchers monitored the participants’ heart rate, blood pressure, and oxygen uptake efficiency. A critical metric was "peak VO2 max," which measures the maximum amount of oxygen a person can utilize during intense exercise. Surprisingly, the study found that the peak VO2 max levels between the CFS group and the control group were similar, suggesting that the underlying lung capacity of the patients was not inherently compromised.
Day Two: Stress-Testing the System
The second day focused on the body’s reaction to exertion. By analyzing breathing rate and patterns during physical stress, the team identified the presence of hyperventilation and dysfunctional breathing. The data revealed a stark contrast between the two groups. While the control group remained relatively stable, the CFS cohort showed a chaotic respiratory response to the exertion, providing empirical evidence that their breathing mechanisms struggle to maintain homeostasis under stress.
Supporting Data: The Scale of the Discrepancy
The statistics unearthed by the researchers are striking and highlight a widespread, yet previously "unappreciated" issue in clinical practice.
- Prevalence of Dysfunction: A staggering 71% of the chronic fatigue group exhibited significant breathing abnormalities, including hyperventilation, dysfunctional breathing, or a combination of both.
- The Control Comparison: Nearly half of the CFS participants displayed irregular breathing during the testing, compared to only four individuals in the control group.
- Hyperventilation Rates: One-third of the CFS patients suffered from hyperventilation, a condition that was essentially absent in the control group, where only one person displayed similar symptoms.
- The Combined Effect: Nine patients in the study suffered from both hyperventilation and dysfunctional breathing—a combination that was completely nonexistent among the healthy control subjects.
These numbers suggest that breathing issues are not just a peripheral symptom but a core component of the CFS clinical profile. Because these symptoms—dizziness, difficulty concentrating, and shortness of breath—overlap perfectly with the known symptoms of CFS, they have likely been misattributed to the primary condition, leaving the underlying respiratory dysfunction untreated.
Official Perspectives: The Experts Speak
Dr. Benjamin Natelson, a prominent figure in the study of chronic fatigue, emphasized the significance of these findings during the study’s release. "Nearly half of our chronic fatigue subjects had some disorder of breathing—a totally unappreciated issue, probably involved in making symptoms worse," Dr. Natelson noted. He expressed optimism that this newfound focus on respiratory health will pave the way for novel therapeutic strategies.
Dr. Donna Mancini, who served as the study’s first author, addressed the silent nature of these abnormalities. "While we know the symptoms generated by hyperventilation, we remain unsure what symptoms may be worse with dysfunctional breathing," she explained. "But we are sure patients can have dysfunctional breathing without being aware of it. Dysfunctional breathing can occur in a resting state."
The researchers believe that the link between dysautonomia and respiratory dysfunction is a primary suspect. "Possibly dysautonomia could trigger more rapid and irregular breathing," Dr. Mancini added. She highlighted "orthostatic intolerance"—the inability to remain upright without symptoms—as a key trigger. In this state, the heart rate spikes to compensate for poor blood flow regulation, which in turn forces the patient into a cycle of rapid, shallow breathing that can lead to hyperventilation.
Clinical Implications: The Path to "Pulmonary Physiotherapy"
The most encouraging aspect of this study is the potential for non-invasive, effective intervention. If breathing patterns are indeed exacerbating the exhaustion experienced by CFS patients, then "re-training" the breath could offer a pathway to symptom relief.
Potential Therapeutic Avenues:
- Biofeedback: Using technology to measure exhaled carbon dioxide (CO2) levels, patients can learn to identify when they are beginning to hyperventilate. By consciously reducing the depth and frequency of their breaths, they can restore balance to their CO2 levels, thereby mitigating symptoms like dizziness and palpitations.
- Guided Conditioning: Natelson suggests that gentle physical conditioning, such as swimming or specific yoga practices, could be beneficial. These activities emphasize controlled, rhythmic breathing, which may help re-synchronize the diaphragm and chest muscles.
- Diaphragmatic Re-education: For patients who have developed a habit of "chest breathing," physical therapy aimed at restoring the use of the diaphragm could reduce the muscular effort required to breathe, effectively lowering the overall energy expenditure of the patient.
The Future of Chronic Fatigue Management
While the researchers caution that more studies are required before these methods are recommended as standard clinical practice, the implications are profound. For a disease that has historically been dismissed or treated only through psychiatric lenses, identifying a concrete, physical, and measurable dysfunction like "dysfunctional breathing" is a massive step forward.
By addressing the way a patient breathes, clinicians may be able to reduce the severity of post-exertional malaise. Even if these breathing interventions do not "cure" CFS, they may act as a vital tool in symptom management, allowing patients to reclaim a degree of agency over their physical state.
As the medical community continues to peel back the layers of Chronic Fatigue Syndrome, this research serves as a reminder that the most significant breakthroughs often come from looking at the most fundamental of human functions. Sometimes, the key to surviving a complex, multisystem disease is as simple—and as difficult—as learning how to catch your breath.