By TCTMD Editorial Staff
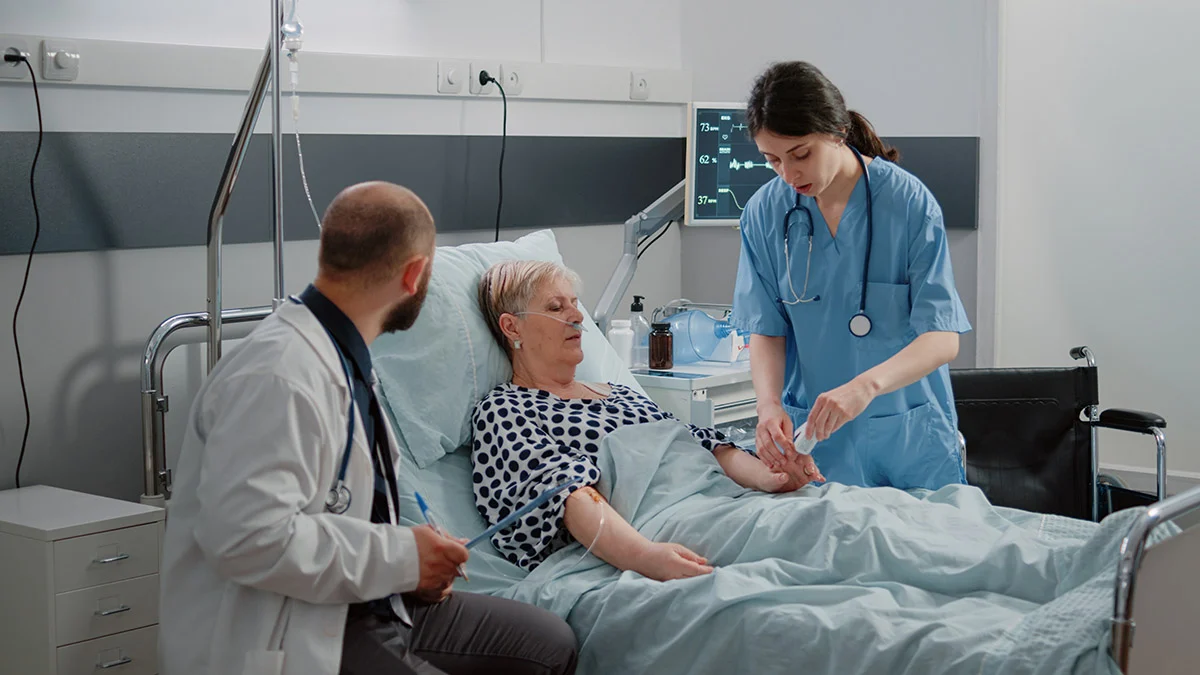
For decades, the administration of supplemental oxygen has been a cornerstone of emergency cardiac care. It is a therapy so deeply ingrained in clinical practice that it is often viewed as a benign, reflexive intervention for any patient presenting with respiratory distress. However, new data from the REDOX-AHF trial, presented at the European Society of Cardiology’s Heart Failure 2026 meeting in Barcelona, suggests that the "more is better" approach to oxygenation may be fundamentally flawed.
The trial provides the first blinded, randomized evidence that a restrictive oxygenation strategy—targeting lower saturation levels—is not only safe but potentially superior to the liberal strategies currently employed in most hospital settings. By prioritizing decongestion and potentially improving survival, this study challenges clinicians to reconsider the "high-flow" habits that have defined heart failure management for over a century.
The Clinical Context: A Century of Assumptions
Oxygen supplementation has been a standard treatment for acute heart failure (HF) and dyspnea for over 100 years. Clinicians have traditionally operated under the assumption that keeping oxygen saturation levels high—often targeting 96% or above—is a harmless way to alleviate symptoms and protect the myocardium from the ravages of hypoxemia.
Current guidelines, including those from the European Society of Cardiology (ESC) published in 2021, offer a Class I, level C recommendation for oxygen in patients with peripheral oxygen saturation (SpO2) below 90% or partial pressure of oxygen (PaO2) below 60 mm Hg. However, the guidelines remain conspicuously silent on a ceiling for oxygenation. There is no formal recommendation against maintaining higher saturation levels, leading many physicians to default to liberal oxygen supplementation.
Dr. Ida Arentz Taraldsen, lead investigator from the University of Copenhagen, highlights the irony of this practice. "Oxygen acts as a vasodilator in the pulmonary arteries but as a vasoconstrictor in the coronary arteries," she noted. "How those interact in acute heart failure is uncertain. The reality is that oxygen may have deleterious effects on cardiac function that we have historically overlooked." With up to 75% of patients hospitalized with acute heart failure receiving supplemental oxygen, the potential for systemic over-oxygenation is significant.
Chronology of the REDOX-AHF Trial
The REDOX-AHF study was designed to move beyond anecdotal practice and provide the rigorous data needed to update clinical standards. The trial enrolled 135 patients across two centers, specifically targeting those admitted with acute heart failure who presented with subjective dyspnea, clinical or radiological signs of pulmonary congestion, and baseline SpO2 levels of 92% or lower.
Trial Design and Methodology
The trial was notable for its use of an automated oxygen administration device, which allowed for double-blinding—a critical feature for minimizing bias in a study where subjective patient reports (dyspnea) are a primary outcome. Participants were randomized into two distinct arms:
- The Restrictive Group: Targeted an SpO2 of 90%.
- The Liberal Group: Targeted an SpO2 of 96%.
The demographics of the cohort reflected the typical heart failure population: a mean age of approximately 78 years, with a nearly equal gender split (52% female). The group presented with a mean left ventricular ejection fraction (LVEF) of roughly 40%, with 23% having reduced ejection fraction and 20% having preserved ejection fraction. Baseline NT-proBNP levels were high in both groups, confirming the acuity of their heart failure status.
Implementation and Adherence
The study maintained high standards for internal validity. Diuretic dosing—a potential confounding variable in decongestion—was kept consistent between the two groups. Time within the target interval was comparable, with the restrictive group spending 58.5% of the time within their target range and the liberal group spending 54.2% in theirs. Most importantly, the risk of harm from hypoxia was managed effectively, with less than 2% of patients in the entire cohort experiencing severe hypoxia (SpO2 < 85%).
Supporting Data: Decongestion and Clinical Outcomes
The primary endpoint of the study focused on the change in lung fluid content over the first 24 hours of hospitalization. This was measured using remote dielectric sensing (ReDS) technology, a precise method for quantifying pulmonary congestion.
The Superiority of the Restrictive Approach
The results were compelling:
- Restrictive Group: Mean lung fluid content dropped from 33.3% at baseline to 30.9% at 24 hours.
- Liberal Group: Mean lung fluid content dropped from 35.2% to 34.0%.
On multivariable analysis, the estimated between-group difference in lung fluid reduction was 2.4% (P = 0.01). This significant drop in fluid suggests that lower oxygen targets may facilitate more efficient decongestion. Furthermore, these results were consistent across various patient subgroups, including those with varying LVEF, age, renal function, and body mass index, indicating that the benefits of the restrictive strategy are likely broadly applicable.
Secondary and Exploratory Findings
While the primary focus was on fluid, the secondary and exploratory data offered a glimpse into long-term patient health. By 30 days, patients in the restrictive arm enjoyed a greater number of days alive and out of the hospital (a median of 23 days) compared to those in the liberal arm (a median of 21 days; P = 0.04).
Additionally, there was a positive trend regarding all-cause mortality, which was numerically lower in the restrictive group (4.6% vs. 10.1%), although this did not reach statistical significance. Lengths of stay were also shorter in the restrictive group (4.7 days vs. 6.4 days), though again, the P-value (0.26) suggests that larger studies are needed to confirm these gains in efficiency. Crucially, the "restrictive" group did not report higher levels of dyspnea, suggesting that the clinical goal of patient comfort was not compromised by the lowered oxygen targets.
Official Responses and Expert Perspective
The medical community has reacted with cautious optimism to the findings presented at the ESC Heart Failure meeting. Dr. Maja Cikes of the University Hospital Centre Zagreb, who served as the trial discussant, lauded the study for its pragmatic design and high clinical relevance.
"It is likely unnecessary to insist on liberal oxygenation targets," Dr. Cikes stated during her remarks. "In other words, do consider restrictive oxygenation targets." She emphasized that while hypoxia is a natural physiological challenge that must be addressed, hyperoxia is an "iatrogenic" intervention—a state introduced by the physician—that may be significantly more taxing for the heart and lungs to process.
Dr. Cikes highlighted that the trial effectively bridges the gap between theoretical cardiovascular physiology and bedside practice. By demonstrating that oxygen is not a "harmless" drug, the REDOX-AHF trial has provided a necessary counter-narrative to the standard of care that has persisted for generations. However, she was quick to note that while the results are promising, they should be viewed as an invitation for larger, multicenter randomized controlled trials (RCTs) to definitively establish new global guidelines.
Clinical Implications: A Paradigm Shift?
The implications of the REDOX-AHF study extend far beyond the emergency department. If these findings are corroborated by larger studies, they could necessitate a fundamental shift in how hospitals manage acute heart failure.
Reducing Iatrogenic Harm
The primary shift in mindset involves recognizing that hyperoxia—the over-administration of oxygen—is a potential clinical harm. Given that oxygen can induce vasoconstriction in the coronary arteries, reducing excessive oxygen levels may alleviate some of the stress placed on the heart during an acute failure event. This could potentially reduce the workload on the heart, allowing for better management of pulmonary congestion.
Resource Allocation and Cost
The data regarding length of stay and "days alive and out of the hospital" suggest that a restrictive oxygen strategy could have significant economic and resource-management benefits. Shorter hospitalizations reduce the burden on healthcare systems and decrease the risk of hospital-acquired infections or complications, which are prevalent in the elderly, high-risk heart failure population.
Future Research Directions
The investigators of REDOX-AHF acknowledge that while 135 patients provided significant insights, a larger, phase III trial is the necessary next step. Future research will likely focus on:
- Long-term mortality outcomes: Establishing if the numerical trend toward lower mortality becomes statistically significant in larger populations.
- Diverse demographics: Ensuring that the benefits of restrictive oxygenation hold true across international populations with different nutritional and environmental backgrounds.
- Automated monitoring: Evaluating whether the "closed-loop" or automated oxygen administration used in the trial can be scaled for general use, ensuring that patients receive the exact dose required to maintain a 90% threshold without human error.
Conclusion: Less May Indeed Be More
The REDOX-AHF trial serves as a wake-up call to the cardiology community. For too long, the administration of supplemental oxygen in heart failure has been a "set it and forget it" practice. The evidence now suggests that a more nuanced, restrictive approach—one that avoids the potential dangers of hyperoxia—can lead to better decongestion, improved quality of life, and potentially better survival.
As clinicians move forward, the message is clear: the goal of treatment should be to correct hypoxemia, not to chase the highest possible saturation numbers. In the delicate balance of acute heart failure management, it appears that, when it comes to oxygen, less is not only more—it is better.