Chronic wounds—those stubborn, non-healing lesions that persist for months or even years—have long been considered a "silent epidemic" of modern medicine. For the millions of individuals suffering from diabetic foot ulcers, venous leg ulcers, or persistent pressure injuries, these wounds represent more than just physical discomfort; they are a gateway to systemic infection, profound disability, and, in severe cases, life-altering amputations.
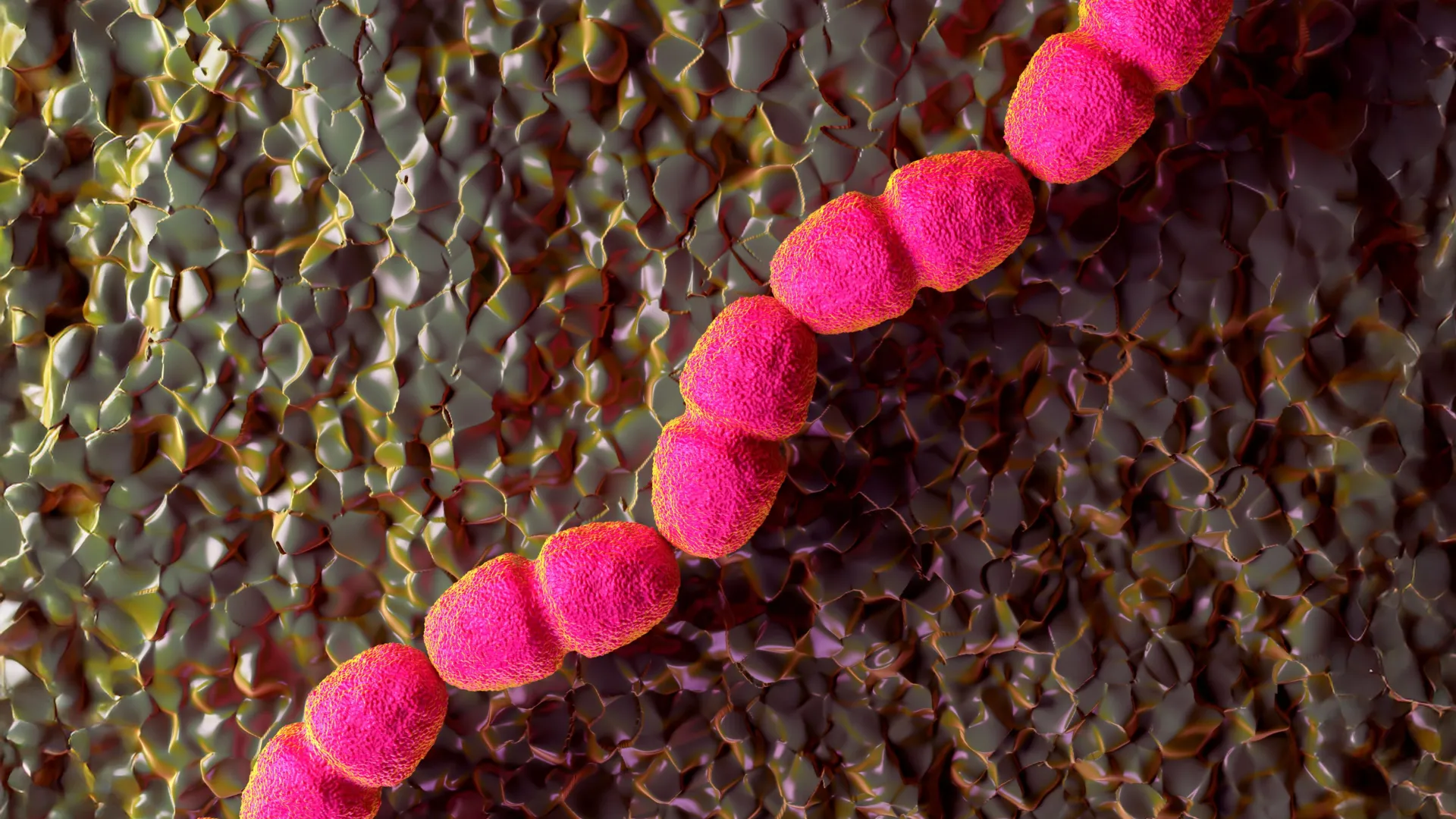
Now, an international research team led by Nanyang Technological University, Singapore (NTU Singapore), in collaboration with the University of Geneva, has unlocked a critical mystery that has baffled clinicians for decades. By identifying the precise biological mechanism by which the common bacterium Enterococcus faecalis (E. faecalis) sabotages the body’s repair processes, researchers have paved the way for a revolutionary treatment approach that shifts the focus from killing bacteria to neutralizing the "metabolic weapons" they wield.
The Silent Epidemic: The Global Burden of Chronic Wounds
Chronic wounds represent a mounting challenge to global healthcare systems. With an aging global population and the rising prevalence of metabolic diseases like diabetes, the number of people requiring long-term wound care is surging.
Current data highlights the staggering scale of the issue:
- Diabetic Foot Ulcers: Each year, approximately 18.6 million people worldwide develop these debilitating wounds. In fact, it is estimated that as many as one in three individuals with diabetes will face a foot ulcer at some point in their lifetime.
- The Amputation Crisis: Chronic wounds are a leading cause of non-traumatic lower limb amputations. The cycle of infection and failed healing often leads to tissue necrosis, necessitating surgical intervention to save the patient’s life.
- Regional Impact: In Singapore alone, over 16,000 cases of chronic wounds are reported annually. These cases are concentrated among the elderly and the diabetic population, creating a significant strain on specialized clinics and nursing resources.
The fundamental problem is that these wounds are not just "slow to heal"—they are actively prevented from healing. While clinicians have known for years that infection complicates the recovery process, the exact "how" and "why" remained a medical enigma until now.
Chronology of a Discovery: Unmasking E. faecalis
The journey to this discovery began with a shift in perspective. Instead of viewing E. faecalis merely as a hostile invader, researchers sought to understand its metabolic footprint within the microenvironment of a wound.
Phase 1: Identifying the Saboteur
E. faecalis is an opportunistic pathogen frequently isolated from chronic, non-healing wounds. Its ability to persist in harsh environments and develop resistance to multiple classes of antibiotics has made it a nightmare for infectious disease specialists.
Phase 2: The Role of Extracellular Electron Transport (EET)
The research team, led by NTU Associate Professor Guillaume Thibault and Professor Kimberly Kline of the University of Geneva, discovered that E. faecalis employs a unique metabolic strategy known as extracellular electron transport (EET). Unlike other pathogens that rely on the secretion of aggressive toxins to damage tissue, E. faecalis produces hydrogen peroxide as a metabolic byproduct of its EET pathway.
Phase 3: The Cellular Paralyzer
The researchers observed that the hydrogen peroxide generated by these bacteria creates a state of chronic oxidative stress in human skin cells, specifically keratinocytes. In a healthy wound, keratinocytes must migrate to the site of injury to "seal" the breach. However, the study found that this specific oxidative stress triggers the "unfolded protein response" (UPR) in the skin cells.
While the UPR is a natural protective mechanism designed to help cells manage stress, its prolonged activation by E. faecalis essentially freezes the cells. The keratinocytes become so preoccupied with managing the protein damage caused by the bacterial hydrogen peroxide that they lose their ability to move, effectively stalling the wound-healing process.
Supporting Data: Validating the Mechanism
To confirm that the EET pathway was indeed the culprit, the team utilized a genetically modified strain of E. faecalis that lacked the capacity for EET. The results were definitive: without the ability to produce high levels of hydrogen peroxide, the genetically altered bacteria failed to inhibit the migration of keratinocytes.
The researchers then performed a "rescue" experiment. They introduced catalase—an antioxidant enzyme that naturally breaks down hydrogen peroxide—to the infected cell cultures. The results were transformative: once the hydrogen peroxide was neutralized, the oxidative stress subsided, and the keratinocytes regained their mobility, effectively "unlocking" the wound-healing process.
Official Responses: Shifting the Paradigm of Infection Control
The implications of these findings for the medical community are profound. For decades, the gold standard for treating infected wounds has been the use of antibiotics. However, with the rise of multi-drug resistant (MDR) bacteria, this strategy is losing its efficacy.
"Our findings show that the bacteria’s metabolism itself is the weapon, which was a surprise finding previously unknown to scientists," said Assoc Prof Guillaume Thibault, who serves as Assistant Dean (International Engagement) at NTU’s College of Science.
Prof. Thibault emphasizes that the discovery moves the focus away from a futile arms race against bacterial evolution. "Instead of focusing on killing the bacteria with antibiotics, which is becoming increasingly difficult and leads to future antibiotic resistance, we can now neutralize it by blocking the harmful products it generates and restoring wound healing. We are targeting the cause of the chronic nature of the wound—the reactive oxygen species—rather than just the source."
The collaborative nature of the study, involving experts from the Singapore Centre for Environmental Life Sciences and Engineering (SCELSE), underscores the multidisciplinary approach required to solve complex medical problems. By bridging the gap between microbiology and cellular biology, the team has identified a therapeutic window that exists entirely outside the traditional antibiotic framework.
Future Implications: From Lab Bench to Bedside
The research team is already looking toward the future, with the goal of translating these laboratory successes into clinical reality. Because catalase and other antioxidants are already well-characterized and understood in medical and industrial applications, the regulatory pathway for developing treatments based on this discovery may be significantly shorter than that of a novel synthetic drug.
Proposed Clinical Strategies:
- Antioxidant-Infused Dressings: The most immediate application is the development of advanced wound dressings embedded with enzymes like catalase. These dressings would act as a "sink," absorbing the hydrogen peroxide produced by the bacteria as it is released, thereby keeping the wound microenvironment conducive to healing.
- Topical Therapies: Beyond dressings, the research points toward topical formulations that could be applied directly to diabetic ulcers to stabilize the skin cell environment and kickstart the migration process.
- Combination Therapy: While the focus is on neutralizing metabolic byproducts, this strategy could be used in tandem with targeted antimicrobial agents, potentially allowing for lower, more effective doses of antibiotics that do not trigger the same resistance pathways.
The Road Ahead: Clinical Trials
The team is currently conducting studies in animal models to determine the most effective delivery systems for these antioxidants. Once the efficacy and safety profile are fully established in these models, the researchers intend to transition to human clinical trials.
If successful, this approach would represent a paradigm shift in wound care. It offers a solution not only for E. faecalis infections but potentially for other bacterial species that utilize similar metabolic pathways to suppress the immune system and inhibit tissue repair.
Conclusion
The findings published in Science Advances represent a major milestone in the fight against chronic wounds. By identifying the "metabolic weapon" used by E. faecalis, researchers have provided a roadmap for treating infections that are currently resistant to our most potent antibiotics.
As we move closer to clinical trials, the prospect of an "antioxidant-based" treatment for chronic ulcers offers newfound hope to millions. It is a testament to the power of curiosity-driven research: by asking not just how to kill a pathogen, but how a pathogen interacts with the host, science has once again found a way to turn the tide against a persistent and dangerous foe. For patients living in the shadow of chronic, non-healing wounds, this discovery marks the beginning of a potential end to a cycle of pain, infection, and loss.