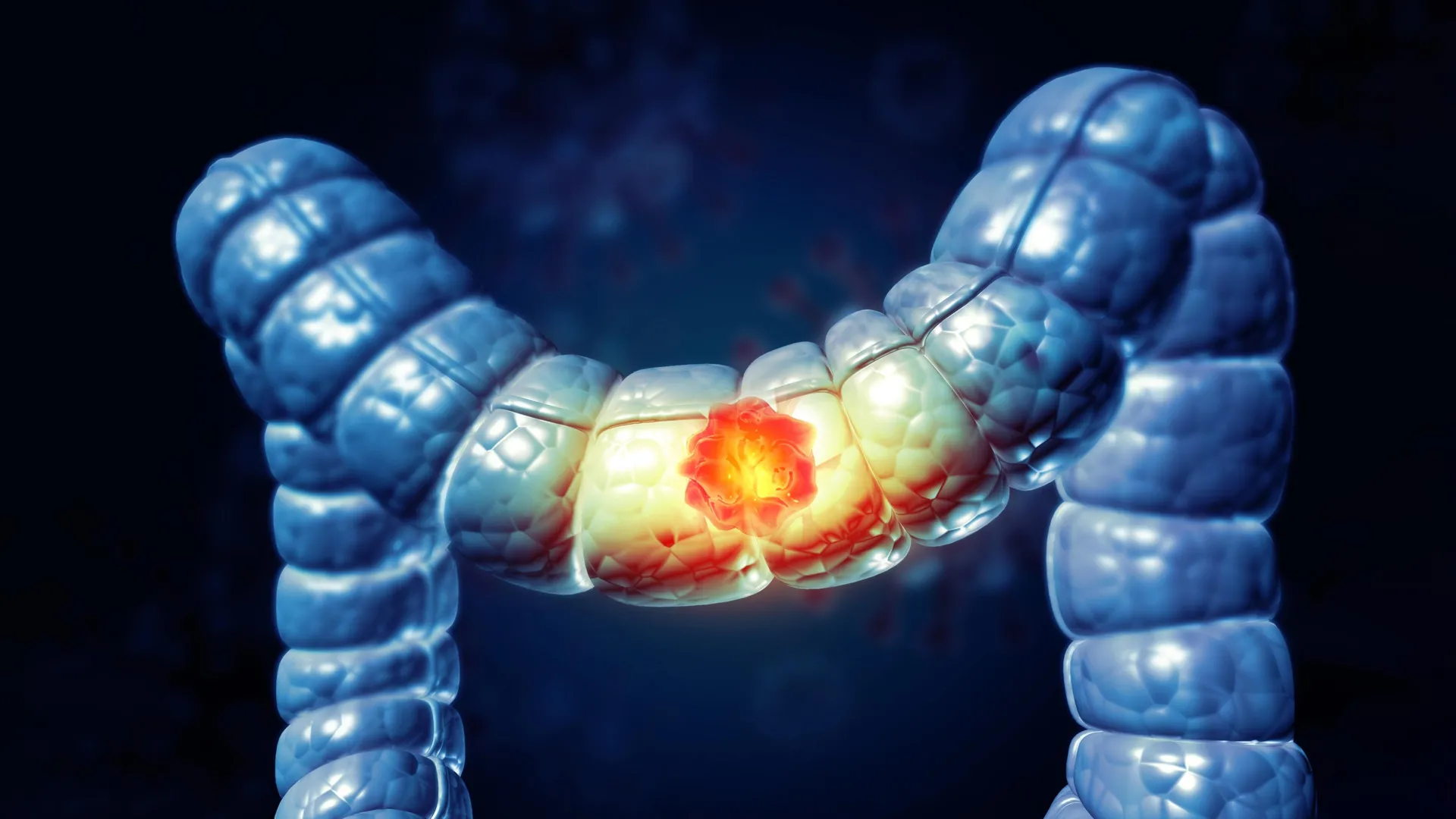
In a landmark development for cancer care, a new clinical trial has unveiled a potential paradigm shift in the treatment of colorectal cancer. The NEOPRISM-CRC study, led by researchers at University College London (UCL) and University College London Hospitals (UCLH), has demonstrated that a short, targeted course of immunotherapy administered prior to surgery can lead to extraordinary long-term outcomes for patients with high-risk bowel cancer.
The results, presented at the American Association for Cancer Research (AACR) Annual Meeting 2026 in San Diego, show that patients treated with the immunotherapy drug pembrolizumab have remained cancer-free for nearly three years, effectively bypassing the need for traditional, often grueling, post-surgical chemotherapy.
Main Facts: A Paradigm Shift in Treatment
For decades, the standard of care for stage two and three colorectal cancer has involved a sequence of surgery followed by several months of chemotherapy. While effective, this regimen is associated with significant side effects and a non-negligible risk of recurrence. The NEOPRISM-CRC trial challenges this status quo.
The study focused on a specific genetic subtype of the disease known as "MMR deficient/MSI-high" (mismatch repair deficient/microsatellite instability-high) colorectal cancer. This subtype, which occurs in approximately 10–15% of such cases—roughly 2,000 to 3,000 patients in the UK annually—is characterized by a specific set of mutations that make the tumor more visible to the immune system.
By administering pembrolizumab for just nine weeks before surgery, researchers observed a "melting away" of tumors in many participants. Most notably, the 33-month follow-up data reveals that zero patients in the trial have experienced a cancer recurrence, a stark contrast to the standard treatment pathway where approximately 25% of patients typically see their cancer return within three years.
Chronology of the NEOPRISM-CRC Trial
The journey of the NEOPRISM-CRC trial represents a meticulous approach to clinical innovation.
- Initial Enrollment and Treatment: The trial recruited 32 patients diagnosed with stage two or three colorectal cancer harboring the MMR-deficient subtype. Participants were transitioned from the conventional "surgery-first" model to a "neoadjuvant" (pre-surgical) immunotherapy model.
- The Nine-Week Window: Over a span of nine weeks, participants received doses of pembrolizumab. This intervention was designed to prime the immune system to recognize and destroy malignant cells before the physical removal of the tumor.
- Surgical Intervention: Following the immunotherapy course, patients underwent surgery. In several instances, surgeons were shocked to find that the tumors had either been eradicated entirely or reduced to minimal, non-viable remnants.
- The Monitoring Phase: Post-surgery, the cohort entered an intensive monitoring period. Unlike the standard treatment protocol, these patients did not receive adjuvant chemotherapy.
- The 33-Month Milestone: As of the 2026 reporting, the study reached a critical 33-month follow-up point. The sustained absence of disease across the entire participant group serves as a powerful testament to the efficacy of the neoadjuvant approach.
Supporting Data and Biological Insights
The success of the trial is supported by sophisticated diagnostic tools. The research team, in collaboration with the biotech firm Personalis, utilized personalized blood tests to monitor the presence of circulating tumor DNA (ctDNA).
Predictive Power of Blood Profiling
Researchers discovered that the disappearance of tumor DNA from the bloodstream served as a highly accurate biomarker for long-term success. Yanrong Jiang, the study’s first author, noted that the ability to track patients using these "liquid biopsies" provided immediate, real-time feedback on how the body was responding to the immunotherapy.
"When tumor DNA disappeared from the blood, patients were much more likely to have no cancer remaining, and this matched the long-term results we’re now seeing," Jiang explained. This data suggests that doctors may soon be able to determine, with high precision, whether a patient has achieved a complete response, potentially allowing for the omission of invasive surgeries or unnecessary follow-up treatments.
The Role of Immune Profiling
Beyond liquid biopsies, the team conducted detailed immune profiling of tumor tissue before the first cycle of treatment. This process identified specific immune markers that predict whether a patient will respond favorably to pembrolizumab. By understanding the biological environment of the tumor before intervention, clinicians can better tailor therapies, sparing patients from ineffective treatments while identifying those who require more aggressive care.
Official Responses and Expert Perspectives
The clinical community has met the findings with cautious optimism and, in some quarters, profound excitement.
Dr. Kai-Keen Shiu, Chief Investigator of the trial and a Consultant Medical Oncologist at UCLH, emphasized the safety and transformative potential of the results. "Seeing that no patients have experienced a cancer recurrence after almost three years of follow-up is extremely encouraging," Dr. Shiu stated. "It strengthens our confidence that pembrolizumab is a safe and highly effective treatment to improve outcomes in patients with high-risk bowel cancers."
Dr. Shiu further highlighted the future of personalized medicine: "What is particularly exciting is that we now may be able to predict who will respond to the treatment using personalized blood tests and immune profiling. These tools could help us tailor our approach, identifying patients who are doing well and may need less therapy versus patients at higher risk of disease progression who need additional intervention."
Professor Marnix Jansen, also from the UCL Cancer Institute, underscored the significance of the biological insights gained. "These results not only confirm the durability of responses we saw almost three years ago, but also provide crucial biological insights into why immunotherapy is so effective in this setting."
Patient Story: A Real-World Perspective
The clinical data is anchored by the lived experience of patients like 73-year-old Christopher Burston. Diagnosed in February 2023 following a routine screening, Mr. Burston was faced with the daunting prospect of stage three colorectal cancer.
"I saw the images when I had the first colonoscopy and could see it was really quite a substantial lump," Burston recalled. After joining the NEOPRISM trial, he received three doses of immunotherapy. By the time he underwent surgery in May 2023, the results were definitive. "The outcome of the surgery was essentially that the cancer had melted away," he noted.
Three years later, Mr. Burston describes himself as feeling "back to normal," enjoying a life largely unburdened by the shadow of his previous diagnosis. His story highlights the dual benefit of the treatment: the clinical eradication of the tumor and the preservation of quality of life, avoiding the toxicity often associated with prolonged chemotherapy.
Implications for Future Cancer Care
The implications of the NEOPRISM-CRC trial are vast, touching upon public health, clinical protocol, and the broader economics of cancer treatment.
Changing the Standard of Care
Bowel cancer is the fourth most common cancer in the UK, with roughly 44,000 new cases diagnosed annually. While survival rates vary significantly by stage—ranging from 90% at stage one to just 10% at stage four—the shift toward neoadjuvant immunotherapy could redefine the survival curve for the 10-15% of patients with MMR-deficient tumors.
Economic and Health System Impact
By identifying which patients respond to short-course immunotherapy, health services may be able to significantly reduce the costs and resource utilization associated with long-term chemotherapy, hospitalizations for side-effect management, and the high costs of treating cancer recurrence.
The Rise of Precision Oncology
The integration of personalized blood tests into routine care is perhaps the most significant long-term takeaway. As these tests become more accessible and standardized, they move oncology closer to a model where treatment is dynamic and adaptive. Instead of "one-size-fits-all" protocols, clinicians can pivot based on the molecular signals emitted by the tumor itself.
Future Research Directions
While the results are groundbreaking, the research team remains focused on the next steps. Future trials will aim to see if these findings can be replicated in larger, more diverse patient populations and whether this immunotherapy approach can be applied to other, more common subtypes of colorectal cancer.
In conclusion, the NEOPRISM-CRC trial stands as a beacon of progress in the fight against cancer. By combining the precision of modern genomics with the power of the human immune system, researchers have provided a glimpse into a future where "cancer-free" is not just a hope, but an expected outcome for high-risk patients. As the trial continues to inform clinical practice, it promises to spare thousands of patients from the ravages of advanced disease and the toxicity of traditional treatments, marking a definitive victory in the evolution of modern medicine.