In an era of increasing mental health awareness, the vocabulary of psychology has entered the mainstream. Terms like "depressed," "anxious," and "traumatized" are frequently used in casual conversation to describe everyday fluctuations in mood. However, mental health professionals warn that conflating the natural human emotion of sadness with the clinical medical condition of depression can lead to significant misunderstandings regarding treatment and recovery.
While sadness is an adaptive, necessary response to life’s inevitable hardships, clinical depression—formally known as Major Depressive Disorder (MDD)—is a complex physiological and psychological condition that requires targeted intervention. Understanding where the boundary lies is not merely an academic exercise; it is a critical step in ensuring that those in distress receive the appropriate level of care.
Main Facts: The Biological and Psychological Divide
At its core, sadness is an emotional reaction to a specific trigger. It is a fundamental part of the human experience, often brought on by loss, disappointment, or frustration. From a biological perspective, sadness serves a purpose: it signals to others that we may need support and allows the individual to pause and process significant life changes. Crucially, sadness is fluid. It comes in waves, often interspersed with moments of levity or the ability to experience pleasure.
Clinical depression, however, is a systemic malfunction of the brain’s regulatory systems. It involves more than just a "low mood." It is characterized by a persistent state of emotional, physical, and cognitive impairment that lasts for at least two weeks. Unlike sadness, depression often exists independently of external circumstances. A person can have a theoretically "perfect" life and still suffer from debilitating clinical depression due to imbalances in neurotransmitters like serotonin, norepinephrine, and dopamine, or due to structural changes in the brain’s hippocampus and amygdala.
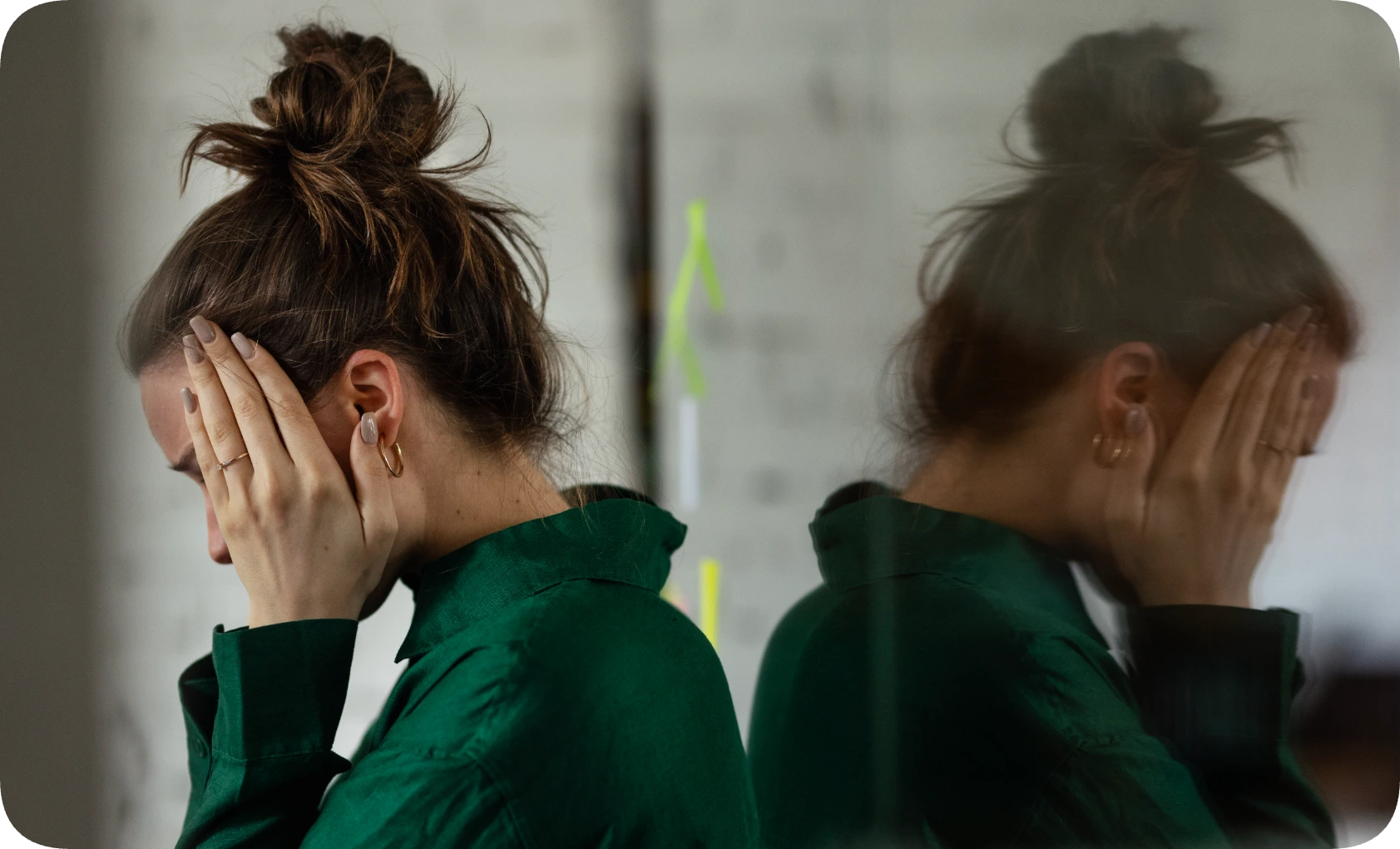
The most significant fact distinguishing the two is the concept of anhedonia—the inability to feel pleasure. While a sad person might still enjoy their favorite meal or a conversation with a friend, a person suffering from depression often finds that the things that once brought them joy now feel empty or burdensome.
Chronology: The Timeline of Emotional Persistence
To differentiate between a "rough patch" and a clinical diagnosis, clinicians look closely at the chronology of the symptoms. The timeline of emotional distress provides essential clues for diagnosis.
The Lifecycle of Sadness
Sadness typically follows a clear trajectory. Following a triggering event—such as a breakup, the loss of a job, or the death of a loved one—the emotion is intense. However, as days and weeks pass, the intensity of the sadness naturally fluctuates. The individual begins to integrate the experience into their life story. While the "weight" of the loss may remain, the individual’s ability to function and experience other emotions gradually returns.
The Stagnation of Depression
In contrast, depression is marked by its stubborn persistence. The American Psychiatric Association (APA) notes that for a diagnosis of MDD, symptoms must be present "most of the day, nearly every day" for a minimum of two weeks. For many, this timeline extends into months or even years.
There is no "upward curve" in untreated depression. Instead, the condition often creates a feedback loop: the lack of energy leads to social withdrawal, which increases feelings of isolation and worthlessness, further deepening the depressive state. This chronology of stagnation is a primary indicator that the brain’s natural emotional recovery mechanisms have been overwhelmed.
Supporting Data: A Multi-Dimensional Symptom Analysis
The distinction between sadness and depression becomes clearer when examining the data across four key dimensions: emotional, physical, cognitive, and functional.
1. Emotional and Mood Indicators
In cases of sadness, the primary emotion is grief or disappointment. In depression, the emotional palette is often described as "numb" or "hollow."
- Irritability: Data suggests that in men and adolescents, depression often manifests not as sadness, but as persistent anger or agitation.
- Guilt: While a sad person may regret a specific action, a depressed person often feels a generalized, "excessive or inappropriate" sense of guilt and worthlessness that is disconnected from reality.
2. Physical and Somatic Symptoms
Clinical depression is as much a physical illness as a mental one. Supporting data from clinical trials shows that depression frequently involves:

- Sleep Disturbances: Insomnia (difficulty falling or staying asleep) or hypersomnia (sleeping 10+ hours a day) are reported in over 80% of depressed patients.
- Appetite Changes: Significant weight loss or gain (a change of more than 5% of body weight in a month) is a diagnostic marker.
- Psychomotor Retardation: This refers to the visible slowing of physical movement, speech, and thought processes, making even simple tasks like showering feel like an Olympic feat.
3. Cognitive Distortions
The way a person processes information changes under the weight of depression.
- Executive Function: Depressed individuals struggle with concentration and decision-making. Simple choices, such as what to eat for lunch, can become paralyzing.
- Negative Filtering: The "depressive realism" or negative bias causes the brain to ignore positive stimuli and hyper-focus on perceived failures or threats.
4. Functional Impairment
This is perhaps the most quantifiable data point. Sadness may make work difficult, but depression often makes it impossible. Functional impairment is measured by the inability to maintain social roles, hygiene, and professional responsibilities.
Official Responses: Clinical Standards and Global Perspectives
Leading health organizations have established rigorous frameworks to ensure that depression is treated with the same medical urgency as physical ailments.
The DSM-5-TR Criteria
The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, Text Revision (DSM-5-TR) provides the "gold standard" for diagnosis. To be diagnosed with Major Depressive Disorder, an individual must experience five or more of the following symptoms during the same two-week period, with at least one of the symptoms being either (1) depressed mood or (2) loss of interest or pleasure:

- Depressed mood most of the day.
- Markedly diminished interest in all, or almost all, activities.
- Significant weight loss or gain.
- Insomnia or hypersomnia.
- Psychomotor agitation or retardation.
- Fatigue or loss of energy.
- Feelings of worthlessness or excessive guilt.
- Diminished ability to think or concentrate.
- Recurrent thoughts of death or suicidal ideation.
The World Health Organization (WHO)
The WHO recognizes depression as a leading cause of disability worldwide, affecting an estimated 280 million people. Their official response emphasizes that depression is not a sign of "weakness" but a result of a complex interaction of social, psychological, and biological factors. They advocate for a multi-faceted treatment approach that includes psychosocial support and, where appropriate, pharmacological intervention.
Crisis Intervention Standards
A critical component of the official response to mental health is the implementation of crisis resources. The 988 Suicide & Crisis Lifeline in the United States serves as a primary intervention tool. Official data indicates that immediate access to trained counselors significantly reduces the risk of self-harm during acute depressive episodes.
Implications: The Path to Recovery and Societal Impact
The implications of failing to distinguish between sadness and depression are profound. When depression is dismissed as "just sadness," individuals may blame themselves for their inability to "snap out of it," leading to a dangerous delay in seeking help.
The Risks of Untreated Depression
Untreated clinical depression can lead to chronic physical health issues, including heart disease and weakened immune systems. More critically, it increases the risk of suicide. When the brain is locked in a state of cognitive distortion, it can no longer see a future without pain, making professional intervention a literal matter of life and death.

The Efficacy of Treatment
The positive implication is that depression is one of the most treatable mental health conditions. Research into Cognitive Behavioral Therapy (CBT) shows that by identifying and restructuring negative thought patterns, patients can "rewire" their emotional responses. Furthermore, advancements in Interpersonal Therapy (IPT) and various classes of antidepressants (such as SSRIs and SNRIs) provide a range of options for those whose depression is rooted in biological or relational issues.
The Roadmap for the Individual
If an individual identifies with five or more items on the clinical checklist, the implications for their next steps are clear:
- Professional Assessment: Consult a primary care physician or a licensed therapist to rule out underlying physical issues (like thyroid dysfunction) and receive a formal diagnosis.
- Evidence-Based Treatment: Engage in a combination of therapy and, if recommended, medication.
- Support Systems: Reduce isolation by engaging with support groups or trusted family members.
- Self-Compassion: Recognize that the condition is a medical hurdle, not a character flaw.
Conclusion: Validating the Experience
Whether a person is experiencing the heavy, temporary clouds of sadness or the deep, persistent winter of depression, their pain is valid. However, identifying the nature of that pain is the only way to find the right map out of it. Sadness requires time, self-care, and the comfort of others; depression requires those things plus the clinical expertise of the medical community. By fostering a clearer understanding of these differences, we can ensure that no one has to navigate the spectrum of sorrow without the appropriate support.