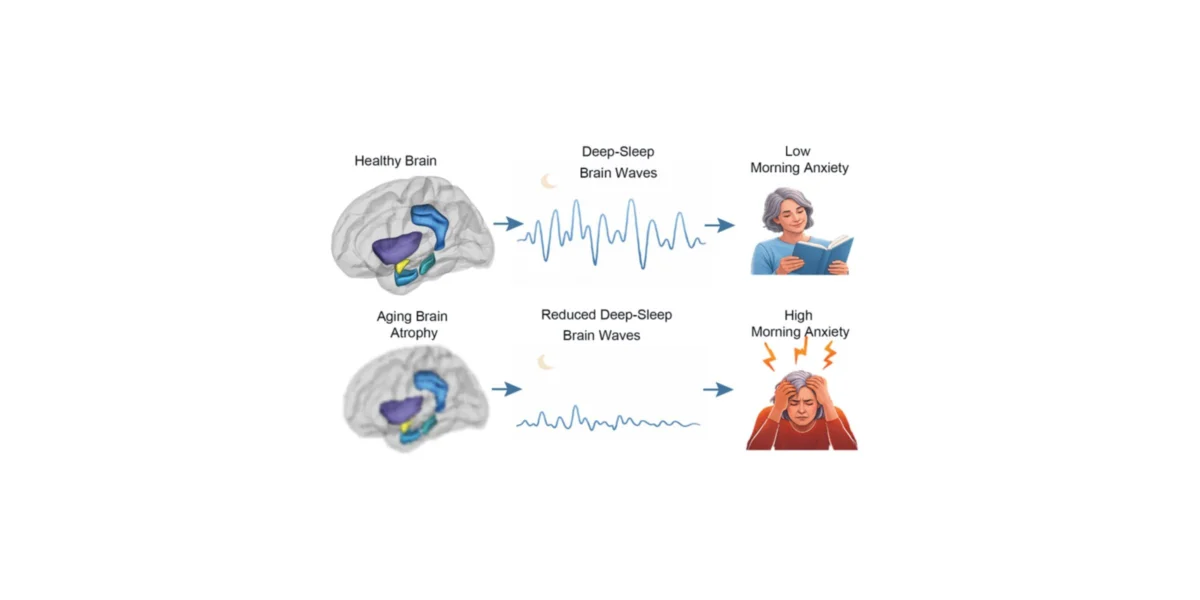
For many adults over the age of 60, the sunrise does not bring the freshness of a new day, but rather an immediate, lingering sense of apprehension. While anxiety is often categorized as a psychological issue, new, groundbreaking research suggests the root of the problem may be physiological—specifically, a failure of the brain’s "nightly recalibration" system.
A study conducted by researchers at the Center for BrainHealth at The University of Texas at Dallas has unveiled a critical link between the loss of deep, slow-wave sleep and the rising tide of anxiety in aging populations. Published in the journal Nature Communications Psychology, the findings suggest that the decline of these rolling brain oscillations is not merely a symptom of aging, but a modifiable target that could fundamentally change how we treat mental health in the elderly.
The Biological Mechanism: What is Slow-Wave Sleep?
To understand the study, one must first understand the architecture of sleep. During the deepest phase of non-REM sleep, the brain enters a state of synchronized activity characterized by large, rolling oscillations known as slow-wave activity (SWA).
For years, neuroscientists have understood that these waves are essential for physical restoration and memory consolidation. However, the UT Dallas team—led by Dr. Eti Ben Simon and Dr. Matthew Walker—has now demonstrated that these waves serve a secondary, equally vital purpose: emotional regulation.
"Deep sleep acts as a kind of nightly recalibration for the anxious brain," explains Dr. Ben Simon, associate director of the Sleep Innovation Laboratories at the Center for BrainHealth. "When that recalibration is impaired, anxiety doesn’t fully resolve overnight. The brain enters the next day lacking the necessary neurobiological buffer to handle the stressors of life."
A Chronology of the Research: From Data to Discovery
The research team undertook an extensive multi-year study to map the relationship between brain structure, sleep quality, and emotional state. The process involved 61 cognitively healthy older adults, with an average age of 74.6 years.
The Initial Assessment
The study began with a rigorous baseline assessment. Each participant underwent polysomnography—a comprehensive recording of biophysiological changes that occur during sleep—in a specialized laboratory environment. Researchers tracked the frequency and intensity of slow-wave activity throughout the night. Concurrently, participants provided self-reported data regarding their anxiety levels both before going to sleep and immediately upon waking.
The Structural Mapping
To determine if physical brain changes were driving these sleep deficits, the team utilized high-resolution MRI scans. They specifically looked for atrophy in the amygdala, insula, and cingulate cortex—the "emotional control centers" of the brain. The results were striking: participants who showed greater shrinkage in these regions produced significantly fewer slow waves during their sleep sessions.
The Four-Year Longitudinal Follow-Up
To move beyond a static snapshot, the researchers returned to a subset of 24 participants four years later. The longitudinal data provided a sobering look at the aging process. Over those four years, the group showed an average 20% decline in slow-wave activity. Crucially, the increase in their self-reported anxiety levels tracked almost perfectly with that decline, confirming that as the brain’s ability to generate deep sleep wanes, emotional resilience follows suit.
Supporting Data: Disentangling Age from Biology
One of the most profound revelations of the study is that chronological age is not the sole arbiter of emotional health. While the cohort was comprised of older adults, there was significant individual variation in how they slept and how they felt.
The study employed a mediation analysis to clarify the causal chain. It revealed that while brain atrophy is associated with lower anxiety, it is not the direct cause of the anxiety itself. Instead, the atrophy reduces the brain’s "power"—its structural capacity to generate deep, slow-wave sleep. It is the lack of that deep sleep that subsequently manifests as anxiety.
As Dr. Matthew Walker, senior author and director of the Sleep Innovation Laboratories, aptly puts it: "The atrophy is upstream—it’s the power cut, not the darkness itself."
Furthermore, the team found that not all sleep is created equal. While slow-wave activity was a perfect predictor of next-day anxiety, REM sleep did not show the same relationship. This specificity suggests that the therapeutic target for late-life anxiety is not just "better sleep" in a general sense, but the preservation and enhancement of the slow-wave deep sleep phase.
Official Responses and Clinical Implications
The implications for geriatric medicine are significant. Anxiety disorders currently represent the most prevalent mental health challenge for those over 60, yet they are frequently overshadowed by the clinical focus on dementia, Alzheimer’s, and depression.
"The stakes here are real," Dr. Walker notes. "As a society, our brainspans are not keeping up with our extended lifespans, but research continues to reveal new avenues that we can influence to proactively improve and optimize our brain health—including sleep."
The team proposes two distinct, complementary pathways for why this occurs:
- Autonomic Shift: Slow-wave sleep naturally encourages a shift from sympathetic arousal (the "fight or flight" mode) to parasympathetic recovery. Without this shift, the nervous system remains in a state of high alert.
- Locus Coeruleus Deterioration: The researchers point to the potential degradation of the locus coeruleus—a brainstem structure that produces noradrenaline. This structure begins to degrade around the same time that slow-wave sleep starts to decline, suggesting a shared biological vulnerability.
A New Frontier: Modifiable Targets for Intervention
Perhaps the most optimistic takeaway from the study is the concept of "modifiability." Unlike structural brain atrophy, which is currently difficult to reverse, sleep architecture is a dynamic process that can be influenced.
The researchers are already moving into the next phase of their work: active intervention. They are currently designing studies to test the efficacy of acoustic stimulation. By delivering precisely timed, gentle audio cues during the NREM sleep phase, the team hopes to artificially boost the brain’s generation of slow waves.
If successful, this could provide a non-pharmacological pathway to reducing anxiety in older adults, potentially improving their overall quality of life and autonomy. Beyond anxiety, the team is also investigating whether these interventions could serve as a prophylactic measure against the progression from normal aging to mild cognitive impairment.
The Societal Perspective
In an aging world where life expectancy has increased but the quality of "brainspan" has not, this research offers a roadmap for intervention. By shifting the focus from the irreversible (structural atrophy) to the modifiable (sleep quality), medical professionals may be able to offer older adults a tangible, effective way to manage their emotional well-being.
The study confirms that the bridge between the physical aging of the brain and the psychological experience of anxiety is built on the foundation of sleep. By reinforcing that bridge through better sleep hygiene and emerging technologies, we may be able to ensure that the later years of life are characterized not by apprehension, but by the calm, restored clarity that a good night’s sleep provides.
Key takeaways from the research:
- Slow-Wave Significance: Declining slow-wave activity is a primary driver of increased next-day anxiety in older adults.
- Brain Structure vs. Function: While structural brain atrophy (in the amygdala and insula) correlates with anxiety, it is the consequent loss of deep sleep that acts as the direct catalyst for emotional instability.
- Age is not a Predictor: Chronological age is less important than the individual’s current capacity to generate deep sleep; some older adults maintain strong slow-wave activity and, by extension, better emotional regulation.
- A New Therapeutic Target: Because sleep is a modifiable behavior, it offers a more immediate and effective intervention point than trying to reverse structural brain changes.
- Future Interventions: Researchers are now exploring acoustic stimulation to boost slow-wave sleep, potentially providing a non-drug treatment for late-life anxiety.