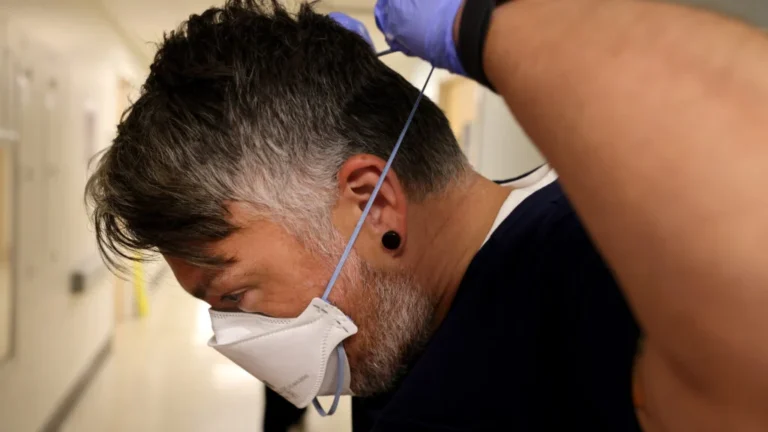
For patients undergoing hemodialysis, the central venous catheter is a literal lifeline. However, it is also a source of significant psychological burden, often acting as a barrier to the most basic of human rituals: the daily shower. A groundbreaking quality-improvement initiative recently presented at the National Kidney Foundation (NKF) Spring Clinical Meeting suggests that this barrier can be safely removed, restoring a sense of normalcy and dignity to patients without compromising their medical safety.
The initiative, spearheaded by researchers at Intermountain Health in Salt Lake City, Utah, demonstrates that a structured, education-heavy showering protocol can successfully allow hemodialysis patients to shower with their catheters in place. By shifting from a culture of blanket prohibition to one of educated empowerment, the program achieved high patient satisfaction scores while maintaining a zero-percent increase in central line-associated bloodstream infections (CLABSIs).
The Weight of Restriction: The "Straw That Breaks the Camel’s Back"
To understand the significance of this project, one must first understand the lifestyle of a hemodialysis patient. Beyond the life-sustaining treatment itself, these patients navigate a complex web of rigid dietary restrictions, demanding medication schedules, and the constant physical reminder of their illness via the catheter.
"Hemodialysis patients are typically told not to shower if they have a central venous catheter because of the infection risk, but from the patient perspective, it comes at a real cost," explained Carri Ekberg, MS, RN, the project lead at Intermountain Health.
For many, the directive to avoid showering is not merely a medical inconvenience; it is an emotional blow. "In addition to lifestyle changes and multiple dietary restrictions, they are dealing with a lot of psychological stress and change—and now we tell them that they can’t shower," Ekberg noted. "A lot of times, this is the straw that breaks the camel’s back."
The patient feedback gathered during the study revealed a profound sense of loss. Patients consistently reported feelings of frustration and the erosion of their self-image. For those living with chronic kidney disease, the act of showering is not just about hygiene; it is a fundamental pillar of personal dignity, independence, and psychological well-being.
Chronology of the Initiative: From Observation to Implementation
The project was born out of a stark realization: there was a massive disconnect between the clinical advice being given to patients and the reality of their daily lives.
Pre-Initiative Realities
Before the implementation of the new protocol, data collected from the four participating Utah dialysis centers revealed that medical advice was failing to translate into safe behavior. While 75% of patients had been strictly instructed to avoid showering, 58% admitted they were showering anyway.
Even more alarming was the lack of safety measures utilized by these patients. Of those who showered against medical advice, 16% took no protective measures at all. Those who did attempt to protect their catheter site often relied on dangerous "makeshift" solutions, such as wrapping the area in towels or plastic grocery bags—methods that offered little to no protection against moisture, which is the primary vector for infection.
The Intervention Strategy
Recognizing that patients were going to shower regardless of medical warnings, the Intermountain Health team chose to mitigate risk through education rather than prohibition. The chronology of the project followed these distinct phases:
- Protocol Development: Nephrologists and nursing staff collaborated to establish a standardized safety protocol.
- Educational Integration: The team moved away from passive pamphlets. They developed bilingual written instructions and short, easy-to-understand instructional videos.
- One-on-One Engagement: Two dedicated nurses conducted private training sessions, sitting with patients to watch the videos, answering questions, and demonstrating the application of professional-grade barrier products.
- Resource Provision: The centers began providing patients with a choice of high-quality protective barriers, such as Glad Press’n Seal or medical-grade "Shower Shields." The cost was absorbed by the centers, with professional shields costing roughly $1 per unit.
- Monitoring and Evaluation: From July to December 2025, the team tracked CLABSI rates and patient adherence, comparing these metrics against the same timeframe in 2024.
Supporting Data: Safety and Satisfaction
The initiative’s success was measured not only by the lack of infection but by the shift in patient autonomy.
Clinical Safety Outcomes
The primary clinical concern for any dialysis program is the incidence of CLABSIs. These infections are notoriously dangerous and financially burdensome, with a single event estimated to cost healthcare systems approximately $60,000. During the six-month trial period, the intervention group saw zero increase in infection rates, proving that with proper education and the right materials, the risk associated with showering can be effectively managed.
Patient Empowerment Metrics
The qualitative and quantitative data regarding patient response was overwhelmingly positive:
- 92% of patients reported feeling confident in their ability to keep their dressing dry.
- 86% of patients could correctly identify the steps to take if their dressing became wet.
- 89% of patients explicitly stated that the new protocol significantly increased their sense of safety while showering.
Monthly follow-ups indicated high levels of long-term adherence. Only a small percentage of patients discontinued the protocol, and in those cases, the reasons were medical or related to skin sensitivity rather than a failure of the education process.
Official Responses and Clinical Implications
At the National Kidney Foundation Spring Clinical Meeting, the presentation sparked a conversation about the "humanization" of dialysis care.
"Education wasn’t rushed or passive," Ekberg emphasized during her presentation. "Nurses reviewed the materials with the patients, sat down and watched the videos with them, answered their questions, and made sure that the patients knew what to do and that they understood what to do if something went wrong."
The clinical community has long struggled with the balance between "defensive medicine"—where the goal is to avoid all risk by banning activities—and "patient-centered care," which accounts for the mental health and quality of life of the individual. This study suggests that the two are not mutually exclusive.
A Call for Broader Adoption
The implications of this initiative are significant. By recognizing patients as "capable partners" in their own care, healthcare providers can foster greater trust and compliance. If a patient feels heard and supported in their desire for normalcy, they are more likely to communicate honestly with their care team about other health challenges.
Ekberg is now calling for a transition from this pilot phase to larger, more diverse clinical trials. "The project wasn’t just about showering," she concluded. "It was about dignity, trust, and recognizing patients are capable partners in their care. It was about humanizing dialysis care."
Conclusion: The Path Forward
The emotional testimonies from participants highlight the true success of the program. For many, the ability to wash their hair independently or feel truly clean was a transformative experience. Some patients even reported "happy tears," a poignant reminder of the small, everyday freedoms that chronic illness often strips away.
As the medical community looks to the future, the Intermountain Health protocol serves as a blueprint for how healthcare systems can improve patient outcomes by looking beyond the clinical chart. By addressing the psychological and emotional barriers that patients face, providers can ensure that their care is not only effective at treating the kidneys but also at supporting the person behind the diagnosis.
Future studies will look to expand this protocol to larger populations, refine the educational methods, and test the efficacy of various barrier products. However, the lesson remains clear: when you empower patients with the right tools and information, they can safely reclaim their lives, one shower at a time.