A recent, alarming outbreak of the Andes hantavirus strain aboard the international cruise ship MV Hondius has sent ripples through the global public health community. While the incident may appear isolated to a single vessel, experts warn that it represents a far more significant systemic risk: the potential for "silent" human-to-human transmission of a pathogen previously thought to be largely confined to rodent-to-human spillover events. This incident has underscored critical gaps in our understanding of how viruses circulate in wild populations and how modern travel networks can turn a localized zoonotic encounter into an international health crisis.
RT’s Three Key Takeaways
- Shift in Transmission Paradigms: Unlike most hantaviruses, the Andes strain is capable of human-to-human transmission, complicating containment efforts in high-density environments like cruise ships.
- The "Reactive" Research Gap: Current public health frameworks are primarily reactive, focusing on containment after a spillover occurs rather than proactively monitoring viral circulation in wildlife reservoirs.
- Clinical Severity and Mortality: With mortality rates reaching up to 60% in some regions, the Andes hantavirus poses a far more lethal threat than many respiratory viruses, necessitating advanced, aggressive supportive care strategies in the absence of a vaccine.
Main Facts: The Andes Hantavirus Threat
The MV Hondius incident serves as a stark case study in the unpredictability of zoonotic pathogens. According to researchers at Virginia Tech, the event highlights a fundamental misunderstanding of the ecological plasticity inherent in certain hantavirus strains.
Historically, the medical community viewed hantaviruses as pathogens that maintained a strict relationship with specific rodent hosts. However, the Andes strain demonstrates a dangerous versatility. It does not merely jump from rodent to human; it possesses the biological capacity to transmit between humans, a feature that transforms a simple environmental encounter into a potential pandemic vector. The implications for the cruise industry—and indeed any sector reliant on global human mobility—are profound. When a virus can move silently through an asymptomatic or mildly symptomatic population, the window for effective quarantine and intervention narrows significantly.
Chronology: From Wildlife Reservoir to Maritime Crisis
The path from a remote wilderness to a cruise ship deck is complex, yet the MV Hondius outbreak provides a window into the chain of events:
- Pre-Outbreak Phase: Viral circulation persists in wild rodent populations, often driven by environmental stressors or changes in habitat. During this period, the virus remains largely undetected by public health surveillance systems.
- The Spillover Event: A human encounter—likely involving contaminated dust or excreta—leads to the initial infection. In the case of the Andes strain, this individual becomes a carrier capable of infecting others.
- Maritime Transmission: Once aboard the cruise ship, the confined environment and the shared ventilation systems of modern vessels create a perfect incubator for respiratory transmission.
- Detection and Response: Symptoms among passengers and crew lead to medical intervention. However, because hantavirus is not always the first consideration for respiratory illness in travelers, the initial stages of the outbreak likely saw a period of undiagnosed spread, further complicating contact tracing.
Supporting Data: Understanding the Biological Threat
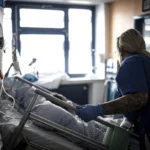
The clinical reality of an Andes hantavirus infection is sobering. For healthcare professionals, the primary concern is the development of Hantavirus Pulmonary Syndrome (HPS).
Unlike other respiratory illnesses that destroy lung tissue, HPS triggers an extreme inflammatory response. The immune system, in its attempt to neutralize the virus, goes into overdrive. This results in a massive "cytokine storm," causing the lungs to fill rapidly with fluid. The physiological stress is immense, and in the absence of a vaccine, the only clinical recourse is intensive, supportive care—often requiring extracorporeal membrane oxygenation (ECMO) or advanced mechanical ventilation.
The statistics are equally alarming. While COVID-19 captured the world’s attention for its transmissibility, the Andes hantavirus demands attention for its lethality. In parts of southern Chile, mortality rates among those hospitalized have hovered near 60%. This makes the virus a potent, albeit less frequent, threat that requires a significantly higher level of hospital preparedness than current standards for seasonal influenza or common respiratory infections.
Official Responses and Epidemiological Insights
Luis Escobar, an associate professor in the College of Natural Resources and Environment at Virginia Tech, has been at the forefront of analyzing this event. In a recent news release, Escobar emphasized that the scientific community’s current approach is fundamentally flawed.
"Most of our research on zoonotic viruses remains reactive," Escobar noted. "We study them after they spill over into humans instead of understanding how they circulate in wildlife beforehand."
This sentiment is echoed by broader warnings from the US National Academy of Medicine, which has consistently argued that the global community is ill-prepared for the next pandemic. The MV Hondius outbreak is being used as evidence to push for a more proactive surveillance strategy. This would involve "genomic surveillance" of rodent populations in high-risk areas, allowing scientists to identify emerging strains before they reach human centers of activity.
Furthermore, health officials are grappling with the "silent spread" problem. Because many hantavirus cases present with mild, flu-like symptoms, the true number of infections is likely significantly higher than what is reported in hospital databases. This "iceberg effect" makes it nearly impossible for authorities to accurately calculate the risk or implement effective containment strategies without mass, random testing—a logistical nightmare for international travel.
Implications for Global Public Health
The MV Hondius incident is more than a cruise ship story; it is a warning about the intersection of human behavior and viral evolution.
1. The Mobility Factor
Human mobility is the greatest driver of modern outbreaks. As the world becomes increasingly interconnected, pathogens that were once geographically isolated can cross oceans in hours. Cruise ships, which act as "mini-cities," are particularly vulnerable to respiratory outbreaks. The reliance on centralized air conditioning and the high-density interactions of passengers create an environment where viruses can thrive if they are not detected early.
2. Environmental Drivers
Research suggests that human-driven environmental changes—such as deforestation, urbanization, and climate shifts—are forcing wild rodents into closer contact with human settlements. This shifts the ecological balance, increasing the frequency of spillover events. Escobar emphasizes that we must stop blaming the virus and start analyzing the human behaviors that facilitate these interactions.
3. The Need for Proactive Surveillance
The transition from reactive to proactive healthcare is the single most important lesson from this outbreak. Public health budgets are currently weighted toward treatment, but the Andes hantavirus highlights that prevention at the source is the only way to avoid catastrophic outcomes. This involves international collaboration to track viral movement in wildlife, coupled with better diagnostic tools that can be deployed quickly in travel hubs like airports and cruise terminals.
4. Re-evaluating Respiratory Protocols
For the clinical community, the Andes hantavirus mandates a re-evaluation of respiratory protocols. When a patient presents with severe pulmonary symptoms after travel, clinicians must look beyond the standard panel of respiratory viruses. Including hantavirus in the differential diagnosis, especially if the travel history includes areas where the Andes strain is endemic, could save lives through earlier initiation of aggressive supportive care.
Conclusion: A Call to Action
The outbreak of the Andes hantavirus aboard the MV Hondius has stripped away any lingering complacency regarding the predictability of zoonotic diseases. We are living in an era where the barriers between wildlife and human society are thinner than ever.
As we look toward the future, the integration of ecological research with public health policy is non-negotiable. We cannot afford to wait for the next spillover to understand how these pathogens behave. By investing in proactive monitoring, improving diagnostic speed, and fostering international coordination, the global health community may yet gain the upper hand. However, the MV Hondius remains a sobering reminder: the next pandemic may not come from a laboratory or a known viral strain, but from the silent, unchecked evolution of a pathogen hiding in plain sight within our own wild backyards.