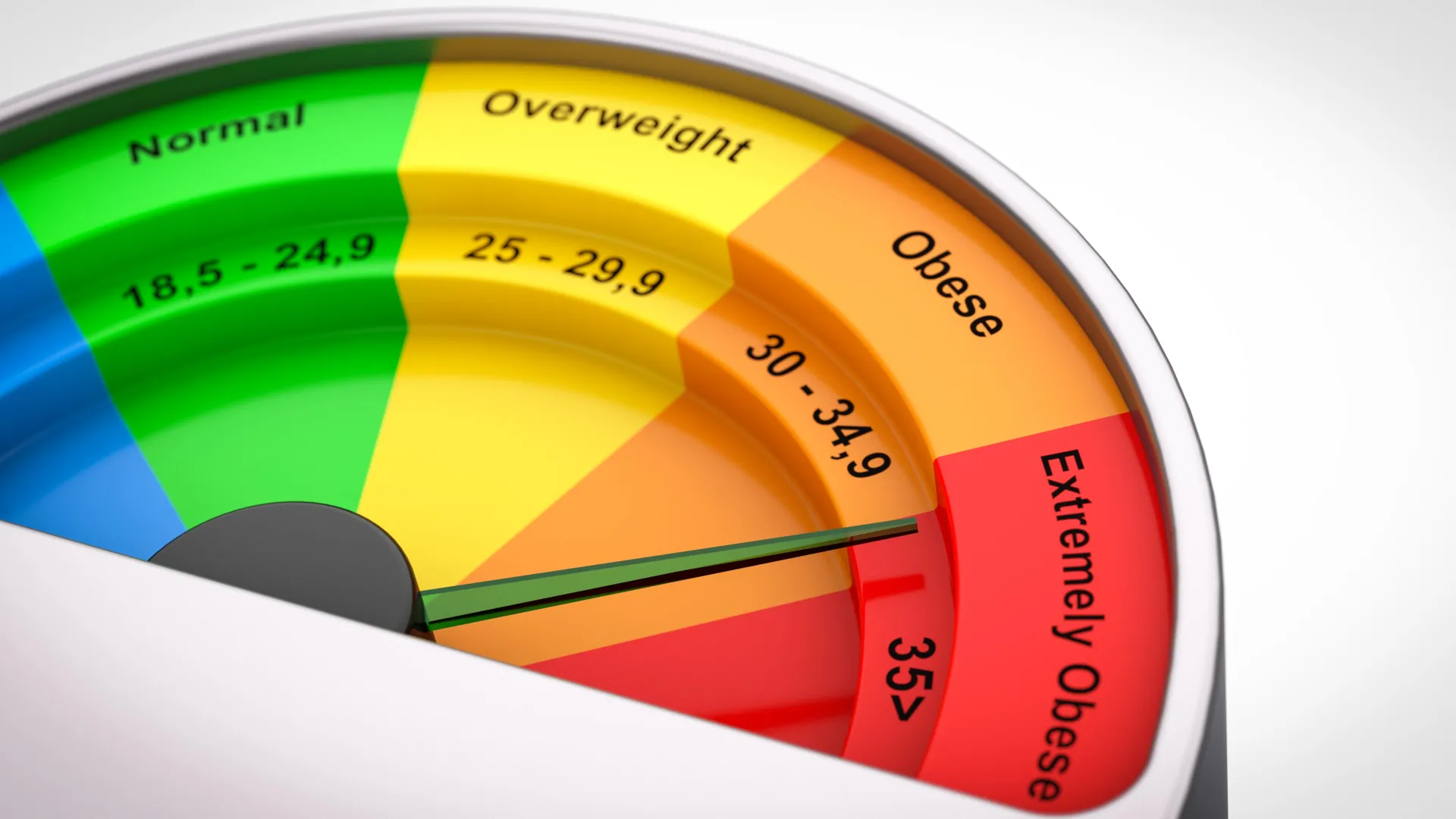
For over a century, the Body Mass Index (BMI)—a simple calculation derived from a person’s height and weight—has served as the cornerstone of clinical obesity diagnostics. It is the metric that insurance companies use to set premiums, that governments use to track public health trends, and that general practitioners use to initiate weight-loss conversations. However, a groundbreaking study set to be presented at the upcoming European Congress on Obesity (ECO 2026) in Istanbul suggests that this universal shorthand for health may be fundamentally flawed.
New research, published in the journal Nutrients, indicates that BMI frequently misclassifies millions of individuals, misrepresenting their actual physiological health by failing to distinguish between fat mass and muscle mass. As healthcare shifts toward more personalized, precision medicine, this study provides some of the most compelling evidence to date that our reliance on BMI may be an outdated practice in need of urgent reform.
The Flawed Gold Standard: Why BMI Is Losing Credibility
The fundamental limitation of the BMI system is its simplicity. It is a mathematical ratio—weight in kilograms divided by the square of height in meters—that assumes a one-size-fits-all correlation between mass and body fat. Critically, BMI does not account for body composition. It cannot differentiate between a pound of dense muscle tissue and a pound of adipose tissue (body fat), nor does it consider where that fat is stored.
Professor Marwan El Ghoch, of the Department of Biomedical, Metabolic and Neural Sciences at the University of Modena and Reggio Emilia, notes that this lack of nuance creates a "blind spot" in clinical practice. "BMI is a crude instrument," says El Ghoch. "Because it does not directly measure adiposity or fat distribution, it struggles to provide an accurate reflection of metabolic health. Despite this, it remains the default for clinical and non-clinical settings alike, from GPs’ offices to large-scale public health policy."
The implications of this inaccuracy are significant. When patients are incorrectly labeled as "obese," they may face unnecessary psychological stress, stigmatization, or the prescription of weight-loss interventions that are inappropriate for their specific body composition. Conversely, those with high body fat but "normal" BMI—sometimes referred to as "skinny fat"—may be overlooked by screening tools, potentially missing early warnings for metabolic conditions like insulin resistance or cardiovascular disease.
A Chronology of the Research
The study, a collaborative effort between the University of Verona and Beirut University, was designed to put the BMI system to the test against the "gold standard" of body composition analysis: Dual-energy X-ray absorptiometry (DXA).
The Methodology
The research team recruited a cohort of 1,351 adults, aged 18 to 98, from the Department of Neurosciences, Biomedicine and Movement Sciences at the University of Verona. To ensure a focused analysis, the participants were exclusively White Caucasian, a decision made to control for known ethnic variations in body fat distribution that can further complicate BMI accuracy.
The study followed a clear investigative progression:
- Baseline Assessment: Participants were initially classified using the World Health Organization (WHO) standard BMI categories: Underweight (<18.5), Normal weight (18.5–25), Overweight (25–30), and Obese (>30).
- The Gold Standard Test: Researchers performed DXA scans on all 1,351 participants. DXA is a sophisticated imaging technology that measures bone density, lean muscle mass, and fat percentage with high precision.
- Comparative Analysis: The team compared the BMI-derived labels against the DXA-derived body fat percentage (BF%) classifications, which are adjusted for age and gender.
Key Data Points
The initial BMI classification of the group yielded the following:
- Underweight: 1.4% (19 individuals)
- Normal Weight: 58.3% (787 individuals)
- Overweight: 26.2% (354 individuals)
- Obese: 14.1% (191 individuals)
This initial snapshot suggested a 41% combined rate of overweight and obesity, aligning with existing epidemiological data for the Veneto region of Italy. However, once the DXA results were integrated into the assessment, the landscape of the data shifted dramatically.
Significant Misclassification: The Data Revealed
The most startling aspect of the study was not just the degree of error, but the specific categories where the errors occurred.
Overweight and Obesity Discrepancies
Among those labeled "obese" by BMI, a full 34% were found to be in the "overweight" category when measured by body fat percentage. Even more concerning was the misclassification of the "overweight" group: 53% of individuals labeled as overweight by BMI did not meet the DXA criteria for that category. Of that 53%, approximately 75% were actually in the "normal" weight range, while the remaining 25% were categorized as obese.
The Underweight Paradox
Perhaps the most surprising finding occurred in the underweight category. Of the 19 individuals labeled as underweight by BMI, nearly 69% (13 people) were actually at a healthy, normal weight according to their body composition. This suggests that the current BMI cut-off for "underweight" may be too aggressive, potentially pathologizing individuals who simply possess a lean, healthy frame.
Normal Weight Agreement
The BMI system performed best at the center of the bell curve. Among those classified as "normal weight" by BMI, 78% were confirmed as such by DXA. However, even in this category, 22% were misclassified, with 11.4% actually falling into the overweight category—a group that might be "passing" as healthy while carrying higher-than-recommended body fat levels.
Overall, while the total prevalence of overweight and obesity was relatively similar between the two methods (41% for BMI vs. 37% for DXA), the individuals caught in the crosshairs were different. As Professor Chiara Milanese of the University of Verona points out, "We are talking about different people. The individuals identified by DXA are not all the same as those from BMI classification."
Official Responses and Expert Interpretation
The research team argues that these findings are not merely academic—they represent a call to action for the medical community. Professor El Ghoch emphasizes the danger of relying on a system that systematically overestimates prevalence rates for weight categories.
"Our findings suggest that a large proportion of the Italian general population is misclassified," says El Ghoch. "When you rely on traditional WHO BMI classification, you are inherently biasing your data. By comparing this to the gold-standard DXA, we can see clearly that we are mismanaging, or at the very least mislabeling, a significant portion of the population."
The experts involved in the study do not necessarily advocate for the complete abandonment of BMI, but rather for a move toward a "multidimensional" assessment. They suggest that BMI should be viewed as a screening tool, not a diagnostic one. If a patient’s BMI indicates a potential health risk, the clinical pathway should trigger secondary, more precise measurements.
Implications for Public Health and Clinical Practice
What does this mean for the future of healthcare? If the findings from this study are representative of White Caucasian populations globally, the implications are profound:
1. Reforming Clinical Guidelines
Healthcare institutions may need to update their protocols to integrate body composition measurements. While DXA is expensive and time-consuming, researchers suggest there are simpler, more accurate alternatives, such as:
- Waist-to-Height Ratio: A better predictor of visceral fat and metabolic risk.
- Skinfold Measurements: A low-cost, portable way to assess body fat.
- Bioelectrical Impedance Analysis (BIA): An accessible, non-invasive method for tracking body composition changes over time.
2. Policy and Insurance
If BMI is used to determine insurance premiums or public health subsidies, the misclassification identified in this study suggests that many individuals are being unfairly penalized. If a person is labeled "obese" due to muscle mass rather than excess body fat, they may be paying higher premiums for a risk profile they do not actually possess.
3. Addressing Ethnic Variation
The researchers were careful to note that their study focused on White Caucasians. They acknowledge that body composition varies significantly across ethnic groups. For instance, South Asian populations may experience metabolic complications at lower BMI levels than those of European descent. Future research must replicate these findings across diverse demographics to ensure that global health guidelines are equitable and accurate.
Conclusion: A New Frontier in Health Assessment
The study to be presented at ECO 2026 serves as a wake-up call. We are living in an era of wearable technology and advanced metabolic testing, yet we continue to use a height-to-weight calculation invented in the 19th century to define health.
While the convenience of BMI is undeniable, the accuracy of medical diagnosis must take precedence. By transitioning toward tools that measure body composition rather than just total mass, clinicians can provide more accurate health assessments, reduce the stigma associated with weight, and move closer to a truly personalized model of patient care. As the medical community converges in Istanbul this May, the conversation surrounding the retirement of the "BMI-only" model is set to take center stage, marking a potential turning point in how we define, measure, and treat body weight in the 21st century.