By Sree Roy
For years, the sleep medicine community has been engaged in a high-stakes campaign to educate CPAP (Continuous Positive Airway Pressure) users about the risks associated with automated cleaning devices. These ozone- and ultraviolet-based gadgets, once marketed as "set-it-and-forget-it" solutions for sanitizing sleep apnea equipment, have faced intense scrutiny from the US Food and Drug Administration (FDA) and major medical device manufacturers.
New survey data from Sleep Review suggest that this messaging has been remarkably successful. However, as the industry celebrates this victory in consumer behavior, a new, equally pressing concern has emerged: while patients have largely abandoned these controversial devices, they are struggling to maintain the manual, labor-intensive cleaning regimens required to keep their equipment safe and functional.

Main Facts: A Shift in Cleaning Paradigms
The primary takeaway from the latest survey data is that the message regarding automated cleaners has reached the target audience. An overwhelming 86% of respondents reported that they have "never" used an automated CPAP cleaning device. The remaining 14% represent users who have experimented with them in the past but have since ceased usage. Significantly, 0% of respondents reported currently using such a device.
This abandonment is driven by a combination of heightened consumer awareness and aggressive policy shifts by manufacturers. The FDA has been clear in its public health communications: these add-on devices do not replace the manufacturer’s recommended cleaning protocols, which prioritize the use of mild soap and water. Furthermore, many manufacturers have explicitly updated their warranty language to exclude damage caused by ozone or UV light exposure—a financial risk that is clearly resonating with the patient population.
Chronology of a Regulatory Pushback
The path to this current state of affairs was marked by mounting scientific concern and regulatory intervention.

2019–2020: The Rising Tide of Concern
As the popularity of "convenience-based" CPAP cleaners grew, so did reports of internal equipment degradation. Users began complaining of damaged seals, degraded silicone masks, and even the release of ozone gas into bedrooms. Clinical experts began warning that ozone could potentially cause respiratory irritation, particularly for those with underlying pulmonary conditions.
2021–2022: FDA Formalizes Warnings
The FDA issued a landmark consumer update, stating definitively that there is no clinical necessity for automated cleaning devices. The agency emphasized that the "cleaning" provided by these units was not equivalent to the mechanical removal of oils, skin cells, and bacteria that occurs through thorough hand-washing with soap and water.
2023–2024: Warranty Exclusions and Industry Alignment
Following the FDA’s guidance, major CPAP manufacturers—including ResMed and Philips—revised their user manuals and warranty terms. These updates explicitly warned that the use of ozone or UV cleaners would void the warranty. This proved to be a decisive "tipping point" for consumers, as the prospect of replacing a $500 to $1,000 machine out-of-pocket incentivized compliance with traditional methods.

Supporting Data: The "Mask-Only" Syndrome
While the industry has succeeded in driving patients away from potentially harmful automated cleaners, the Sleep Review survey highlights a critical gap in the "next step" of patient education: consistent, holistic equipment maintenance.
The Discrepancy in Hygiene
The data reveals a stark contrast between how users treat their masks versus how they treat the "infrastructure" of their CPAP setup—the tubing, the humidifier water chamber, and the air filters.
- Mask Hygiene: The majority of patients are doing well here. 57% of respondents reported washing their mask within the last 24 hours, and 29% within the last week. This aligns with the gold standard of daily mask cleaning to prevent facial breakouts and ensure a proper seal.
- Tubing and Humidifier Neglect: When the focus shifts to the tubing and humidifier, the numbers drop significantly. A large percentage of users report that these components go weeks or even months without a thorough deep clean.
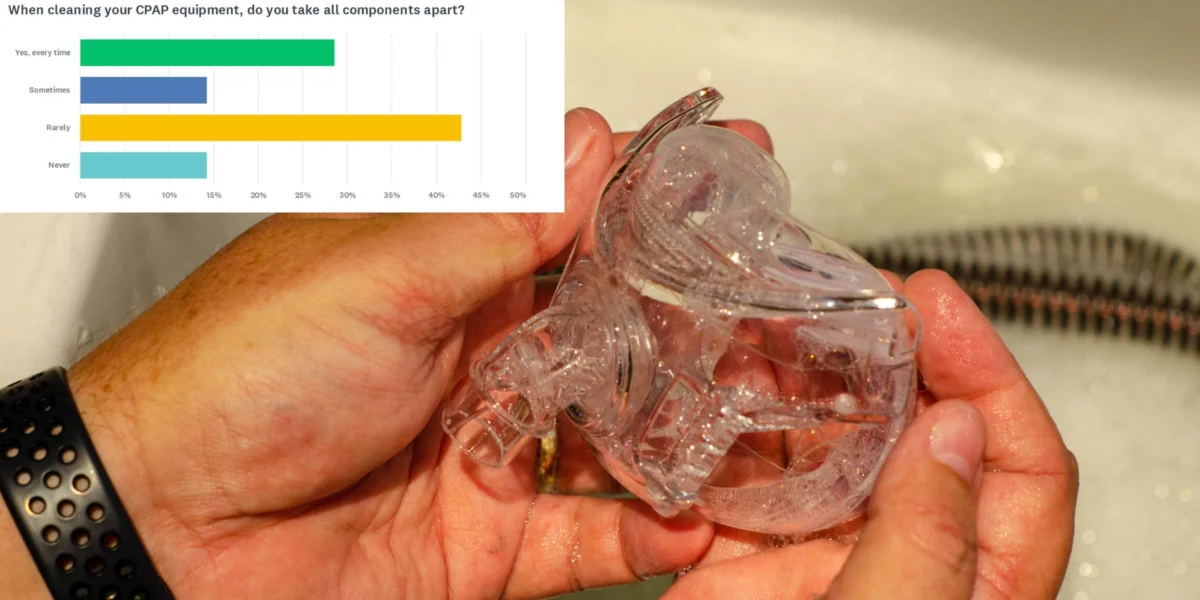
- The Disassembly Failure: Perhaps the most concerning finding is the lack of proper disassembly. Only 29% of respondents take their entire system apart "every time" they clean it. A staggering 43% report "rarely" taking the system apart, and 14% "never" do.
This means that a significant portion of the user base is performing "surface cleaning" on the mask while allowing biofilm and mineral buildup to accumulate in the harder-to-reach areas of the tubing and the humidifier tank.

Official Responses: What the Experts Say
The consensus among durable medical equipment (DME) providers and sleep specialists is that the "automated cleaner" era created a false sense of security. Patients became accustomed to a "hands-off" approach to hygiene. Transitioning back to manual maintenance requires more than just a list of instructions; it requires a change in daily habits.
"I was told by an employee from my CPAP supply company to not use any of the cleaning machines—that they weren’t good for the machine," one survey respondent noted. This indicates that the frontline of education—the DME providers—are playing a vital role. However, the data suggests that providers must now emphasize the how-to of manual cleaning as much as they emphasize the why-not of automated cleaners.
According to the FDA, the manual process should involve:

- Disassembling the mask, tubing, and water chamber completely.
- Soaking the components in warm water with a mild, fragrance-free detergent.
- Rinsing thoroughly to ensure no soap residue remains.
- Air-drying away from direct sunlight, ensuring all components are completely dry before reassembly to prevent mold growth.
Implications: The Path Forward for Sleep Health
The shift away from automated cleaners is a success story for patient safety, but the current state of manual hygiene is a "quiet" public health challenge. If CPAP equipment is not cleaned properly, users risk more than just equipment degradation; they risk exposure to bacterial and fungal pathogens that can be aerosolized during use.
Improving Patient Outcomes
For the sleep medicine community, the implications are clear:
- Standardized Education: DMEs must integrate a "hands-on" training component during the initial setup process. Providing a video tutorial or a physical demonstration of how to disconnect and reconnect the tubing and water chamber can increase compliance.
- Simplifying the Routine: Many patients fail to clean the system because they find the process cumbersome. Manufacturers could aid this by designing components that are easier to disassemble without specialized tools or excessive force.
- Addressing the Drying Gap: While 83% of users air-dry their equipment—which is the recommended method—the timing matters. If a user tries to reassemble the device before it is fully dry, they create a breeding ground for bacteria. Education needs to emphasize that "drying time" is a mandatory part of the cleaning cycle.
A Renewed Focus on Hygiene Literacy
The survey results serve as a wake-up call. We have successfully removed a "convenience" that was causing long-term harm, but we have yet to replace it with a sustainable, healthy, and effective manual routine for all patients.

As the industry looks ahead, the focus must shift from "what not to use" to "how to best maintain." By fostering a better understanding of why the entire system—not just the mask—requires regular, thorough attention, sleep professionals can ensure that CPAP users continue to reap the benefits of their therapy without compromising their health through poor hygiene.
Ultimately, the goal remains the same: ensuring that every patient using CPAP therapy can do so with the peace of mind that their equipment is as clean as it is effective. The data shows that the awareness is there; now, it is time to build the habits to match.