Featured Buzz – January 11, 2026
The landscape of respiratory medicine is undergoing a profound transformation. As diagnostic precision becomes increasingly critical in the face of rising chronic respiratory conditions and the global challenge of antibiotic resistance, researchers are turning to high-tech solutions. From leveraging artificial intelligence (AI) to interpret routine cardiac tests for lung disease to utilizing ultrasound for neonatal care and molecular biomarkers for infection control, recent breakthroughs are redefining the standard of care. This report examines three pivotal studies that highlight how technology is enabling earlier interventions and more judicious clinical decision-making.
1. ECGs as a Gateway to Early COPD Diagnosis
Chronic Obstructive Pulmonary Disease (COPD) remains one of the world’s leading causes of morbidity, yet it is notoriously underdiagnosed in its early stages. Often, patients do not seek medical attention until lung function has already significantly declined.
The Mount Sinai Breakthrough
Researchers from the Mount Sinai Health System have introduced a novel diagnostic paradigm: utilizing standard electrocardiograms (ECGs) to screen for COPD. While ECGs are the bedrock of cardiac screening, their potential to detect lung pathology has long been overlooked.
By analyzing a massive dataset comprising 208,231 ECGs from 18,225 COPD patients and over half a million control samples, the team trained a Convolutional Neural Network (CNN) to recognize patterns in heart electrical activity that correlate with COPD-related physiological changes, such as pulmonary hypertension or lung hyperinflation.
Clinical Implications
The research, published in eBioMedicine, suggests that while ECGs will not replace gold-standard spirometry, they serve as a highly pragmatic screening tool. Because ECGs are performed frequently in primary care, embedding this AI model into electronic health records (EHRs) could flag high-risk patients during routine visits. Early recognition allows for timely smoking cessation interventions, pulmonary rehabilitation, and targeted therapies—all of which are essential for slowing the progression of this debilitating disease.
2. Precision in the NICU: Lung Ultrasound and Extubation Success
For very low birth weight (VLBW) infants, the transition from mechanical ventilation to independent breathing is a high-stakes clinical event. Failed extubation is associated with increased mortality, prolonged hospitalization, and higher healthcare costs.
A New Predictive Metric
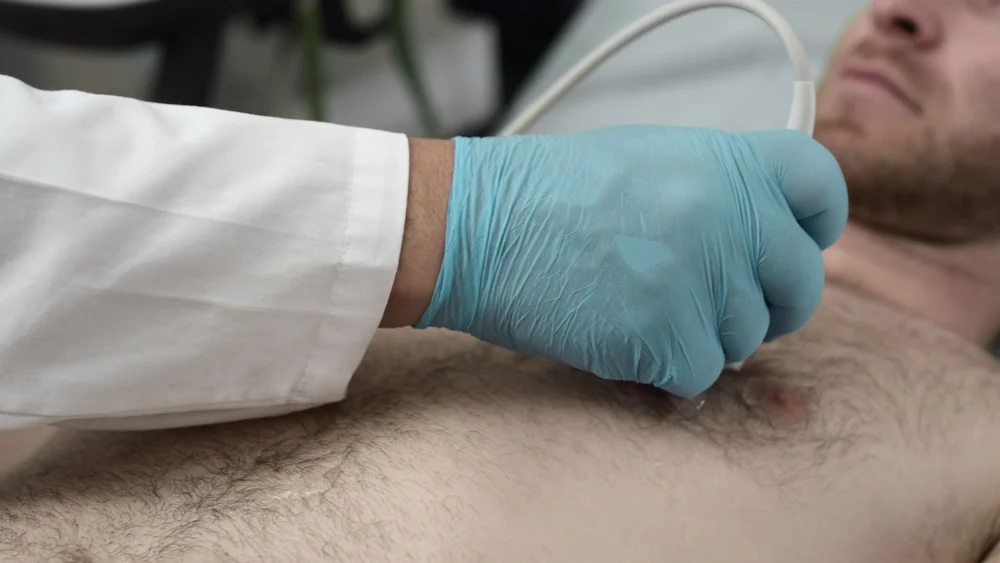
A study conducted by the University of Chicago, published in the Journal of Perinatology, sought to improve these outcomes using lung ultrasound (LUS). By monitoring 45 VLBW infants, the researchers demonstrated that a neonatal-adapted LUS score, calculated three to six hours prior to an extubation attempt, acts as a robust predictor of success.
The study compared 53 extubation attempts, defining failure as the need for reintubation within seven days. The findings provide a clear, actionable metric for neonatologists, allowing them to assess lung readiness with precision rather than relying solely on clinical observation or arterial blood gases.
Addressing Therapeutic Misconceptions
A significant takeaway from the study was the clarification of the role of corticosteroids in neonatal care. The researchers found that dexamethasone treatment, often used to facilitate weaning from ventilators, was not associated with improved LUS scores. This insight encourages clinicians to move away from potentially unnecessary pharmacological interventions in favor of objective, ultrasound-based weaning protocols.
3. Combating Antibiotic Overuse: The AI-Biomarker Synthesis
The "silent pandemic" of antibiotic resistance is fueled, in part, by the empirical prescription of antibiotics for lower respiratory tract infections (LRTIs) in the absence of definitive diagnostic data.
The UCSF Diagnostic Model
Researchers at the University of California, San Francisco (UCSF), have developed a sophisticated diagnostic strategy that integrates molecular biology with generative AI. Their model focuses on the gene FABP4, which is found in lung fluid and plays a role in tempering inflammation. In cases of bacterial infection, FABP4 expression drops significantly compared to healthy tissue.
The UCSF team combined this host biomarker data with a generative AI analysis of EHR data—including chest X-ray reports and clinical notes—to create a comprehensive diagnostic tool.
Accuracy and Clinical Impact
In an observational study of critically ill adults, the model achieved a 96% diagnostic accuracy rate, significantly outperforming human clinicians. The implications for stewardship are immense: the authors estimate that widespread adoption of this model could reduce inappropriate antibiotic use by over 80%. As the medical community struggles to preserve the efficacy of current antibiotics, tools that provide high-confidence diagnoses of LRTIs are of paramount importance. The team is currently moving toward validating the model for clinical deployment and expanding the technology’s application to the detection of sepsis.
Chronology of Technological Integration
The recent surge in these diagnostic tools follows a distinct developmental timeline:
- Early 2024: Initial development of generative AI models for clinical note analysis begins in academic medical centers.
- Late 2024: Research teams shift focus toward multimodal integration (combining biomarkers with EHR data).
- 2025: Large-scale validation studies (including the Mount Sinai ECG project and the UCSF LRTI study) are completed and submitted for peer review.
- January 2026: Publication of these findings highlights a paradigm shift toward "AI-augmented clinical intelligence."
Supporting Data and Comparative Analysis
| Study Area | Primary Technology | Key Metric | Success Rate/Impact |
|---|---|---|---|
| COPD | CNN-trained ECGs | ICD-code accuracy | High potential for early detection |
| NICU | Neonatal LUS Score | Reintubation rates | Excellent predictive value |
| LRTI | Generative AI + FABP4 | Diagnostic precision | 96% accuracy; 80% reduction in antibiotic waste |
Official Responses and Expert Consensus
Medical societies and academic institutions have reacted with cautious optimism to these developments. While the integration of AI into diagnostic workflows is seen as inevitable, experts emphasize the need for "human-in-the-loop" oversight.
"The goal is not to replace the clinician," stated one UCSF lead investigator, "but to provide the clinician with a higher level of data synthesis that is impossible for a human to perform in the minutes allotted during a critical care rounds."
The sentiment across all three research groups is clear: the future of medicine lies in the synthesis of high-resolution molecular data (like FABP4), real-time imaging (LUS), and large-scale pattern recognition (AI-ECG).
Implications for Future Healthcare
The implications of these three studies extend beyond their immediate applications:
- Reduced Healthcare Burden: By catching COPD early and preventing reintubation in VLBW infants, healthcare systems can reduce the length of hospital stays and the frequency of readmissions.
- Stewardship of Resources: The UCSF model represents a significant step forward in antimicrobial stewardship. Reducing inappropriate antibiotic use not only helps individual patients by avoiding side effects but also protects public health by curbing the development of multidrug-resistant organisms.
- Democratization of Diagnostics: With the availability of HIPAA-compliant interfaces like GPT-4, sophisticated diagnostic tools that were previously limited to tertiary research centers are becoming accessible to general practitioners and community hospitals.
A New Era of Diagnostic Precision
As we move further into 2026, the integration of these technologies marks the transition from reactive to proactive medicine. The ability to "see" disease before it manifests clinically, or to distinguish between inflammatory and infectious states with molecular precision, represents a leap forward that will define the next decade of patient care.
While clinical validation remains the essential final hurdle, the evidence provided by these institutions—Mount Sinai, the University of Chicago, and UCSF—demonstrates that the tools to transform respiratory health are already at our fingertips. As these models move from the pages of eBioMedicine, Journal of Perinatology, and Nature Communications into the daily workflow of the modern hospital, the focus will increasingly shift toward how these digital assistants can be scaled to serve a global patient population.