For millions of adults worldwide, the simple act of rising from a chair or walking to the mailbox is accompanied by the persistent, grinding ache of knee osteoarthritis (OA). As the global population ages, this degenerative condition—characterized by the breakdown of protective cartilage—has become a leading cause of disability. While physical activity has long been prescribed as a primary defense, the medical community has historically struggled to provide patients with a definitive "prescription" for which type of exercise works best.
A landmark study published in The BMJ has finally provided that clarity. Synthesizing data from 217 clinical trials, researchers have concluded that aerobic activity—such as walking, cycling, and swimming—stands as the most effective intervention for managing knee osteoarthritis, offering superior results in pain reduction, physical function, and overall quality of life.
The Silent Epidemic: Understanding Knee Osteoarthritis
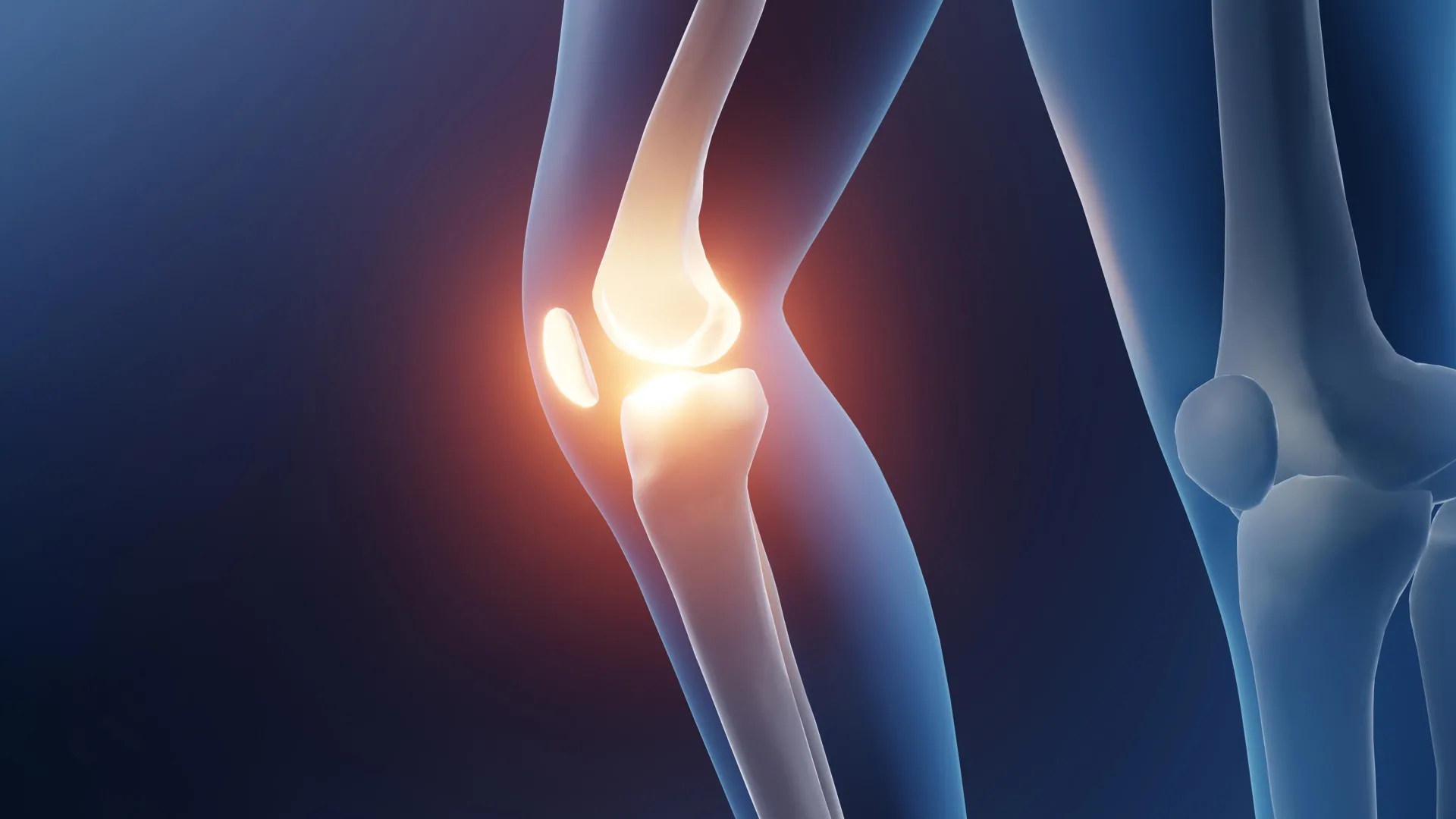
To appreciate the significance of this research, one must understand the pathology of the condition. Knee osteoarthritis is a progressive disease where the articular cartilage—the smooth, rubbery tissue that cushions the ends of bones—gradually erodes. As this protective layer thins, bones begin to rub against each other, leading to chronic inflammation, swelling, and debilitating joint stiffness.
The prevalence of this condition is staggering. Nearly 30% of adults over the age of 45 show radiographic evidence of knee osteoarthritis, and for approximately half of those individuals, the symptoms are severe enough to interfere with daily life. Despite its prevalence, medical guidelines have remained frustratingly vague, often offering general advice to "stay active" without specifying the intensity, duration, or type of exercise that yields the most significant clinical outcomes.
A Comprehensive Chronology: The Evolution of Clinical Evidence (1990–2024)
The quest for a definitive answer led an international team of researchers to conduct one of the most exhaustive reviews in the history of musculoskeletal medicine. Spanning three decades of clinical inquiry, the team analyzed 217 randomized controlled trials conducted between 1990 and 2024.
Phase 1: Data Aggregation and Methodology
The study involved a cohort of 15,684 participants, creating a robust statistical foundation that far outweighs previous smaller-scale analyses. Researchers categorized interventions into several distinct groups:
- Aerobic exercise: Walking, cycling, and swimming.
- Strengthening programs: Resistance training focused on the quadriceps and hamstrings.
- Flexibility exercises: Stretching and range-of-motion routines.
- Mind-body practices: Yoga, Tai Chi, and meditative movement.
- Neuromotor training: Balance and coordination exercises.
- Mixed programs: Hybrid approaches combining multiple modalities.
Phase 2: The GRADE System Assessment
Recognizing that not all clinical trials are created equal, the researchers employed the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) system. This rigorous framework allowed them to weigh the certainty of the evidence, filtering out noise from smaller, lower-quality studies to identify consistent, high-impact clinical trends.
Phase 3: Longitudinal Analysis
The researchers examined outcomes across three critical time horizons:
- Short-term: Four weeks post-intervention.
- Mid-term: 12 weeks post-intervention.
- Long-term: 24 weeks post-intervention.
Supporting Data: Why Aerobic Exercise Reigns Supreme
The study’s most striking finding is the consistency with which aerobic exercise outperformed its counterparts. While other forms of movement are undeniably beneficial, aerobic activity demonstrated a unique ability to address the multifaceted nature of OA.
Pain Reduction and Functional Capacity
The data showed, with moderate certainty, that aerobic exercise provides a dual-action benefit: it reduces pain levels and improves physical function in both the short and mid-term. Unlike strengthening exercises, which may take longer to manifest functional improvements, aerobic activity appears to improve blood flow to the joint and facilitate better mobility through repetitive, low-impact movement.
Gait Performance and Quality of Life
For patients, "function" is not just a clinical metric; it is the ability to walk without a limp and maintain independence. The study revealed that aerobic exercise specifically improves walking ability and overall quality of life. While neuromotor training showed promise in boosting gait performance in the short term, and strengthening programs improved mid-term function, neither offered the same comprehensive, sustained benefits as aerobic training.
Comparative Efficacy
The analysis highlighted that while "mixed" exercise programs are often prescribed, they do not necessarily outperform focused aerobic routines. This suggests that for patients with limited time or energy, prioritizing aerobic activity is a more efficient use of therapeutic effort than attempting a broad, poorly defined mix of exercises.
Official Responses and Clinical Implications
The medical community has greeted these findings as a long-awaited "gold standard" for non-surgical OA management. By providing a clear hierarchy of exercise, the study empowers clinicians to move away from vague recommendations toward evidence-based prescriptions.
The New Clinical Protocol
The researchers explicitly recommend that clinicians adopt aerobic exercise as a "first-line intervention" for patients suffering from knee osteoarthritis. This does not mean that other forms of exercise should be discarded, but rather that they should be positioned as supportive, secondary therapies.
"If a patient can only commit to one form of exercise, the data suggests it should be aerobic," the authors note. However, they are careful to emphasize individualization. If a patient’s unique health profile or physical limitations make swimming or cycling impossible, clinicians should pivot to alternative structured activities, such as mind-body practices or targeted strengthening, which still provide meaningful, safe, and effective relief.
Safety and Long-Term Considerations: A Holistic View
One of the most encouraging findings of the 217-trial review is the safety profile of these interventions. Across all categories, there was no evidence that exercise increased the risk of adverse events compared to sedentary control groups. For years, patients have feared that exercise would "wear out" their joints faster, but this study confirms that movement is, in fact, the best medicine for preserving joint health.
Addressing the Limitations
The researchers were transparent about the study’s limitations. They noted that many of the comparisons between different types of exercise were indirect, as few trials directly pitted "cycling vs. yoga" in a head-to-head format. Furthermore, while the short and mid-term data is exceptionally strong, there is a relative scarcity of 24-week (long-term) data, which makes it difficult to predict the exact maintenance requirements for long-term symptom management.
Future Directions
This study serves as a critical baseline, but it also highlights the need for future research to focus on the long-term adherence to aerobic programs. While the study proves that aerobic exercise works, the real-world challenge lies in ensuring that patients maintain these habits for years, rather than months.
Conclusion: A Paradigm Shift in OA Management
The BMJ study marks a definitive shift in how we approach the treatment of knee osteoarthritis. By validating aerobic exercise as the most effective, safest, and most accessible tool in the clinical toolkit, researchers have provided a roadmap that is both simple and scientifically sound.
For the patient, the message is one of empowerment: the pain of osteoarthritis is not an inevitable sentence to inactivity. By incorporating walking, cycling, or swimming into a daily routine, individuals can regain control over their mobility, reduce their reliance on pain medication, and significantly enhance their quality of life. As healthcare providers begin to integrate these findings into their practice, we can expect a more standardized, effective, and patient-centered approach to one of the most common ailments of the modern age.
Movement, it seems, remains the best medicine—and now, we finally know exactly which movements matter most.