A kidney cancer diagnosis often arrives as a shock, accompanied by a cascade of complex medical terminology, uncertainty, and fear. However, the paradigm of oncological care is shifting. For those facing this diagnosis, understanding the current landscape of treatment—particularly the revolutionary role of immunotherapy—is the first step toward reclaiming agency in the healing process. While the road ahead may seem daunting, patients are increasingly finding hope in a new generation of therapies that work in harmony with the body’s own defense systems.
Main Facts: Understanding Kidney Cancer
Kidney cancer, or renal cell carcinoma (RCC) in its most common form, occurs when cells within the kidneys begin to proliferate uncontrollably, eventually forming a malignant tumor. The kidneys are sophisticated, bean-shaped organs, each roughly the size of a fist. Despite their size, they perform life-sustaining tasks: filtering metabolic waste from the blood, regulating electrolyte balance, managing blood pressure, and stimulating the production of red blood cells.
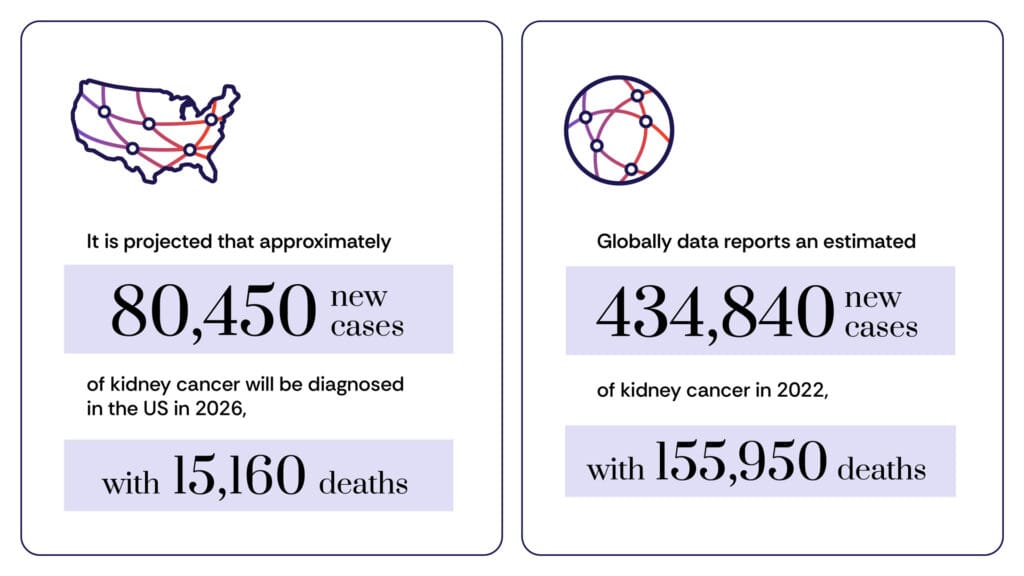
Statistically, kidney cancer ranks among the top ten most prevalent cancers in the United States, accounting for approximately 3% to 5% of all adult malignancies. It is a disease that disproportionately affects older populations, with a median age of diagnosis at 65. Furthermore, epidemiological data consistently shows that men are twice as likely as women to develop the disease, suggesting both hormonal and environmental factors may play a role in its pathogenesis.
The Chronology of Treatment: From Surgery to Precision Medicine
The history of kidney cancer treatment is a narrative of technological and biological progress. For decades, the standard of care was primarily surgical: partial or radical nephrectomy. While surgery remains a cornerstone of treatment, particularly for localized disease, the systemic treatment of metastatic kidney cancer has evolved significantly over time.

- The Early Era: Historically, metastatic kidney cancer was considered highly resistant to traditional chemotherapy and radiation. Outcomes were often bleak, with few systemic options available.
- The Targeted Therapy Shift: The early 2000s introduced "targeted therapies"—drugs designed to interfere with specific molecules involved in tumor growth and blood vessel formation (angiogenesis). These therapies improved survival but often came with significant quality-of-life challenges.
- The Immunotherapy Revolution: Within the last decade, the clinical focus has shifted toward immunotherapy. By manipulating the immune system to recognize cancer cells that previously evaded detection, clinicians have opened a new chapter in oncology. Today, we are in the era of Immune Checkpoint Inhibitors (ICIs), which have fundamentally altered the survival statistics for metastatic patients.
Supporting Data: The Power of the Immune System
Immunotherapy is not merely a drug; it is a strategy to "unmask" the enemy. Cancer cells are notoriously adept at "hiding" from the immune system. They often express proteins that trick T-cells—the body’s "soldiers"—into believing they are healthy cells.
Immunotherapy works by blocking these inhibitory signals. Specifically, ICIs target pathways such as PD-L1 and CTLA4. By effectively releasing the "brakes" on the immune response, these therapies allow the patient’s own immune system to identify, target, and destroy malignant cells.
Encouraging Trends:
While the annual incidence of new kidney cancer diagnoses has steadily climbed, a counter-intuitive and highly positive trend has emerged: mortality rates are declining. This divergence is attributed to earlier detection through diagnostic imaging and the integration of highly effective immunotherapies that allow patients to live with a chronic-like management of the disease rather than a terminal prognosis.
Official Perspectives: The Clinical Reality
Leading oncologists emphasize that while immunotherapy is a breakthrough, it is not a "one-size-fits-all" solution. The decision to pursue immunotherapy is highly personalized.

"The modern approach to kidney cancer is defined by biomarker testing and a deep assessment of the patient’s overall health," notes recent oncology clinical literature. Physicians consider the specific histological subtype of the cancer, the stage of the disease, and the patient’s history of prior treatments.
When asked about the future, researchers are optimistic. The current focus is on "overcoming resistance." Some cancers, while initially responsive to immunotherapy, eventually develop ways to bypass the blockade. Consequently, the research frontier is now occupied by combination therapies—often pairing ICIs with targeted inhibitors or other biological agents—to ensure a more durable response. Furthermore, personalized cancer vaccines and the adaptation of CAR T-cell therapy are being rigorously evaluated in clinical trials, pushing the boundaries of what is possible in precision medicine.
Implications: Navigating the Journey
For the patient and their loved ones, the implication of these medical advancements is clear: education is a vital component of the treatment plan. Being an advocate for one’s own health means asking the right questions. Patients are encouraged to discuss the following with their care teams:
- What is the specific subtype of my kidney cancer?
- Am I a candidate for immunotherapy, and what is the expected profile of side effects?
- Are there active clinical trials that could offer access to next-generation therapies?
- How will we monitor the effectiveness of the treatment over the coming months?
Frequently Asked Questions
How does immunotherapy differ from chemotherapy?
The distinction is fundamental. Chemotherapy relies on cytotoxic drugs designed to kill rapidly dividing cells—an approach that often impacts healthy cells as well, leading to systemic toxicity. Immunotherapy, by contrast, is biological; it modulates the body’s internal defenses. It does not attack the cancer directly; it teaches the immune system to do the work.
Is immunotherapy right for everyone?
Not currently. Because immunotherapy relies on the presence of specific immune markers, it is most effective for those whose tumor microenvironment is "hot" or responsive. However, researchers are working tirelessly to turn "cold" tumors into "hot" ones, potentially expanding the patient pool for these therapies in the near future.
What is the role of clinical trials?
Clinical trials are the engine of progress. By participating in a trial, patients not only gain access to cutting-edge therapies that are not yet available to the general public, but they also contribute to the collective knowledge that saves lives in the future.
Conclusion: A Future Shaped by Hope
The trajectory of kidney cancer care is moving toward greater longevity and a higher quality of life. As researchers refine combination therapies and explore the potential of personalized medicine, the goal is shifting from temporary management to potential long-term control.
If you or a loved one are facing a kidney cancer diagnosis, remember that the landscape is changing for the better. You are not alone in this fight. By engaging with your care team, staying informed about the latest research, and utilizing available support systems, you can approach your treatment with the clarity and confidence required to navigate the journey ahead. The future of kidney cancer treatment is not just about survival; it is about providing every patient with more time, more options, and, most importantly, more hope.