A diagnosis of kidney cancer—medically referred to as renal cell carcinoma (RCC) in its most common forms—often arrives with a profound sense of uncertainty. For patients and their families, the journey from diagnosis to treatment plan can feel overwhelming. However, we are currently living through a paradigm shift in oncology. Thanks to rapid advancements in immunotherapy, the prognosis for many kidney cancer patients has shifted from a narrative of despair to one of manageable, long-term care and renewed hope.
Understanding the Disease: The Basics of Kidney Cancer
Kidney cancer occurs when cells within the kidneys—the two fist-sized, bean-shaped organs located in the retroperitoneum—begin to undergo mutations that lead to uncontrollable growth. These organs are the body’s primary filtration system, working tirelessly to cleanse blood, regulate blood pressure, balance electrolytes, and stimulate the production of red blood cells.
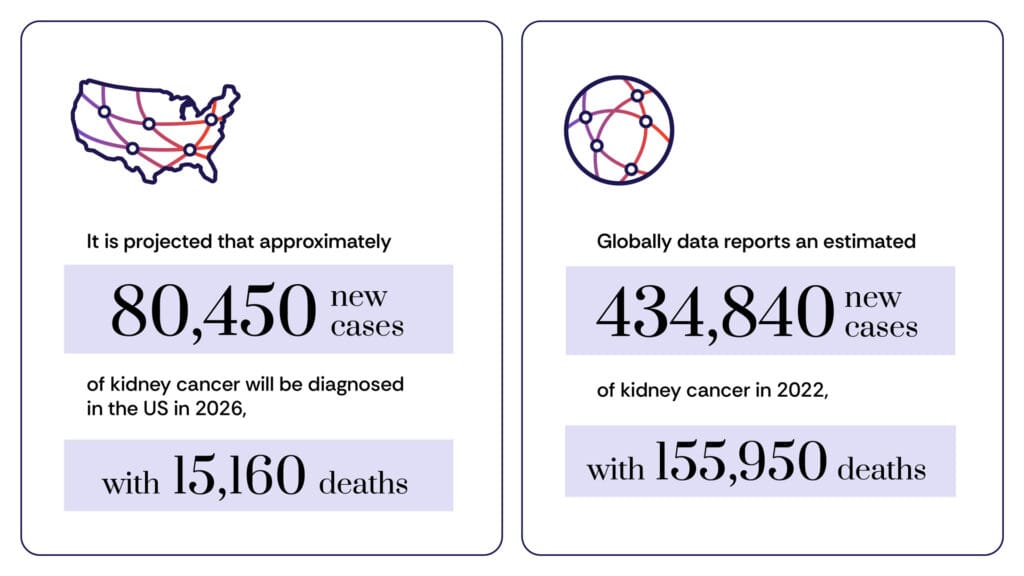
When these cells transform into malignant tumors, they can disrupt these vital homeostatic processes. While kidney cancer accounts for approximately 3% to 5% of all adult cancer diagnoses in the United States, it is a complex condition with multiple histological subtypes. Data indicates a higher prevalence among men and an average age of onset around 65. Despite these statistics, the medical community has observed an encouraging trend: while the incidence of new diagnoses has risen, the mortality rate has steadily declined over the last two decades. This success is largely attributed to earlier detection and the integration of novel systemic therapies.
The Immunotherapy Revolution: A Chronology of Progress
The history of cancer treatment has traditionally relied on the "three pillars": surgery, radiation, and chemotherapy. However, the last decade has ushered in the era of the "fourth pillar"—immunotherapy.
The Early Days: Cytokines
Before the modern era of precision medicine, treatment for advanced kidney cancer was limited. In the 1980s and 90s, scientists utilized cytokines—specifically interleukin-2 (IL-2) and interferon-alpha. While these treatments were the first to prove that the immune system could be harnessed to fight kidney cancer, they were notoriously difficult for patients to tolerate, often causing severe systemic toxicity.

The Targeted Therapy Era
In the early 2000s, the focus shifted to targeted therapies, such as tyrosine kinase inhibitors (TKIs). These drugs were designed to starve tumors of their blood supply. While effective, they rarely resulted in durable, long-term remissions.
The Checkpoint Inhibitor Breakthrough
The true turning point arrived with the development of immune checkpoint inhibitors (ICIs). Scientists discovered that cancer cells often exploit "brakes" on the immune system—proteins like PD-1, PD-L1, and CTLA-4—to hide from T-cells. By developing monoclonal antibodies to block these checkpoints, researchers essentially "took the brakes off" the immune system, allowing the body’s own natural defenses to identify and eradicate malignant cells. This era has redefined the survival benchmarks for metastatic renal cell carcinoma.
Supporting Data: Why Immunotherapy Matters
The clinical impact of immunotherapy is best illustrated through recent trial data. In studies involving patients with advanced RCC, the combination of checkpoint inhibitors (such as nivolumab and ipilimumab) has shown significant improvements in overall survival compared to historical standards of care.
According to major oncological research institutions, the benefits of these therapies include:
- Durable Responses: A subset of patients experiences long-term disease control that persists even after the cessation of therapy.
- Improved Quality of Life: While immunotherapy has its own unique side-effect profile, many patients report a higher quality of life compared to the systemic exhaustion associated with traditional cytotoxic chemotherapy.
- Combination Efficacy: Modern protocols now frequently combine immunotherapy with targeted agents, creating a multi-pronged attack that hinders tumor growth while simultaneously supercharging the immune response.
Official Perspectives and Expert Consensus
Leading oncology organizations, including the American Society of Clinical Oncology (ASCO) and the Cancer Research Institute, emphasize that immunotherapy is not a "one-size-fits-all" solution.

"The landscape is moving toward personalization," says a lead researcher at a major cancer center. "We are no longer just looking at the stage of the cancer; we are looking at the molecular signature of the tumor to predict who will respond best to specific immunotherapeutic agents."
Medical boards currently stress the importance of biomarker testing. By evaluating the tumor microenvironment, doctors can better predict whether a patient will respond to ICIs or if they require a combination of immunotherapy and anti-angiogenic agents. The consensus among the medical community is clear: patient outcomes are optimized when treatment is tailored to the individual’s biological and clinical profile.
Clinical Implications: The Road Ahead
The integration of immunotherapy into the standard of care has profound implications for the future of kidney cancer management.
1. Moving Toward Adjuvant Therapy
Research is currently moving beyond the metastatic setting. New trials are investigating whether immunotherapy can be used as an "adjuvant"—a treatment given after surgery to clear any remaining microscopic cells and prevent recurrence. Early data suggests that this approach could drastically reduce the rate of relapse in high-risk patients.
2. Overcoming Resistance
A significant challenge in current research is "primary resistance," where some tumors do not respond to initial immunotherapy. Ongoing clinical trials are testing novel combination therapies, including vaccines that train the immune system to recognize specific tumor antigens, and CAR T-cell therapies, which involve re-engineering a patient’s own immune cells in a laboratory setting before re-infusing them into the body.
3. Improving the Patient Experience
Future research is also prioritizing the mitigation of immune-related adverse events (irAEs). As we learn more about how to manage these side effects, the treatment process becomes safer, allowing for longer durations of therapy and better patient adherence.
Empowering the Patient: A Guide to Advocacy
If you or a loved one has been diagnosed with kidney cancer, the sheer volume of information can be daunting. Advocacy starts with education. Here are the essential steps to navigating your diagnosis:
- Become an Expert on Your Case: Understand the subtype of your kidney cancer (e.g., clear cell vs. papillary) and its stage. This information determines which treatments are most likely to be effective.
- The Power of the Second Opinion: Kidney cancer management is rapidly evolving. Ensure your care team is up-to-date with the latest clinical trial data and immunotherapy protocols.
- Ask the Right Questions: When meeting with your oncologist, consider asking:
- "Is immunotherapy an option for my specific stage and histology?"
- "What are the potential side effects, and how will we monitor them?"
- "Are there any clinical trials currently enrolling that might be a better fit than standard-of-care options?"
- Utilize Support Networks: Cancer is a psychosocial journey as much as a physical one. Engaging with patient support groups can provide emotional resilience and practical insights into living with treatment.
Frequently Asked Questions
How does immunotherapy differ from chemotherapy?
While chemotherapy works by introducing toxic chemicals into the body to kill rapidly dividing cells—often damaging healthy cells in the process—immunotherapy works by stimulating the body’s endogenous immune system. It trains the body to recognize the cancer as a threat, which often leads to more durable, long-term responses.
Is immunotherapy effective for all kidney cancer patients?
Not currently. Immunotherapy is highly effective for a specific subset of patients, particularly those with advanced renal cell carcinoma. However, researchers are working hard to expand its reach by finding ways to make "cold" tumors (those that don’t trigger an immune response) "hot" (those that the immune system can see).
What is the "future" of kidney cancer treatment?
The future lies in the integration of AI-driven diagnostics, personalized cancer vaccines, and the combination of metabolic therapies with immunotherapy. The goal is to move away from generic treatment plans toward a future where every patient receives a therapy specifically mapped to their tumor’s unique genetic sequence.

Conclusion: A Future Defined by Hope
The narrative surrounding kidney cancer has undergone a remarkable transformation. Where there was once a reliance on harsh, non-specific treatments, there is now a sophisticated, growing toolkit of immunotherapies that are saving lives.
For those navigating this diagnosis, remember: you are not a statistic. You are an individual with access to an unprecedented level of medical innovation. By staying informed, advocating for yourself, and leaning into the expertise of your clinical team, you can approach your treatment with the confidence that you are on the cutting edge of modern medicine. The ongoing commitment of researchers worldwide ensures that, with each passing year, the options grow, the side effects diminish, and the promise of a longer, healthier life becomes a reality for more patients than ever before.




















